
GOTS Master's week in Luxembourg 🇱🇺
20/11/2025
The GOTS Master's week, coordinated by Dr.Nührenbörger, took place in Luxembourg throughout last week. Several LIROMS members and collaborators were actively involved, delivering high-level teaching and sharing their expertise with participants.🔒Camille Tooth delivered a presentation within the Sports Medical Care for Children and Adolescents session, highlighting key principles of Protection and Safety (Safeguarding).📚 Dr Romain Seil led a session on ligament injuries, sharing essential perspectives on mechanisms and management.🏥 Caroline Mouton presented the ACL clinical pathway, detailing a clear and structured approach from diagnosis to return to sport.Participants had the opportunity to visit the Sport Fabrik as part of the week’s continuation, where additional sessions were held in collaboration with the Luxembourg Institute for High Performance in Sports and LIROMS.🏃♀️Jennifer Fayad offered an insightful presentation on the kinematics and kinetics of running.📐 Tiago Neto conducted a practical workshop on isokinetic and dynamometric assessment.

Congratulations to Yana Feller for her thesis : From Trauma to Rehabilitation: How Can Elite Volleyball Players Safely Return to Training After an ACL Injury?
20/10/2025
You will find below a summary of Yana Feller's Master thesis from the 'Technische Universitat München Fakultät für Sport- und Gesundheitswisssenschaften' From Trauma to Rehabilitation: How Can Elite Volleyball Players Safely Return to Training After an ACL Injury?An anterior cruciate ligament (ACL) tear is among the most severe injuries in competitive sports. Volleyball athletes are particularly affected, as the sport demands frequent jumping, abrupt landings, and rapid changes of direction. The consequences are far-reaching: long recovery times, psychological strain, and an elevated risk of subsequent injuries. This complex journey back to the court was the central focus of a study that examined how athletes can safely return to training and competition after an ACL rupture.The ACL, whether anterior or posterior, plays a crucial role in knee stability. It prevents dislocations, controls rotational movements, and, through embedded receptors, provides vital information for muscular coordination. The consequences of a torn ligament are therefore severe. Diagnosis is typically based on clinical tests such as the Lachman or Pivot-shift test, complemented by imaging techniques like MRI. ACL tears often occur alongside other injuries, for instance to the meniscus or collateral ligaments.The causes can vary. For young female athletes, hormonal factors and anatomical structures such as a steeper tibial plateau slope play a role, while for men, intensity of load and technique are more influential. Further aspects such as hall floor and footwear also contribute. Interestingly, most injuries occur during competition rather than during training, largely due to higher intensity and stress. Women are affected more frequently overall, which is attributed primarily to hormonal and anatomical differences.Successful treatment involves multiple dimensions. While conservative approaches aim to restore stability through muscle strengthening, surgery remains the standard for elite athletes. ACL reconstruction is widely established, though newer techniques such as internal bracing are rising. Regardless of the method chosen, rehabilitation is decisive. It progresses through phases: restoring mobility, building strength, training coordination, and finally reintegrating sport-specific movements. For volleyball players, this means targeted jump and landing drills, block and attack simulations, and gradually returning to game-like situations. Nutrition also plays an important role—adequate protein supports muscle building, while vitamin C and omega-3 fatty acids promote healing. Preventive programs such as FIFA 11+ or plyometric exercises have been shown to significantly reduce the risk of re-injury.A study I conducted with 45 elite volleyball players highlights the significance of this issue. The average age at the first injury was just 19.5 years—a stage when many athletes are only beginning to advance into higher leagues. Most injuries occurred in competition, typically without contact from opponents, and almost always during landings after attacks or blocks. Around 87% opted for surgery after their first rupture, but many required further procedures. Accompanying injuries were also frequent: 80% had additional damage to the meniscus or collateral ligaments.Rehabilitation outcomes varied widely. While some players returned to the court after six to nine months, others needed over a year. Four athletes had to end their careers entirely. Even after completing rehabilitation, 78% still reported pain, restricted mobility, or instability in the knee. Only a small minority sought psychological support, though the mental burden was frequently described as particularly high.The findings make clear that a safe return to volleyball training can only be achieved through a holistic approach. This includes individually tailored rehab plans, regular performance assessments, targeted prevention programs, and psychological support. The decision to resume training should not be based solely on elapsed time but on objective criteria such as strength, stability, movement quality, and mental readiness.In conclusion, ACL ruptures represent not only a medical issue but also a sporting and psychological challenge. Long-term athletic performance requires an integrated approach combining medicine, physiotherapy, training, prevention, and mental coaching. Only such a comprehensive strategy ensures that athletes can return to the court not just quickly, but above all safely.

Congratulations to Dr. Alexis Lion!
05/10/2025
Dr. Alexis Lion has been appointed Chair of the HEPA Europe Network (2025–2027). Alexis holds an MSc and PhD in Life and Health Sciences from the University of Lorraine and serves as Director of a sports federation for people with chronic diseases (FLASS – www.sport-sante.lu) in the Grand Duchy of Luxembourg. In this capacity, he coordinates and promotes therapeutic physical activity programs aimed at improving health and well-being. Alongside his administrative and advocacy roles, Alexis contributes to research in various domains, including neuroscience, sports medicine, sports sciences, and public health. His primary research focus lies in the promotion of physical activity within health care settings, a field in which he has been actively involved through the HEPA Europe Working Group on HEPA promotion in health care settings. His appointment as Chair of the HEPA Europe Network (https://www.who.int/europe/groups/hepa-europe-(european-network-for-the-promotion-of-health-enhancing-physical-activity)) reflects his continued commitment to advancing evidence-based strategies that foster active and healthy living across Europe.

Open position : Administrative assistant
07/08/2025
We are hiring a administrative assistant - Part time (50% FTE) More info: https://www.linkedin.com/posts/liroms-asbl_administrative-assistant-job-description-activity-7359137227982938112-1qk3?utm_source=share&utm_medium=member_desktop&rcm=ACoAAC1lij4BhT9Djhkq2RWanTsBgmJaTCV16qQ

HR News
01/08/2025
🔔 Latest Team News : We are excited to officially welcome Andréas Tamang to the Liroms team ! After a successful 6 months internship within the Human Motion Lab we are very happy to have him on board as ‘Biomechanical and biomedical engineer in sports medicine and surgery’ 👏

Liroms is looking for 2 postdoctoral researchers
29/07/2025
LIROMS is looking for two postdoctoral researchers to join exciting projects based in Luxembourg: 1️⃣ One focused on mental health in sport 2️⃣ One exploring sports policy and performance More information : https://www.linkedin.com/feed/update/urn:li:activity:7355963136685867009 If you're interested, or know someone who might be, feel free to reach out or share within your network! Please send your CV and cover letter to info@liroms.lu no later than September 8th, 2025.

E-MOTION: Protecting the mental health of young athletes in the age of social media
18/07/2025
A new project is being launched within LIROMS!Social media is omnipresent in the lives of young people, including young athletes. In response to the risks associated with hyper-connectivity, such as cyberbullying, social pressure and loss of self-esteem, a new research and prevention project is being launched in Luxembourg under the coordination of LIROMS (Luxembourg Institute of Research in Orthopaedics, Sports Medicine and Science).Entitled ‘Impact of social media on the mental health of young athletes: longitudinal monitoring and prevention interventions’, this project is aimed at athletes aged 12 to 18, in partnership with Sportlycée, ALAD, INAPS and the ReFORM network, and is supported by the Oeuvre Nationale de Secours Grande-Duchesse Charlotte. The objective is twofold: to better understand the effects of digital interactions on the psychological well-being of young athletes, and to propose concrete, educational and technological solutions to address them.The project will run for two years and will consist of several components: longitudinal monitoring of young athletes, awareness-raising and digital education workshops, and the creation of a digital platform containing appropriate resources. The results will not only equip young athletes, but also enable recommendations to be made to sports federations, schools and policymakers to strengthen the protection of young people in an increasingly digital environment.📍 Follow us to find out about the next steps, the resources available and the partners involved in this initiative!Project managers: Katy Seil-Moreels, Camille Tooth With the support of OEUVRE Nationale de Secours Grande-Duchesse Charlotte https://www.oeuvre.lu/fr

The CHL Sports Clinic has once again been certified as a Luxembourg Olympic Medical Centre by the COSL
03/07/2025
Press release from the Luxembourg Olympic and Sports Committee (COSL) concerning the recertification of the Luxembourg Olympic Medical Centre (CMOL): The Luxembourg Olympic and Sports Committee (COSL) has reconfirmed the award of the Luxembourg Olympic Medical Centre (CMOL) label to the Sports Clinic of the Centre Hospitalier de Luxembourg-Clinique d'Eich (CHL) following a rigorous recertification process. This label, initially awarded in 2008, attests to the clinical, scientific and educational excellence of the Sports Clinic and its ongoing commitment to international standards in sports medicine. The centre offers recognised expertise in the monitoring of elite athletes, particularly in collaboration with the Luxembourg Institute for High Performance in Sports (LIHPS), but also in the care of patients of all levels facing issues related to physical activity. Thanks to its interdisciplinary approach, specialised equipment and highly qualified medical team, the Cliniquedu Sport in Eich performs more than 35,000 outpatient consultations and 2,300 surgical procedures each year. The centre also plays a central role in providing medical coverage for major COSL events such as the Olympic Games and the Games of the Small States of Europe (GSSE), while ensuring regular monitoring of COSL sports executives, Sportlycée students and athletes monitored by LIHPS. During these major events, the care of athletes also benefits from the good relations and close collaboration between CMOL doctors and their counterparts from other neighbouring Olympic committees, such as the Deutscher Olympische Sportbund (DOSB). On a scientific level, the Sports Clinic is continually strengthening its collaborations, notably with the Luxembourg Institute of Research in Orthopaedics, Sports Medicine and Science (LIROMS), a member of the French-speaking ReFORM networkrecognised by the International Olympic Committee (IOC). Together, they actively contribute to research in fields as diverse as clinical biomechanics, injury prevention, mental health in athletes, orthopaedics and sports cardiology. This pooling of expertise is complemented by the presence at the Eich site of the ESSKA (European Society of Sports Traumatology, Knee Surgery and Arthroscopy), the most representative learned society in sports orthopaedics inEurope. Numerous collaborations stem from the presence and proximity of these various medical and scientific entities, thus contributing to Luxembourg's international reputation. The COSL is delighted to be able to continue this fruitful collaboration with the team at the CHL Sports Clinic, serving the health and performance of Luxembourg's athletes.

Book your appointment online at the HML
02/06/2025
The Human Motion Lab is now available on Doctena! You can find us there to book your gait/ running analysis : https://www.doctena.lu/en/movement-analysis/luxembourg

GOTS – JSOA – KOSSM Fellowship Visit and Symposium in Luxembourg 2025
30/05/2025
Since 1991, the German-speaking Society for Orthopedic and Traumatological Sports Medicine (Gesellschaft für Orthopädisch-Traumatologische Sportmedizin, www.GOTS.org) in collaboration with the Korean Society of Sports Medicine (KOSSM) and the Japan Sports Orthopaedic Association (JSOA), has organized a travel fellowship aimed at fostering cultural and professional exchange among physicians and scientists from the three societies. Serving as a bridge between continents, this program promotes international collaboration and mutual learning in the field of sports orthopaedics. Following last year’s visit of GOTS members to Japan and South Korea, the CHL Sports Clinic, in collaboration with LIROMS, had the pleasure of welcoming this year’s fellows: Dr. Du-Han Kim and Dr. Du Hyun Ro from South Korea, and Dr. Hideaki Nagamoto and Prof. Dr. Seikai Toyooka from Japan. From May 30 to June 2, the team led by Dr. Christian Nührenbörger and Prof. Dr. Romain Seil hosted an engaging and diverse program that blended medicine, science, sports, culture, and national heritage. The visit began on Friday with a tour of the CHL Sports Clinic and the LIROMS Human Motion Lab, where Prof. Dr. Jan Cabri shared valuable insights into the lab’s research and technology. Saturday included a guided tour by Alwin de Prins, director of the Luxembourg Institute for High Performance in Sports (LIHPS), through the High Performance, Training and Recovery Center (HPTRC) at the COQUE, followed by a visit to the LIHPS Biomechanical Movement Laboratory, SportFabrik, in Differdange. Here, the fellows learned about Luxembourg’s elite athlete development and the integrated rehabilitation and performance services provided to top-level athletes. In the afternoon, the group explored the City of Science and the historic Blast Furnace Belval, and later experienced the vibrant atmosphere of the ING Night Marathon in Luxembourg City. On Sunday, the fellows enjoyed a behind-the-scenes tour of the Philharmonie Luxembourg and a guided walk through Luxembourg’s historic old town, rounding off the day with a relaxed barbecue evening. Monday focused on clinical and academic exchange, including operating room sessions with insights into our meniscus repair and ACL reconstruction techniques. The program concluded with a scientific symposium featuring current research and discussions. At this symposium, the four fellows presented their clinical and scientific work, offering valuable insights into current research and innovative treatment approaches from their countries. The local team was represented by Dr. Esfandiar Chahidi, who spoke about ACL injury severity and knee decompensation, and Dr. Tiago Neto, who highlighted importance of biomechanical analysis in the return to sport process following an ACL injury. Additionally, Amanda Magosch shared her personal experiences from last year’s GOTS fellowship in Japan and South Korea. We were truly honored to host our international colleagues and are grateful for the enriching conversations, shared knowledge, and new friendships formed. A heartfelt thank you to all supporters, organizers, and partners who made this inspiring exchange possible. https://drive.google.com/file/d/1pEehSlFN1t2tPdUOjmKV6mF8S5cTG1qn/view

25th Annual Conference 2025 of the Society for Paediatric Sports Medicine
16/03/2025
The 25th Annual Conference of the Society for Paediatric Sports Medicine (www.kindersportmedizin.org) took place in Luxembourg from the 14th to the 16th of March, 2025. More than 80 participants came to the Museum of Contemporary Art, MUDAM, in Luxembourg to celebrate the 25th anniversary. The conference president Tobias Stadtfeld, paediatrician and sports physician in Luxembourg, put together a compelling and top-class programme featuring 30 lectures and two hands-on workshops on the topic of ‘Young athletes’, made possible in part by the support of LIROMS. The conference was jointly opened by the Luxembourg Minister of Health and Social Security, Martine Deprez, and the Luxembourg Minister of Sport, Georges Mischo. The topic of the first day was ethics and psychology as well as safeguarding in child and youth sport. National and international concepts in the field of child protection in sport were presented and discussed, followed by an explanation of the topic of nutritional supplements and doping prevention. The second day begun with a practical workshop on fracture sonography in growing children. The programme continued with two sessions organised by the GOTS Paediatric Sports Orthopaedics Committee, including two LIROMS members, Prof. Romain Seil and Dr Christian Nührenbörger, as well as their colleagues Dr Felix Hoffmann and Dr José Azzolin from the CHL Sports Clinic in Luxembourg. The first session provided an update on sports orthopaedic pathologies of the knee joint in children and adolescents. The second GOTS session opened with a presentation on the prevention of sports injuries in young athletes and proceeded with updates on the treatment of concussions and special sports orthopaedic cases in children. On Saturday afternoon, the focus shifted to sports science contributions from the fields of cycling and endurance sports. The day concluded with a keynote lecture by Prof. Helge Hebestreit on the 25-year history of the Society for Paediatric Sports Medicine. The third and final day of the conference began actively with a workshop on return-to- competition after anterior cruciate ligament injury, led by physiotherapists Nina Goedert and Ben Moes from Luxembourg. The second session on sports science focused on key topics including overtraining, dealing with heat, and the psychiatric aspects of adolescence. To conclude the 25th annual conference, representatives of the DGPK's paediatric sports cardiology working group presented fascinating insights into the physiological reactions of children with heart defects at altitude and underwater. In line with the motto ‘25 years of Society for Paediatric Sports Medicine - 25 years of a moving future’, all participants were able to enjoy an engaging and inspiring weekend in the extraordinary atmosphere of the MUDAM. The event fostered many open and appreciative discussions and provided valuable opportunities to build networks for the coming years - amongattendees, LIROMS, the GOTS Pediatric Sports Orthopaedics Committee, and the Society for Paediatric Sports Medicine alike. Text: Dr Christian Nührenbörger Photos: Tobias Stadtfeld

2025 Academie Programme
12/02/2025
Programme of the 2025 sports science lectures is online We are proud to present this year’s calendar of sports medicine, sports physiotherapy and sports science lectures, in collaboration with our partners the Luxembourg Institute for Hight Performance in Sports (LIHPS), the Centre Hospitalier de Luxembourg (CHL), the Comité Olympique et Sportif Luxembourgeois (COSL), the Société Luxembourgeoise de Kinésithérapie du Sport (SLKS), the Société Luxembourgeoise de la Médecine du Sport (SLMS) and the Ministry of Sport (MSP). You may subscribe to the newsletter for all eventual updates and information here. Link to the programme

Welcome to our new collaborator !
01/01/2025
On January 1st, Camille Tooth joined Liroms as a scientific project coordinator. She is a sports physiotherapist as well as strength and conditionning coach. She obtained a PhD in Motor Sciences from the University of Liège in 2022, focusing on the critical analysis of current assessment tools for the sporting shoulder. She currently serves as the Scientific Coordinator of the ReFORM network (IOC Research Center). Her professional experience includes roles as a physiotherapist for the French-speaking Belgian Swimming Federation and National Team as well as collaborations with different sports federations and/or clubs in Belgium (tennis, handball, volleyball, rugby for example). She’s been Associate Professor in the Department of Physical Activity and Rehabilitation Sciences of the University of Liège until December 2024. Her research work, includes studies on shoulder injuries in athletes but mainly focus on prevention in general.

Methods for recording and reporting of epidemiological data in tennis: ReFORM synthesis of the International Olympic Committee Consensus Statement
04/12/2024
C. Tooth, J. Cabri, P. Tscholl, F. Bieuzen, M.-A. Démaret, F. Petrot, P. EdouardMéthodes d’enregistrement et de recueil des données épidémiologiques sur les blessures et les maladies dans le tennis : synthèse ReFORM de la position de consensus du Comité international olympiqueJournal de Traumatologie du Sport,Volume 41, Issue 4,2024, Pages 405-408, ISSN 0762-915X,https://doi.org/10.1016/j.jts.2024.05.005.(https://www.sciencedirect.com/science/article/pii/S0762915X24000858) Link to the article: 10.1016/j.jts.2024.05.005

Great success for the Sportmedica Congress Exercise and Medicine - 20 years Sports Clinic CHL
25/11/2024
Thank you to all the participants, the speakers, the organizers and the sponsors !

8th International Congress "SPORTMEDICA - Exercise and Medicine – 20 Years Sports Clinic CHL" on 22nd and 23rd November 2024 in Luxembourg
22/11/2024
On November 22 and 23, 2024, the congress "SPORTMEDICA - Exercise and Medicine – 20 Years Sports Clinic CHL" took place at d’COQUE in Luxembourg. "SPORTMEDICA" is an international sports medicine congress, organized every Olympic year by the Luxembourg Society for Sports Physiotherapy (Société Luxembourgeoise de kinésithérapie du sport - SLKS) and the Luxembourg Society for Sports Medicine (Société Luxembourgeoise de médecine du sport - SLMS). This marked the 8th iteration of the event. It was held under the patronage of the Training Academy for Sports Medicine, Sports Physiotherapy, and Sports Sciences in collaboration with its partners, including the Luxembourg Institute of Research in Orthopedics, Sports Medicine, and Science (LIROMS), the Luxembourg Olympic Medical Center (CMOL) of the Centre Hospitalier de Luxembourg (CHL), the Luxembourg Institute for High Performance in Sports (LIHPS), and the Ministry of Sports. This year’s congress also served as the anniversary celebration for the CHL Sports Clinic, which was established 20 years ago as Luxembourg’s first clinical and research-oriented sports medicine institution. Over two decades, the Sports Clinic has gained extensive experience in patient and athlete care and has spearheaded the Training Academy's organization of over 200 colloquia, sports medicine symposia, congresses, and workshops. An outstanding feature of this year's congress was the large industry exhibition with a total of 19 sponsors. It provided participants with up-to-date information and enabled valuable networking, strengthening relationships within the sports medicine community. The organizers once again attracted a host of internationally and nationally renowned experts to present on various current topics in sports medicine. The main themes for 2024 included sports cardiology, the treatment and prevention of sports injuries, mental health, as well as performance physiology and training management. The congress commenced on Friday afternoon with presentations from Prof. Jürgen Scharhag (Vienna), Prof. Tim Meyer, Dr. Lothar Schwarz (both from Saarbrücken), and Prof. Axel Urhausen (Luxembourg) on current issues in sports cardiology, such as sudden cardiac death, sports medicine challenges in triathlon and overtraining. This was followed by official welcome addresses by CHL Director General Dr. Martine Goergen and COSL President André Hoffmann. The next session featured lectures by Dr. Christian Nührenbörger (Luxembourg) on the challenges of injury prevention in sports, Prof. Lars Engebretsen (Oslo/Lausanne) on his 15 years of experience as head of the IOC Medical Commission, Prof. Martin Engelhardt (Osnabrück) on the health consequences of physical inactivity in society, Prof. Stefan Nehrer (Vienna) on the future of sports orthopedics training, and Prof. Romain Seil (Luxembourg) and Camille Tooth (Liège) on the activities of ReFORM, the French-speaking IOC research centers. The first day concluded with a communal dinner. The Saturday morning session focused entirely on anterior cruciate ligament (ACL) injuries. Presentations by Prof. Romain Seil, Dr. Caroline Mouton, Jérôme Pauls, and Nina Goedert (all from Luxembourg), as well as Dr. Anouk Urhausen (Oslo) and Dr. Thomas Patt (Deft), highlighted the latest developments in therapy, rehabilitation, return-to-sport, and prevention of this severe sports injury. This was followed by five theoretical and practical workshops covering leadership in clinical practice (Prof. Nicol van Dyk, Dublin), blood flow restriction training (team led by Ben Moes, Luxembourg), implementation of preventive measures (Aude Aguilaniu, Liège, and Jérôme Pauls), blood lactate analysis in endurance sports (Frédéric Margue and Eric Besenius, Luxembourg), and safeguarding in sports (Dr. Katy Seil, Michelle Tousch, Laura Hoffmann, and Loïc Hoscheit, Luxembourg). In the final session, updates were provided on cartilage injuries by Prof. Henning Madry (Homburg), optimal rehabilitation of hamstring injuries by Nicol van Dyk, and the pros and cons of carbon running shoes by Priv.-Doz. Dr. Casper Grim (Osnabrück). The congress concluded with a fascinating and insightful lecture by Dr. Rolf-Michael Krifter (Graz) on his sports medicine experiences supporting the Dakar Rally. All attendees gained current and practical sports medicine knowledge, which was further deepened through stimulating discussions and workshops. With more than 225 participants from 8 countries, including physicians, physiotherapists, trainers, sports scientists, athletes, and other members of the Luxembourg sports community, the congress was a great success.

Meniscus travelling fellowship
18/11/2024
The Meniscus Group is thrilled to introduce the Meniscus travelling fellowship, a unique opportunity for young Orthopaedic surgeons to deepen their expertise in meniscus science & surgery accross Europe and Asia. https://the-meniscus.org/
New issue of the Journal ARTHROSKOPIE on complex knee surgery in ACL injured knees co-edited by LIROMS president
14/10/2024
https://link.springer.com/journal/142/volumes-and-issues/37-5 The days of meniscectomy and isolated reconstruction of the anterior cruciate ligament are long gone. Nowadays, joint-preserving knee surgery includes the entire portfolio of (multi)ligament reconstructions, multidimensional osteotomies, reconstruction of complex meniscus injuries, meniscus replacement as well as differentiated cartilage therapy and patellar stabilisation procedures. Complex clinical pictures often require a combination of these surgical procedures in order to achieve the best possible result for the patient. The basis of complex interventions is dedicated clinical and imaging diagnostics in order to fully understand the pathologies and treat them individually accordingly. A misinterpretation of the findings can ruin the surgical result in the long term or even worsen the original pathology. Conversely, the surgeon's overly generous approach can also harm the patient. In issue 5, volume 37 of the ARTHROSKOPIE journal, various articles deal with the indications and techniques of combination procedures at the knee joint. From cartilage surgery to meniscus and ligament surgery to double-level osteotomies, readers will get a good overview of the topic of these often complex clinical situations and advanced surgical procedures. Dr. med. Elmar Herbst, PhD University of Münster, Germany Prof. Dr. med. Romain Seil Luxembourg Link to the article

Successful doctoral thesis defense by former LIROMS collaborator
11/10/2024
LIROMS is proud to announce that on the 10th of October, our former collaborator Anouk URHAUSEN was successful in defending her PhD thesis at the Norwegian School of Sport Science in Oslo. During the last 4 years, Anouk has been a PhD student in the Department of Sports Medicine and studied the 10-year outcomes after surgical and non-surgical treatment in patients with anterior cruciate ligament rupture. This project was part of the Delaware-Oslo ACL Cohort Study. The main goal was to assess the long-term results after nonoperative and surgical management of anterior cruciate ligament injury. The complete title of her thesis is: After a decade of the Delaware-Oslo ACL Cohort treatment algorithm: Measurement properties and outcomes after reconstruction or rehabilitation alone for anterior cruciate ligament injury and can be downloaded here. Congratulations, Dr. Anouk!

Welcome to our new collaborator
01/10/2024
Dr. Katy Moreels-Seil is joining LIROMS as a consultant for our projects on mental health in sports. Dr. Moreels is a child and adolescent psychiatrist and systemic and family psychotherapist. She studied medicine at the Catholic University of Louvain (Belgium) and trained as a specialist in Belgium and Luxembourg. She has been in private practice for over 20 years in Luxembourg, where she has also acquired extensive experience in psychosocial structures. For over a decade she has been particularly interested in psychopathology and the treatment of athletes. She is a member of the medical committee of the COSL and a consultant to the LIHPS.

Save the date for the next GOTS Annual Congress 15 -17 May 2025
16/09/2024
More information: https://gots-kongress.org/

A new patient-reported outcome measure for the evaluation of ankle instability: description of the development process and validation protocol
11/09/2024
Spennacchio P, Senorski E.H, Mouton C, Seil R, Cabri J, Karlsson J. A new patient-reported outcome measure for the evaluation of ankle instability: description of the development process and validation protocol. J Orthop Surg Res 19, 557 (2024). https://doi.org/10.1186/s13018-024-05057-4 Background Acute ankle sprains represent one of the most common traumatic injuries to the musculoskeletal system. Many individuals with these injuries experience unresolved symptoms such as instability and recurrent sprains, leading to chronic ankle instability (CAI), which affects their ability to maintain an active lifestyle. While rehabilitation programs focusing on sensorimotor, neuromuscular, strength and balance training are primary treatments, some patients require surgery when rehabilitation fails. A critical analysis of the patient-reported outcome tools (PROs) used to assess CAI surgical outcomes raises some concerns about their measurement properties in CAI patients, which may ultimately affect the quality of evidence supporting current surgical practice. The aim of this research is to develop and validate a new PRO for the assessment of ankle instability and CAI treatment outcomes, following recent methodological guidelines, with the implicit aim of contributing to the generation of scientifically meaningful evidence for clinical practice in patients with ankle instability. Methods Following the Consensus-based Standards for the selection of Health Measurement Instruments (COSMIN), an Ankle Instability Treatment Index (AITI) will be developed and validated. The process begins with qualitative research based on face‒to‒face interviews with CAI individuals to explore the subjective experience of living with ankle instability. The data from the interviews will be coded following an inductive approach and used to develop the AITI content. The preliminary version of the scale will be refined through an additional round of face‒to‒face interviews with a new set of CAI subjects to define the AITI content coverage, relevance and clarity. Once content validity has been examined, the AITI will be subjected to quantitative analysis of different measurement properties: construct validity, reliability and responsiveness. Discussion The development of AITI aims to address the limitations of existing instruments for evaluating surgical outcomes in patients with CAI. By incorporating patient input and adhering to contemporary standards for validity and reliability, this tool seeks to provide a reliable and meaningful assessment of treatment effects. Link to the article

Multiligament knee injury (MLKI): an expert consensus statement on nomenclature, diagnosis, treatment and rehabilitation
07/09/2024
Murray IR, Makaram NS, Geeslin AG, et al Multiligament knee injury (MLKI): an expert consensus statement on nomenclature, diagnosis, treatment and rehabilitationBritish Journal of Sports Medicine Published Online First: 05 September 2024. doi:10.1136/bjsports-2024-108089 Abstract Multiligament knee injuries (MLKIs) represent a broad spectrum of pathology with potentially devastating consequences. Currently, disagreement in the terminology, diagnosis and treatment of these injuries limits clinical care and research. This study aimed to develop consensus on the nomenclature, diagnosis, treatment and rehabilitation strategies for patients with MLKI, while identifying important research priorities for further study. An international consensus process was conducted using validated Delphi methodology in line with British Journal of Sports Medicine guidelines. A multidisciplinary panel of 39 members from 14 countries, completed 3 rounds of online surveys exploring aspects of nomenclature, diagnosis, treatment, rehabilitation and future research priorities. Levels of agreement (LoA) with each statement were rated anonymously on a 5-point Likert scale, with experts encouraged to suggest modifications or additional statements. LoA for consensus in the final round were defined ‘a priori’ if >75% of respondents agreed and fewer than 10% disagreed, and dissenting viewpoints were recorded and discussed. After three Delphi rounds, 50 items (92.6%) reached consensus. Key statements that reached consensus within nomenclature included a clear definition for MLKI (LoA 97.4%) and the need for an updated MLKI classification system that classifies injury mechanism, extent of non-ligamentous structures injured and the presence or absence of dislocation. Within diagnosis, consensus was reached that there should be a low threshold for assessment with CT angiography for MLKI within a high-energy context and for certain injury patterns including bicruciate and PLC injuries (LoA 89.7%). The value of stress radiography or intraoperative fluoroscopy also reached consensus (LoA 89.7%). Within treatment, it was generally agreed that existing literature generally favours operative management of MLKI, particularly for young patients (LoA 100%), and that single-stage surgery should be performed whenever possible (LoA 92.3%). This consensus statement will facilitate clinical communication in MLKI, the care of these patients and future research within MLKI. Link to the article

Methods for recording and reporting of epidemiological data on injury and illness in tennis: ReFORM synthesis of the International Olympic Committee consensus statement
31/08/2024
Tooth C, Verhagen E, Pluim BM, et alMethods for recording and reporting of epidemiological data on injury and illness in tennis: ReFORM synthesis of the International Olympic Committee consensus statementBritish Journal of Sports Medicine Published Online First: 28 August 2024. doi: 10.1136/bjsports-2024-108830 Introduction Following the International Olympic Committee’s (IOC) consensus statement on the methods for collecting and reporting epidemiological data on injury and illness in sports,1 2 the International Tennis Federation’s Sports Science Committee, in collaboration with selected external experts, developed a tennis-specific extension.3 This initiative aimed to standardise health surveillance for non-disabled and wheelchair tennis players and provide discipline-specific recommendations regarding injury and illness classification, mechanisms, onset modes, athlete exposure, risk reporting and data collection methods. The tennis-specific extension and this summary aim to present the elements specific to tennis that differentiate or add to the original IOC consensus for recording and reporting epidemiological data on injury and illness in sports. Link to the article: https://bjsm.bmj.com/content/early/2024/08/28/bjsports-2024-108830

Development of a physical activity prescription in Luxembourg
16/08/2024
Delagardelle C., Lion A., Theisen D., Urhausen A., Worth M. https://doi.org/10.34045/SEMS/2024/34 Abstract Background: We aimed to develop a physical activity prescription (PAP) that would help efficiently promote PA by medical practitioners in Luxembourg. Methods: During a first phase, a PAP model and its user guide were created by 15 experts (medical doctors, sport and exercise scientists, physiotherapists). Second, this PAP and its user guide were evaluated by a panel of medical doctors (different from the 15 experts) who were asked to answer a questionnaire in 2 rounds using 41 questions and 2 questions, respectively. Results: The panel was composed of 66 medical practitioners. Of the 41 items of the PAP, six did not reach consensus and had to be re-evaluated during a 2nd round in which 50 medical practitioners participated. After this 2nd round, four items did not reach consensus and were subsequently presented as optional. A consensus was found concerning the PAP guide from the first round. Conclusion: Our study allowed the development of a consensual tool for the prescription of PA by physicians for physicians. The PAP and its guide may help practitioners to promote health-enhancing PA, in conjunction with a systematic policy-level PA promotion to address the public health issue of physical inactivity. Link to the article
Blood and urine biomarkers for the diagnosis of early stages of knee osteoarthritis: A systematic review
01/08/2024
Ostojic M, Oliveira JP, Kordic D, Mouton C, Prill R, Becker R. Blood and urine biomarkers for the diagnosis of early stages of knee osteoarthritis: A systematic review. J Exp Orthop. 2024 Jul 29;11(3):e12105. doi: 10.1002/jeo2.12105. PMID: 39076848; PMCID: PMC11284962. Purpose. To identify biomarkers in human blood or urine at an early stage of knee osteoarthritis (OA) and to elucidate if any can accurately differentiate between healthy controls and early knee OA patients and be considered as a candidate for widespread clinical use for early diagnosis of the disease. Methods. Medline, Embase and Web of Science were screened to identify comparative studies measuring differences in blood or urine biomarkers between healthy controls and knee OA patients at an early stage (grade 1 or 2 Kellgren–Laurence). Two independent reviewers screened the abstracts for eligibility, reviewed the full texts, assessed the methodological quality and extracted the data. The Joanna Briggs Institute critical appraisal tool for diagnostic test accuracy studies was used to assess the quality of the included studies. Due to relevant heterogeneity, meta‐analysis was not appropriate. Results. Five studies met the eligibility criteria. The examined biomarkers were adropin, collagen type II metabolite, C‐terminal cross‐linked telopeptide of type II collagen, C‐terminal cross‐linked telopeptide of type I collagen, cartilage oligomeric matrix protein, matrix metalloproteinase 3, N‐terminal propeptide of procollagen type IIA, type I procollagen N‐terminal propeptides, N‐terminal osteocalcin, angiopoietin‐2, follistatin, granulocyte colony‐stimulating factor, hepatocyte growth factor, interleukin‐8, leptin, platelet‐derived growth factor‐BB, platelet endothelial cell adhesion molecule‐1, vascular endothelial growth factor and calprotectin and totalling 19 biomarkers. All of the biomarkers were studied only once in the selected papers. Conclusions. There is no reliable biomarker available to differentiate between early knee OA in patients and healthy controls, but a potential role of a cluster of biomarkers to close this gap. There are several limitations, including inappropriate study designs, small sample sizes, nonconsecutive patient groups and inadequate statistical methods for evaluating biomarker performance in studies included. Link to the article: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11284962/

Best presentation award of the GOTS Science Awards 2024
10/07/2024
Liroms supported the “best presentation” award, which was presented at the GOTS Annual Congress 2024. Congratulations to the winners: 1st place: Becker, Josephine, Biomechanical characterization of the external meniscus suture with all-inside fixation on the popliteus tendon2nd place: Degenhardt, Hannes, Beach handball: frequent injuries, injury mechanisms, risk factors & return to sport - a cross-sectional survey on 651 athletes3rd place: Weishorn, Johannes, The role of autologous bone grafting treating of large osteochondral defects at the kneeresults from a matched pairs analysis of 430 individuals in the German cartilage registry (Knorpelregister DGOU) For more information: https://gots.org/preistraeger-gots-wissenschaftspreise-2024/

Injuries of the posteromedial bundle of the posterior cruciate ligament after knee hyperextension trauma: A new clinical entity based on an original case series
08/07/2024
Mouton C, Ibañez M, Hoffmann F, Monllau JC, Seil R. Injuries of the posteromedial bundle of the posterior cruciate ligament after knee hyperextension trauma: A new clinical entity based on an original case series. J Exp Orthop. 2024 Jul 5;11(3):e12052. doi: 10.1002/jeo2.12052. PMID: 38974050; PMCID: PMC11224766. Abstract Purpose: This original case series aims to describe an uncommon triad of clinical signs in patients presenting with persistent pain and inability to resume physical activities after knee hyperextension trauma. Methods: Patient history, clinical examination, arthroscopic findings and investigations of 12 patients who consulted with the senior author are presented. Results: Twelve patients (seven males/five females) presented with persistent pain after knee hyperextension trauma either in sport or a traffic accident. They had a median age of 18.5 and a median body mass index of 23 kg/m2. All had medical visits and at least one magnetic resonance imaging (MRI) before visiting the senior author's institution but the cause of their problems could not be explained. The clinical examination of the injured knee appeared normal except for an uncommon triad of clinical signs with the knee close to extension: (1) a grade 1+ anterior-posterior laxity around 10-20° of knee flexion with a firm end-point (pseudo-Lachman sign), (2) a grade 1+ tibiofemoral step-off sign with a posterior drawer at 10-20° of knee flexion and (3) an increased knee hyperextension compared to the contralateral side. Arthroscopy of eight patients confirmed the pseudo-Lachman sign with a grade I posterior drawer close to knee extension, normal posterior laxity at 90° of knee flexion and an intact anterior cruciate ligament. Conclusion: Patients displayed an increased hyperextension and posterior laxity close to knee extension which normalised at 90° of knee flexion. In patients with a history of knee hyperextension trauma associated with persistent pain, inability to resume physical activities, inconclusive MRIs and a standard clinical examination, clinicians should consider extending their investigations with the knee close to extension to identify this clinical triad consistent with a lesion to the posteromedial bundle of the posterior cruciate ligament. Link to the article: https://pubmed.ncbi.nlm.nih.gov/38974050/

Neuromuscular Adaptations in Endurance-Trained Male Adolescents Versus Untrained Peers: A 9-Month Longitudinal Study
22/06/2024
Birat A, Garnier YM, Dupuy A, Bontemps B, Dodu A, Grossoeuvre C, Dupont AC, Rance M, Morel C, Blazevich AJ, Nottin S, Ratel S. Neuromuscular Adaptations in Endurance-Trained Male Adolescents Versus Untrained Peers: A 9-Month Longitudinal Study. Scand J Med Sci Sports. 2024 Jun;34(6):e14681. doi: 10.1111/sms.14681. PMID: 38881390. Abstract Background: Neuromuscular function is considered as a determinant factor of endurance performance during adulthood. However, whether endurance training triggers further neuromuscular adaptations exceeding those of growth and maturation alone over the rapid adolescent growth period is yet to be determined. Objective: The present study investigated the concurrent role of growth, maturation, and endurance training on neuromuscular function through a 9-month training period in adolescent triathletes. Link to the article: https://pubmed.ncbi.nlm.nih.gov/38881390/

7. GOTS-Expertenmeeting, Deidesheim 7.-9.10.2022, Kindersportmedizin
21/06/2024
Liroms is very proud to announce the release of the GOTS expert meeting book on paediatric sports medicine.

Restoring the Preoperative Phenotype According to the Coronal Plane Alignment of the Knee Classification After Total Knee Arthroplasty Leads to Better Functional Results
14/06/2024
Pangaud C, Siboni R, Gonzalez J-F, Argenson J-N, Seil R, Froidefond P, Mouton C, Micicoi G, Restoring the Preoperative Phenotype According to the Coronal Plane Alignment of the Knee (CPAK) Classification After Total Knee Arthroplasty Leads to Better Functional Results, The Journal of Arthroplasty (2024), doi: https://doi.org/10.1016/j.arth.2024.06.012. Abstract Background. Mechanical alignment after total knee arthroplasty (TKA) is still widely used in the surgical community, but the alignment finally obtained by conventional techniques remains uncertain. The recent Coronal Plane Alignment of the Knee (CPAK) classification distinguishes 9 knee phenotypes according to constitutional alignment and joint line obliquity (JLO). The aim of this study was to assess the phenotypes of osteoarthritic patients before and after TKA using mechanical alignment and to analyze the influence of CPAK restoration on functional outcomes. Methods. This retrospective multicenter study included 178 TKAs with a minimum follow-up of 2 years. Patients were operated on using a conventional technique with the goal of neutral mechanical alignment. The CPAK grade (1 to 9), considering the arithmetic Hip-Knee-Ankle angle (aHKA) and the JLO, was determined before and after TKA. Functional results were assessed using the following patient-reported outcome measures: Knee Injury and Osteoarthritis Outcome Score, the Simple Knee Value, and the Forgotten Joint Score. Results. A true neutral mechanical alignment was obtained in only 37.1%. Isolated restoration of JLO was found in 31.4%, and isolated restoration of the aHKA in 44.9%. Exact restoration of the CPAK phenotype was found in 14.6%. Restoration of the CPAK grade was associated with an improvement in the “daily living”: 79.2 ± 5.3 versus 62.5 ± 2.3 (R2 = 0.05, P < .05) and “Quality of life” Knee Injury and Osteoarthritis Outcome Score subscales: 73.8 ± 5.0 versus 62.9 ± 2.2 (R2 = 0.02, P < .05). Conclusions. This study shows that few neutral mechanical alignments are finally obtained after TKA by conventional technique. A major number of patients present a postoperative modification of their constitutional phenotype. Functional results at 2 years of follow-up appear to be improved by the restoration of the CPAK phenotype, JLO, and aHKA. Link to the article: https://www.arthroplastyjournal.org/article/S0883-5403(24)00611-9/fulltext

Longitudinal study of changes in greenness exposure, physical activity and sedentary behavior in the ORISCAV-LUX cohort study
21/05/2024
van Beek, J.F.E., Malisoux, L, Klein, et al. Longitudinal study of changes in greenness exposure, physical activity and sedentary behavior in the ORISCAV-LUX cohort study. Int J Health Geogr 23, 14 (2024). https://doi.org/10.1186/s12942-024-00374-7 Abstract Background. Greenness exposure has been associated with many health benefits, for example through the pathway of providing opportunities for physical activity (PA). Beside the limited body of longitudinal research, most studies overlook to what extent different types of greenness exposures may be associated with varying levels of PA and sedentary behavior (SB). In this study, we investigated associations of greenness characterized by density, diversity and vegetation type with self-reported PA and SB over a 9-year period, using data from the ORISCAV-LUX study (2007–2017, n = 628). Link to the article: https://ij-healthgeographics.biomedcentral.com/articles/10.1186/s12942-024-00374-7

A practical guide to the implementation of artificial intelligence in orthopaedic research—Part 2: A technical introduction
07/05/2024
Zsidai B, Kaarre J, Narup E, Hamrin Senorski E, Pareek A, Grassi A, Ley C, Longo UG, Herbst E, Hirschmann MT, Kopf S, Seil R, Tischer T, Samuelsson K, Feldt R; ESSKA Artificial Intelligence Working Group. A practical guide to the implementation of artificial intelligence in orthopaedic research-Part 2: A technical introduction. J Exp Orthop. 2024 May 7;11(3):e12025. doi: 10.1002/jeo2.12025. PMID: 38715910; PMCID: PMC11076014. Abstract Recent advances in artificial intelligence (AI) present a broad range of possibilities in medical research. However, orthopaedic researchers aiming to participate in research projects implementing AI-based techniques require a sound understanding of the technical fundamentals of this rapidly developing field. Initial sections of this technical primer provide an overview of the general and the more detailed taxonomy of AI methods. Researchers are presented with the technical basics of the most frequently performed machine learning (ML) tasks, such as classification, regression, clustering and dimensionality reduction. Additionally, the spectrum of supervision in ML including the domains of supervised, unsupervised, semisupervised and self-supervised learning will be explored. Recent advances in neural networks (NNs) and deep learning (DL) architectures have rendered them essential tools for the analysis of complex medical data, which warrants a rudimentary technical introduction to orthopaedic researchers. Furthermore, the capability of natural language processing (NLP) to interpret patterns in human language is discussed and may offer several potential applications in medical text classification, patient sentiment analysis and clinical decision support. The technical discussion concludes with the transformative potential of generative AI and large language models (LLMs) on AI research. Consequently, this second article of the series aims to equip orthopaedic researchers with the fundamental technical knowledge required to engage in interdisciplinary collaboration in AI-driven orthopaedic research. Link to the article: https://pubmed.ncbi.nlm.nih.gov/38715910/

Joint line and knee osteotomy
01/05/2024
Pratobevera A, Seil R, Menetrey J. Joint line and knee osteotomy. EFORT Open Rev. 2024 May 10;9(5):375-386. doi: 10.1530/EOR-24-0037. PMID: 38726996; PMCID: PMC11099584. Abstract This review explores the intricate relationship between knee osteotomy and frontal plane joint line orientation, emphasizing the dynamic nature of the joint line’s influence on knee forces and kinematics.. Consideration of coronal alignments, knee phenotypes, and associated angles (medial proximal tibial angle (MTPA), lateral distal femoral angle (LDFA), joint line convergence angle (JLCA)) becomes crucial in surgical planning to avoid joint line deformities.. The double-level osteotomy is to be considered a valid option, especially for severe deformities; however, the target patient cannot be selected solely based on high predicted postoperative joint line obliquity (JLO) and MPTA.. Keywords: knee osteotomy, joint line orientation, knee phenotypes, frontal plane, double level osteotomy

Nonanatomic Posteromedial Bundle Augmentation of the Posterior Cruciate Ligament after Hyperextension Trauma
27/04/2024
Ibañez M, Valcarenghi J, Hoffmann F, Mouton C, Pioger C, Siboni R, Monllau JC, Seil R,Nonanatomic Posteromedial Bundle Augmentation of the Posterior Cruciate Ligament after Hyperextension Trauma,Arthroscopy Techniques, Volume 13, Issue 8, 2024, 103013, ISSN 2212-6287, https://doi.org/10.1016/j.eats.2024.103013.Abstract: The surgical management of posterior cruciate ligament (PCL) injuries can be challenging. As most PCL injuries occur in a flexed knee position, the anterolateral bundle is thought to be more commonly injured than the posteromedial bundle (PMB); however, in hyperextension, the PMB plays a more significant role. The smaller size of the PMB compared with the anterolateral bundle and its lower strength may explain why isolated hyperextension PMB injuries can be easily overlooked. In this Technical Note, a surgical technique to perform a nonanatomic PMB augmentation of the PCL using a gracilis tendon autograft or allograft is reported. These technical features aim to overcome current limitations in existing techniques to address the symptoms after partial PCL hyperextension injuries. Link to the article: https://www.sciencedirect.com/science/article/pii/S2212628724001191

Sport‐specific differences in ACL injury, treatment and return to sports—Ski jumping
21/04/2024
Jakub Oronowicz*, Gunter Frenzel, Hubert Hörterer, Håvard Moksnes, Guri Ranum Ekas, Jan Cabri, Thomas Tischer, Romain Seil *Corresponding author for this work INTRODUCTION Ski jumping is a very difficult sport discipline requiring extreme technical finesse at high velocity and thus has a specific injury profile. Fortunately, debilitating injuries resulting in permanent disability, such as blindness or lesions to the central nervous system, were eradicated long ago. Compared with other winter sports (i.e., alpine skiing), ski jumping has been reported to have a lower general injury risk. Absolute injury rates in female ski jumpers have been reported to be around 26 injuries/100 athletes/season. The knee is the most frequently affected body part, accounting for 33% of the injuries. Severe knee injuries and especially anterior crucial ligament (ACL) tears seem to be very common, although their exact incidence is still unknown. In countries such as Germany and Norway, ski jumping is popular, has a long tradition and the elite‐level athletes from these countries have been very successful. Recently, many ACL injuries have been observed by members of the medical staff (G. F., G. R. E. and H. M.) in elite male and female ski jumpers. Severe knee injuries, especially ACL injuries, can cause long‐term time losses, decreased perform- ance levels after return to competition and end a career prematurely. Therefore, it is crucial to better understand the sport‐specific ACL injury mechanisms to optimise the treatment and to develop prevention strategies. Link to the article

Sexual violence in sports: the essentials
21/03/2024
Sexual violence in sports: the essentials Original title: Les violences sexuelles et sport : l’essentiel pour agir LIROMS is honored to announce the forthcoming publication, on June 12th, of a book on sexual violence in sport, to which Dr. Katy Moreels, member of LIHPS and the COSL medical and scientific commission, has contributed with a chapter entitled: Bio-psycho-social conceptual model of violence in sport: to better understand, detect and act. The book is published in French by Elsevier Masson and it has been edited by Drs. Olivier Coste and Philippe Liotard from France. It is the fruit of their nearly 25 years' experience on this subject and brings together 35 contributors. It offers an original multidisciplinary approach to sexual violence in sport, integrating it with available data on other forms of violence and other fields. It is aimed at those involved in the world of sports (coaches, educators, healthcare professionals) as well as athletes and their parents. More than thirty authors from France and abroad provide food for thought in three sections: 1) definitions and mechanisms, 2) recognizing, listening and reporting, 3) action plan, prevention and training. The covered aspects will enable readers to increase the effectiveness of their actions through a better understanding of the issues and the logic behind this type of violence.

Information videos posted on Instagram by orthopaedics and sports traumatology surgeons mostly explain surgical technique, and the least mentioned topics are injury prevention and complications
24/02/2024
Şahbat Y, Kocaoğlu B, Ollivier M, Cerciello S, Akgün D, Alentorn-Geli E, Kayaalp ME, Akın HF, Knauer P, Hariri A, Mocini F, Bartroli AP, Seil R. Information videos posted on Instagram by orthopaedics and sports traumatology surgeons mostly explain surgical technique, and the least mentioned topics are injury prevention and complications. Knee Surg Sports Traumatol Arthrosc. 2024 May;32(5):1160-1167. doi: 10.1002/ksa.12140. Epub 2024 Mar 15. PMID: 38488237. Purpose: Social media has become the new information acquisition platform for all content producers. In the current literature, there are no studies examining the content quality and the strengths and weaknesses of videos on Instagram that explain anterior cruciate ligament (ACL) injuries, which is the most discussed topic of sports surgery. The aim of this study was to evaluate the quality, strengths and weaknesses of information pertaining to ACL surgery that is disseminated on Instagram. Link to the article : https://pubmed.ncbi.nlm.nih.gov/38488237/

Vacancy: clinical gait and movement specialist
19/02/2024
We are hiring a clinical gait and movement specialist.

Anterior cruciate ligament injuries in elite ski jumping reliably allow return to competition but severely affect future top performance
16/02/2024
Oronowicz J, Seil R, Hörterer H, Moksnes H, Ekas GR, Cabri J, Mouton C, Frenzel G, Tischer T. Anterior cruciate ligament injuries in elite ski jumping reliably allow return to competition but severely affect future top performance. Knee Surg Sports Traumatol Arthrosc. 2024 Feb 16. doi: 10.1002/ksa.12076. Epub ahead of print. PMID: 38363010. Link to the article Abstract Purpose: In recent years, anterior cruciate ligament (ACL) injuries have been frequently observed in ski jumping. However, available data in this discipline are very scarce. Therefore, the purpose of this study was to investigate whether an ACL injury in elite-level ski jumping limits the performance level after ACL reconstruction (ACLR). Methods: Both male and female elite-level ski jumpers from five national A-teams who suffered an ACL injury were identified retrospectively by searching available media reports and Fédération Internationale de Ski (FIS) database. World Cup (WC) results and time-out-of-competition before ACL injury and after ACLR were compared. Only athletes who suffered the injury during or after the 2009-2010 season and who participated in at least one WC competition before the injury were included in this study. The level of athletes' performance from two full seasons before until three seasons after the injury was compared. Results: Eighteen elite-level ski jumpers (11 males/seven females) were eligible for the study. All male and four female athletes returned to professional competition after ACLR. One female athlete ended her career due to prolonged recovery and two have not yet recovered due to a recent injury. The mean return-to-competition (RTC) time was 14.6 months in males and 13.5 months in females. The mean WC placement decreased after the ACL injury: two seasons before injury the mean position was 17.9 ± 11.0 (n = 12), one season before it was 22.4 ± 12.8 (n = 15). After recovery, the mean placement in seasons 1-3 was: 26.4 ± 8.9 (n = 7), 25.7 ± 10.3 (n = 13), 33.6 ± 12.2 (n = 10) (p = 0.008). Among the athletes returning to competition, only six males and three females reached their preinjury level and only one male and one female (compared to seven males and three females preinjury) reached an individual top-3 placement after ACLR, accounting for less than 10% of podiums compared to preinjury. Conclusion: Only 60% of the professional ski jumpers reached the preinjury level and less than 15% reached a top-3 placement after the ACL injury. These results support the fact that ACL tear during a ski jumping career may be a significant factor limiting high-level performance. In terms of clinical relevance, the findings implicate the need to analyse the reasons of these very low rates of return to elite-level performance, to analyse ACL injury and RTC rates at lower levels of performance and to develop specific prevention strategies in order to reduce the number of ACL injuries in this sport.

Using ultrasound shear wave elastography to characterize peripheral nerve mechanics: a systematic review on the normative reference values in healthy individuals
14/02/2024
Neto T, Johannsson J, Andrade RJ. Using ultrasound shear wave elastography to characterize peripheral nerve mechanics: a systematic review on the normative reference values in healthy individuals. Ultrasonography. 2024 May;43(3):169-178. doi: 10.14366/usg.23211. Epub 2024 Feb 14. PMID: 38544459; PMCID: PMC11079506. Abstract Ultrasound shear wave elastography (SWE) is an emerging non-invasive imaging technique for peripheral nerve evaluation. Shear wave velocity (SWV), a surrogate measure of stiffness, holds promise as a biomarker for various peripheral nerve disorders. However, to maximize its clinical and biomechanical value, it is important to fully understand the factors that influence nerve SWV measurements. This systematic review aimed to identify the normal range of SWV for healthy sciatic and tibial nerves and to reveal the factors potentially affecting nerve SWV. An electronic search yielded 17 studies eligible for inclusion, involving 548 healthy individuals (age range, 17 to 72 years). Despite very good reliability metrics, the reported SWV values differed considerably across studies for the sciatic (1.9-9.9 m/s) and tibial (2.3-9.1 m/s) nerves. Factors such as measurement proximity to joint regions, limb postures inducing nerve axial stretching, and transducer alignment with nerve fiber orientation were associated with increased SWV. These findings suggest regional-specific nerve mechanical properties, non-linear elastic behaviour, and marked mechanical anisotropy. The impact of age and sex remains unclear and warrants further investigation. These results emphasize the importance of considering these factors when assessing and interpreting nerve SWE. While increased SWV has been linked to pathological changes affecting nerve tissue mechanics, the significant variability observed in healthy nerves highlights the need for standardized SWE assessment protocols. Developing guidelines for enhanced clinical utility and achieving a comprehensive understanding of the factors that influence nerve SWE assessments are critical in advancing the field. Keywords: Ultrasound shear wave elastography, Ultrasonography, Sciatic neuropathy, Peripheral nervous system, Nerve biomechanics, Non-invasive mechanics, Diagnostic imaging Link to the article: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11079506/

Program 2024 Luxembourg Academy of sports medicine, physiotherapy & science
22/01/2024
The new program for 2024 is now available.

Actualités Team Lëtzebuerg
16/11/2023
LIROMS well represented on the Team Letzebuerg Evening. The evening was an opportunity to look back on the year's sporting events and celebrate successes of the competitions across Europe. The reception was an opportunity for the Head of State to appreciate the determination of the athletes who have made it to the top of the 10,500 qualifiers. https://teamletzebuerg.lu/actualites/

Visit of students of the GOTS Master course on topics concerning clinical biomechanics
16/11/2023
LIROMS – team involved in the Master Week of the Gesellschaft für Orthopädisch-Traumatologische Sportmedizin (GOTS), organized by Dr. Christian Nührenbörger. In the week of 13th November, we were hosting students of the GOTS Master Course on topics concerning clinical biomechanics. The program offered on the 16th December can be found below. The students represented different medical specializations: from sports medicine to anesthesiology. Dr. C. Mouton held a talk on the ACL clinical pathway as offered in the CHL and demonstrated the ACL laxity-tests in the afternoon. The practical sessions consisted also of demonstrations of some of the tests carried out by the physiotherapy team. The programme: Uhrzeit . Programm . Referent . . Science and Research in Sports Medicine . . 08:30 – 09:00 . ACL-Pathway . Mouton C. . 09:15 – 09:45 . Kinematics and kinetics of gait and running . Fayad J. . 10:00 – 10:30 . Assessment of strength and power . Neto T. . 10:45 – 11:15 . Kinesiologische Elektromyographie . Cabri J. . 11:30 – 12:00 . Biomechanische Basistests im Leistungssport . Cabri J. . 12:00 – 15:00 . Mittagspause mit gemeinsamem Essen und Stadtrundgang Luxemburg City . . 15:00 - 18:00 . Clinique d’Eich CHL Clinique du Sport & Human Motion Lab Praxis in 2 Gruppen ACL-Testung (Laxität, Isokinetik, Sprünge) Biomechanical analysis of gait and running, including EMG. . Cabri J. / Mouton C. / Wennig L. / Neto T. / Wojtylka C. / Fayad J. .

Mini-Invasive Harvesting of Quadriceps Tendon Graft With Patellar Bone Block for ACL Reconstruction Using a Dedicated Harvester
20/10/2023
Vittone G, Valcarenghi J, Mouton C, Seil R. Mini-Invasive Harvesting of Quadriceps Tendon Graft With Patellar Bone Block for ACL Reconstruction Using a Dedicated Harvester. Video Journal of Sports Medicine. 2023;3(5). doi:10.1177/26350254231207405 Background: The selection of the type of graft used to reconstruct the anterior cruciate ligament (ACL) remains a matter of debate. In the past, the quadriceps tendon (QT) was associated with considerable morbidity and less favorable outcomes than other grafts. Improvements in harvesting methods have decreased morbidity of the surgical procedure and led to an increase in the use of QT in recent years. Indications: The QT graft with patellar bone block is a viable option for all patients with closed physis undergoing ACL reconstruction. It is especially suitable for young and active patients who practice activities that require kneeling or athletes in which hamstrings preservation is advisable. Technique Description: A vertical mini-invasive longitudinal incision starts 1 cm proximal to the middle of the patellar pole. After dissection, the bone block is marked and detached with an oscillating saw. A drill hole is performed in the bone block to serve for the passage of a traction suture. The bone block is lifted with the help of the traction suture, and the graft is trimmed to the desired diameter. The layer between tendon and capsule is separated by blunt dissection to spare the capsule of the suprapatellar pouch. Harvesting is achieved using a dedicated QT harvester. Usually, a graft length of 8 cm is harvested. The defect in the QT is closed using a suture passer at the proximal end. Finally, the graft is prepared and calibrated according to the planned technique for ACL reconstruction. Results: There was no major intraoperative complication in the senior author's series (more than 50 patients) using the dedicated QT harvester. On rare occasions (<10% of the cases), the device opened the suprapatellar joint capsule, creating the additional need for capsular repair during defect closure. On two occasions, the graft was shorter than expected, which may have been caused by insufficient dissection or improper use of the harvester. Link to the article

Professor Jan Cabri honored by Portuguese Order of Physiotherapists
30/09/2023
Saturday 30 September 2023, Prof. Jan Cabri was one of the central guests during the honoring ceremony of the Portuguese Order of Physiotherapists. He was rewarded for his work which resulted in the academization of physiotherapy education in Portugal. Through his endeavors, he was the first to offer physiotherapists the possibility to get a university education, leading to a doctorate (PhD) and research lines in this field of work. The document received states: “On the occasion of the 4th anniversary of the Order of Physiotherapists, the board of directors decided to recognize the merit of Jan Cabri in the development and affirmation of Physiotherapy as an autonomous scientific discipline in Portugal, namely for having released the creation of the first doctoral line with the mention of Physiotherapy at the Faculty of Human Kinetics of the Technical University of Lisbon.”
10th anniversary congress of the Cartilage Net of the Greater Region
28/09/2023
On September 28th and 29th 2023, 3 LIROMS and CHL collaborators, Prof Dr med Romain Seil, Dr med Christian Nührenbörger and Dr Caroline Mouton and a resident from the Department of Orthopaedic Surgery of the CHL, Dr med Yorick Fonteyn, attended the 10th anniversary congress of the Cartilage Net of the Greater Region in Saarbrücken, Germany. The congress was perfectly organized and chaired by Prof. Magali Cucchiarini and Prof. Henning Madry from the Department of Experimental Orthopaedics of the University of Saarland and co-chaired by Prof. Seil. The network brings together the different basic, scientific, clinical and engineering groups of the greater region since 2011. This year's congress edition was placed under the European spirit with a special emphasis on the 60th anniversary of the Elysée Treaty and was an ideal platform to honor the friendship between France, Germany, Luxembourg and Belgium. It was an opportunity to exchange on academic cooperation in the Greater Region and the challenges and future of academic research in the field of cartilage diseases with many special guests including Jakob von Weizsäcker, Minister of Finance and Science of Saarland; Profs. Manfred Schmitt and Patricia Oster-Stierle, President and former Vice President of Saarland University; M Georges Santer, Luxembourg's former ambassador in Paris and Berlin as well as M Sébastien Girard, Consul of France in Saarbrücken. Participants from Saarbrücken, Liège, Nancy and Luxembourg focused on recent evolutions in basic science and clinical research in cartilage and related diseases. The Luxembourgish participants reported on their research line on anterior cruciate ligament injuries. These severe knee injuries have a significant public health burden and bear a high risk of meniscus and cartilage lesions as well as later osteoarthritis. Special emphasis was made on the need for injury prevention by Dr Nuhrenbörger, on the importance of documenting the associated tissue damage by Dr Yorick Fonteyn, on joint preservation surgeries by Prof Dr Seil and on the importance of patient follow up by Dr Caroline Mouton.

APPOINTMENT OF PROF. DR. ROMAIN SEIL AS A MEMBER OF THE IOC'S MEDICAL AND SCIENTIFIC COMMISSION
04/09/2023
The Luxembourg Olympic and Sports Committee (COSL) announced the appointment of Prof Dr Romain Seil, member of the Board of Directors and Chairman of the COSL Medical and Scientific Commission, as a member of the Medical and Scientific Commission of the International Olympic Committee (IOC). Link to the article

ECSS - Paris 2023
07/07/2023
Alexandre Maricot – PhD student at the Vrije Universiteit Brussel presented his work on chronic ankle instability at the 28th Annual Congress of the European College of Sport Science in Paris. The project is sponsored by LIROMS and LIH under the supervision of Prof. Romain Meeusen and the academic coordination of Prof. Jan Cabri and Dr. Bernd Grimm.

Global Alliance for the Promotion of Physical Activity: the Hamburg Declaration
29/06/2023
Steinacker JM, Mechelen WV, Bloch W, et alGlobal Alliance for the Promotion of Physical Activity: the Hamburg DeclarationBMJ Open Sport & Exercise Medicine 2023;9:e001626. doi: 10.1136/bmjsem-2023-001626 ABSTRACT Non-communicable diseases (NCDs), including coronary heart disease, stroke, hypertension, type 2 diabetes, dementia, depression and cancers, are on the rise worldwide and are often associated with a lack of physical activity (PA). Globally, the levels of PA among individuals are below WHO recommendations. A lack of PA can increase morbidity and mortality, worsen the quality of life and increase the economic burden on individuals and society. In response to this trend, numerous organisations came together under one umbrella in Hamburg, Germany, in April 2021 and signed the ‘Hamburg Declaration’. This represented an international commitment to take all necessary actions to increase PA and improve the health of individuals to entire communities. Individuals and organisations are working together as the ‘Global Alliance for the Promotion of Physical Activity’ to drive long-term individual and population-wide behaviour change by collaborating with all stakeholders in the community: active hospitals, physical activity specialists, community services and healthcare providers, all achieving sustainable health goals for their patients/clients. The ‘Hamburg Declaration’ calls on national and international policymakers to take concrete action to promote daily PA and exercise at a population level and in healthcare settings. Link to the article

IOC reiterates its support for the Hamburg Declaration to tackle physical inactivity
26/06/2023
The International Olympic Committee (IOC) has further underscored its commitment to encouraging healthy and active lifestyles through its support for the Global Alliance for the Promotion of Physical Activity, enshrined in the Hamburg Declaration, of which the IOC is one of over 100 signatories. Link to the article

Dr Christian Nührenbörger of the CHL Luxembourg is "Sports Doctor of the Year 2023"
16/06/2023
Dr Christian Nührenbörger, Head of the Sports Orthopaedics Department and Consultant Head of Sports Medicine and Prevention at the Centre Hospitalier de Luxembourg (CHL), has been named "Sports Doctor of the Year 2023" by the GOTS.Dr Nührenbörger, who is also President of the Congress of the Society of Orthopaedic-Traumatological Sports Medicine and a presenter in Luxembourg this year, has been honoured for his national achievements in sports medicine. The prize is already be the 2nd. Sharing for someone from Luxembourg - in 2016, Dr Axel Urhausen was already named Sports Doctor of the Year by the CHL."I have no words, it was quite a surprise. You're crazy," said Dr Nührenbörger, who was completely "surprised" by the award. "I'd like to thank GOTS, the medical doctors, my colleagues Romain Seil and Axel Urhausen and of course my family for the support. It's a great pleasure to accept the title. "With Dr Christian Nührenbörger, non-surgical sports orthopaedics as a mainstay of sports medical care can no longer be imagined in Luxembourg. In the meantime, even a number drawing device had to be installed in the CHL waiting room for his emergency consultation. Dr Nührenbörger studied human medicine at the Wilhelms Westphalian University in Münster (D), with periods abroad in Lille and in the USA. He completed his training as a specialist in orthopaedics at the University of Magdeburg, the Hellersen Hospital for Sports Injuries and the Orthopaedic Clinic at Saarland University in Hombourg/Saar. In 1997, he graduated with a thesis on "fractures and dislocations of the root bones of the foot".He obtained additional designations in sports medicine and chiropractic, as well as training in osteopathic medicine, atmospheric therapy, manual medical diagnosis and therapy for infants and disabled children.He has been working at the Centre Hospitalier de Luxembourg since 2004. Starting out in containers in the clinic car park, with his tenacity he has succeeded in establishing his leading field of sports orthopaedics in sports medicine, through teamwork with Prof. Dr. Romain Seil. Dr Nührenbörger has many years' experience in providing sports medical support to clubs, associations and national teams in Germany and Luxembourg in a variety of sports - including rowing, football and triathlon - at events such as the last 3 Olympic Games for Luxembourg, as well as the European Games and the European Youth Games.But the doctor has proved his commitment and expertise not only in caring for athletes at the highest level - his dedication also applies to leisure and health sportspeople, right down to the patient who "moves or can be moved".He pays great attention to the fundamental ethics of the medical profession. He therefore applauds his athletic patients and welcomes good achievements, but rejects achievements at any cost. His stance in the fight against doping and the abuse of power in sport has been, and still is, clear and exemplary.Christian Nührenbörger has been a member of the GOTS since 2003, and since 2022 he has been a member of the Board of Directors, working with the Children's Sports Orthopaedics Committee and the Education Commission. In Luxembourg, he is a member of the National Olympic Committee's medical commission and the board of directors of the LIHPS Olympic Support Centre.From October, he will head up the CHL's sports medical department.

Safeguarding the young athlete in sport
01/06/2023
Lisa Bode, Tine Vertommen, Christian Nührenbörger,Safeguarding the young athlete in sport,Sports Orthopaedics and Traumatology,Volume 39, Issue 2, 2023, Pages 145-154, ISSN 0949-328X,https://doi.org/10.1016/j.orthtr.2023.04.004.(https://www.sciencedirect.com/science/article/pii/S0949328X23001242) Link to the article Summary Recent cases and studies have proven the need for measures of prevention of interpersonal violence against children and adolescents in sports. Dimensions of violence are multi-faceted and e.g. range from psychological degradation or humiliation based on gender, body shape or performance, undue pressure on young athletes to achieve high performance, sex required as a prerequisite for team selection or privileges, physically injurious or sexually degrading initiation (hazing) rituals, to nutrition and weight loss regimes leading to eating disorders such as anorexia or other health problems, beatings and other forms of physical punishment as a spur to improved performance, injury through forced risk-taking in extreme environments and many other possible forms of violence. Perpetrators can most often be found in the direct environment of the athletes. As the child’s right to play is anchored in the United Nations’ Convention on the Rights of the Child any organization providing sports activities for children and young athletes should establish safeguarding measures to help prevent interpersonal violence. The aim to support all positive effects of sports on the well-being of an athlete, governments, national sport governing bodies, organizations, international and national associations, sport managers, officials, parents and caregivers, coaches, support staff, physical education teachers, peers, medical, psychological and scientific staff, fans and educators need to be involved. Athletes should be encouraged to speak up for changes, and survivors should be given a safe space to speak their mind – but the responsibility to speak up and stop the abuse is never the athlete‘s, but rather the perpetrator‘s, and that of bystanders and those responsible for organizing sport.

Students' visit from the High Performance Master of the University of Saarbrücken
31/05/2023
Today we received the visit of students from the High Performance Master of the University of Saarbrücken. This visit illustrates the constructive collaboration with Prof. Dr. Tim Meyer and Dr. Karen aus der Fünten, Institute of Sports and Preventive Medicine Saarland University through our new Memorandum of Understanding. LIROMS & LIHPS teams worked together to provide hands-on workshops on biomechanics, using some of the Sportfabrik equipment. We spent the full day with the students experimenting the different methods available: 3D kinematics and kinetics of jumping, strength and power analysis (1080 Synchro), running technique analysis, hamstrings eccentric strength (Nordbord & Forceframe).

Opening of the new Human Motion Lab (HML)
28/04/2023
On April 28, 2023, at 3 p.m., the Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science (LIROMS) inaugurated the new Human Motion Lab (HML), in the presence of the Minister of Health, Mrs. Paulette Lenert. This event was the occasion to present the "Healthy moves" project which was created thanks to the "André Losch Foundation", with the support of the "Luxembourg Institute of Health" (LIH) and the "Centre Hospitalier de Luxembourg" (CHL). It will be useful to practitioners and researchers of the associated institutions who are regularly confronted with a large number of diseases or injuries of the lower limbs in children, adolescents and young adults that can lead to functional (pain, joint instability, arthrosis) and social (reduced physical activity, difficulties in moving around or in accessing certain jobs) sequelae. The laboratory's objective will be to propose an innovative diagnostic offer accessible to all to cover medical needs that straddle the line between research and innovation on the one hand and daily clinical practice on the other. Equipped with highly sophisticated and innovative equipment including multiple cameras and force platforms, the new laboratory will allow dynamic analysis of patient movement with a very high degree of precision. It will thus extend the usual diagnostic range such as X-rays, scans or MRI, and objectify the results obtained after a treatment. The laboratory staff has specific know-how and works closely with the doctors of the above-mentioned institutions to find personalized therapeutic solutions, whether surgical or non-surgical. In addition to the refined diagnostic capabilities, they will allow the establishment of strategies for the prevention of secondary post-injury injuries such as severe knee sprains in children, for which the 1st European registry is based in Eich, in collaboration with the European Society of Sports Traumatology and Knee Surgery (ESSKA). Finally, the laboratory will be used for research purposes by two LIH teams, the "Physical Activity, Sports and Health" (PASH) group and the "Human Motion, Orthopaedics, Sports Medicine and Physical Methods" (HOSD) group.
Article RTL : Human Motion Lab -Nei Raimlechkeeten a modernst Technologie
28/04/2023
https://www.rtl.lu/news/national/a/2057336.html

MARKERLESS MOTION CAPTURE FOR CLINICAL MOVEMENT ANALYSIS AND THE INFLUENCE OF CLOTHING ON GAIT METRICS
01/04/2023
Flood, M. & Gette, Paul & Cabri, Jan & Grimm, Bernd. (2023). MARKERLESS MOTION CAPTURE FOR CLINICAL MOVEMENT ANALYSIS AND THE INFLUENCE OF CLOTHING ON GAIT METRICS. Orthopaedic Proceedings. 105-B. 70-70. 10.1302/1358-992X.2023.9.070. Abstract: For clinical movement analysis, optical marker-based motion capture is the gold standard. With the advancement of AI-driven computer vision, markerless motion capture (MMC) has emerged. Validity against the marker-based standard has only been examined for lightly-dressed subjects as required for marker placement. This pilot study investigates how different clothing affects the measurement of typical gait metrics. Gait tests at self-selected speed (4 km/h) were performed on a treadmill (Motek Grail), captured by 9 cameras (Qualisys Miqus, 720p, f=100Hz) and analyzed by a leading MMC application (Theia, Canada). A healthy subject (female, h=164cm, m=54kg) donned clothes between trials starting from lightly dressed (LD: bicycle tight, short-sleeved shirt), adding a short skirt (SS: hip occlusion) or a midi-skirt (MS: partial knee occlusion) or street wear (SW: jeans covering ankle, long-sleeved blouse), the lattern combined with a short jacket (SWJ) or a long coat (SWC). Gait parameters (mean±SD, t=10s) calculated (left leg, mid-stance) were ankle pronation (AP-M), knee flexion (KF-M), pelvic obliquity (PO-M) and trunk lateral lean (TL-M) representing clinically common metrics, different joints and anatomic planes. Four repetitions of the base style (LD) were compared to states of increased garment coverage using the t-test (Bonferroni correction). For most gait metrics, differences between the light dress (LD) and various clothing styles were absent (p>0.0175), small (< 2SD) or below the minimal clinically important differences (MCID). For instance, KF-M was for LD=10.5°±1.7 versus MD=12.0°±0.5 (p=0.07) despite partial knee cover. AP-M measured for LD=5.2°±0.6 versus SW=4.1°±0.7 (p<0.01) despite ankle cover-up. The difference for KF-M between LD=10.5°±1.7 versus SWL=6.0°±0.9, SW and SWJ (7.6°±1.5, p<0.01) indicates more intra-subject gait variability than clothing effect. This study suggests that typical clothings styles only have a small clinically possibly negligible effect on common gait parameters measured with MMC. Thus, patients may not need to change clothes or be instructed to wear specific garments. In addition to avoiding marker placement, this further increases speed, ease and economy of clinical gait analysis with MMC facilitating high volume or routine application. Link to the article: https://www.researchgate.net/publication/372662298_MARKERLESS_MOTION_CAPTURE_FOR_CLINICAL_MOVEMENT_ANALYSIS_AND_THE_INFLUENCE_OF_CLOTHING_ON_GAIT_METRICS
Traumatic meniscus tears
09/01/2023
Sebastian Kopf, Roland Becker, Romain Seil, Christian Staerke Link to the article Summary Traumatic meniscus tears exist isolated (in stable knees) or in conjunction with ligament tears of the knee. Classical traumatic meniscus tears such as longitudinal and radial tears should be repaired regardless of patient’s age, body mass index, tear length, etc., if tissue quality allows it and tear can be reduced. In recent years, new types of meniscus pathologies have been described. This includes mainly meniscus instability, tears of the posterolateral meniscus roots, and so-called ramp lesions of the medial meniscus. Especially the two later ones occur mainly combined with tears of the cruciate ligaments. Tears of the posterolateral meniscus root should be repaired. If a lesion of a meniscus ramp should be repaired is still a matter of debate.

Posterior Lateral Meniscal Root and Oblique Radial Tears: The Biomechanical Evidence Supports Repair of These Tears, Although Long-Term Clinical Studies Are Necessary
21/12/2022
Robert F. LaPrade, M.D., Ph.D. , Andrew G. Geeslin, M.D. , Jorge Chahla, M.D., Ph.D., Moises Cohen, M.D., Ph.D. , Lars Engebretsen, M.D., PhD. , Scott C. Faucett, M.D., M.S., Alan M. Getgood, M.D., F.R.C.S. , Eivind Inderhaug, M.D., Ph.D., Darren L. Johnson, M.D., Sebastian Kopf, Dr. med , Aaron J. Krych, M.D. , Christopher M. Larson, M.D. , Martin Lind, M.D., Ph.D., Gilbert Moatshe, M.D., Ph.D. , Iain R. Murray, F.R.C.S., Ph.D. , Volker Musahl, M.D., Roberto Negrin, M.D. , Jonathan C. Riboh, M.D., Romain Seil, M.D., Ph.D. , Tim Spalding, F.R.C.S. Orth Link to the article We read with interest the recent study titled “Stable Lateral Meniscus Posterior Root Tears Left in situ at Time of Anterior Cruciate Ligament Reconstruction are of Minimal Long-Term Clinical Detriment” by Shumborski, Salmon, Monk, and Pinczewski.1 Long-term patient-reported outcomes (PROs) in subjects undergoing anterior cruciate ligament (ACL) reconstruction with an intact lateral meniscus were compared with those with untreated “stable” lateral meniscal posterior root (LMPR) tears. The authors concluded that “there was no adverse clinical outcome to leaving a stable LMPR tear in situ at the time of ACL reconstruction” and that outcomes are similar in patients with these tears to those that had an intact meniscus. In response to the article by Shumborski et al., Dr. Shelbourne wrote an editorial commentary titled “Meniscus Tears Seen at the Time of Anterior Cruciate Ligament Reconstruction Are Overtreated.”2 We have concerns about the clinical implications of accepting the conclusions of these articles without appropriate contextualization.To provide a framework for discussion of our concerns, the posterior lateral meniscal anatomy and tear classification systems are reviewed. We then discuss the biomechanical influence of these tears in the context of knee laxity and contact mechanics. Next, the epidemiology of this tear type and the clinical importance of meniscal preservation in the setting of concomitant ACL reconstruction is discussed. The conclusions by Shumborski et al.1 are discussed in this context along with the recommendations from Shelbourne.2 Lastly, we share our rationale for treatment of these tears as well as recommendations for future communication and research on this important tear pattern.

The Female Athelete's Knee - Prof Dr Romain Seil
19/12/2022
Prof. Romain Seil - Swiss Sports Medicine Society Congress, Interlaken Switzerland - October 2022
Sport - Orthopaedie – Sport - Traumatologie Volume 38 - 2022
14/12/2022
Sports Orthopaedics and Traumatology Sport - Orthopaedie - Sport - Traumatologie Charakteristik Die Zeitschrift setzt einen wissenschaftlichen und praktischen sportorthopaedischen und sporttraumatologischen Schwerpunkt. Sie veroeffentlicht Originalarbeiten zu den Themengebieten Arthroskopie, Biomechanik, internistische Sportmedizin, Bewegungs- und Trainingslehre, Bildgebende Verfahren, Sportpsychologie und Sportrehabilitation sowie Diskussionen ueber Risiko bzw. Gesundheitswert verschiedener Sportarten, Kongressberichte, Erkenntnisse aus der Arzneimittelforschung sowie traumatologische Rahmenthemen. Interdisziplinaeren Themen wird in gebotenem Maße Platz eingeraeumt. Interessenten In Praxis und Klinik sportmedizinisch taetige Aerzte, Internisten, Chirurgen und Orthopaeden. Editorial. In vielen Sportarten ist das Kniegelenk eine der am haeufigsten verletzten Koerperregionen. Sowohl im Freizeit-als auch im Leistungssport generieren Knieverletzungen haeufig Ausfallzeiten von mehreren Wochen oder Monaten. Sie fuehren nicht selten zu Rezidivverletzungen und Folgeschaeden und koennen die Karriere der Athlet*innen maßgeblich negativ beeinflussen. Dies fuehrt haeufig dazu, dass es zu vorgealterten Gelenken kommt, die bereits in jungen Jahren erhebliche Verschleißraten und Arthrosezeichen aufweisen. Gleichzeitig ist der Wunsch zur koerperlichen und sportlichen Betaetigung auch bei zuvor unverletzten, aelteren Patient*innen ab der 5. oder 6. Lebensdekade mit altersgerechten Verschleiß- und Arthrosezeichen noch stark vorhanden, was die behandelnden A ̈rzte und Therapeuten haeufig vor schwierige therapeutische Herausforderungen stellt. In den vergangenen Jahren hat die rasante technologische und wissenschaftliche Entwicklung betraechtlich dazu beigetragen, die Gesamtzahl der Knieverletzungen vollstaendiger zu erfassen und ihr Entstehen besser zu verstehen. Durch die schnelle Verbesserung neuerer therapeutischer Verfahren gelingt es der Medizin zunehmend, viele Athlet*innen besser zu versorgen und es ihnen zu ermoeglichen, auch bei komplexen Verletzungen und Schaeden ihre vor- angegangene Leistungsfaehigkeit wieder zu erlangen. Dank der zur Verfuegung stehenden Hochleistungsmedizin bedeuten schwere Knieverletzungen, die Sportler frueher fast systematisch zur Aufgabe der leistungssportlichen Aktivitaeten gezwungen haben, heute in vielen Faellen nicht mehr das Karriereende. Nicht selten zieht dies aber auch eine Banalisierung der Sportverletzungen im Allgemeinen und der Knieverletzungen im Besonderen nach sich, insbesondere in weniger leistungsstarken Kategorien und im Jugendsport. Auch fu ̈hrt es dazu, dass a ̈ltere Patient*innen trotz bestehender Verschleißphaenomene noch hohe, manchmal unrealistische sportliche Ansprueche an ihr Kniegelenk stellen. Dieses Heft stellt einen aktuellen Ueberblick ueber neueste Erkenntnisse verschiedener Aspekte des breiten Versorgungsspektrums von Kniegelenkverletzungen dar. Neben einem Ueberblick zu den neuesten gelenkerhaltenden Verfahren bei monokompartimentaler Arthrose sowie einem Artikel zur Anwendung von natuerlichen, autologen oder allogenen Substanzen (Stichwort "orthobiologics") stellen die vier weiteren Beitraege zum Hauptthema verschiedene europaeische Kooperationsprojekte der „European Society of Sports Traumatology, Knee Surgery and Arthroscopy‘‘ (ESSKA) dar, in denen auch die GOTS zum Teil stark beteiligt war. Es handelt sich hierbei um drei europaeische Konsensusarbeiten, welche die ESSKA in den vergangenen Jahren unternommen hat. Sie handeln von neuen therapeutischen Ansaetzen zur Behandlung von degenerativen und traumatischen Meniskuslaesionen und vom schwierigen Thema der Revisionsoperationen des vorderen Kreuzbandes (VKB). Ein letzter Artikel beschreibt den aktuellen Stand des kindlichen Kreuzbandregisters der ESSKA, welches eines der wenigen internationalen Register in der Orthopaedie ist. Wir hoffen, dass diese Beitraege vielen GOTS-Mitgliedern nuetzlich sind, um ihr Wissen auf den aktuellen Stand zu bringen, die erwaehnten Erkrankungen oder Verfahren besser einschaetzen zu koennen und ihre sportlichen Patienten entsprechend realistisch zu beraten und zu behandeln. Luxemburg und Erlangen, den 10.11.2022 Prof. Dr. Romain Seil, Dr. Christian Nuehrenboerger, Prof. Thomas Tischer
Update in knee surgery – ACL revision
05/12/2022
Thomas Tischer, Roland Becker, Wolf Petersen, Chris Lutter, Romain Seil, Matthias J. Feucht Link to the article Summary Clinical outcome after revision reconstruction of the anterior cruciate ligament (ACL) is influenced by many factors such as cartilage and meniscal status, coronary and sagittal axis deformities, concomitant ligamentous instabilities, patient activity and aspiration. Revision surgery often results in a worse clinical outcome compared to primary reconstruction. Detailed preoperative diagnosis with careful stability testing in the coronal, sagittal, and axial planes, as well as comprehensive imaging, is a prerequisite for comprehensive preoperative planning. The indication for revision surgery should be individualized. Concomitant pathologies must be considered in this planning and often require additional surgical care (e.g., correction of dorsal tilt of the tibial plateau, refixation of ramp and root lesions, additive extraarticular anterolateral stabilization, cartilage therapy). Essential treatment strategies are outlined.

Enlarging the evidence base for optimal treatment of paediatric ACL injuries the Paediatric Anterior Cruciate Ligament Initiative (PAMI)
01/12/2022
Caroline Mouton, Amanda Magosch, Håvard Moksnes, Rob Janssen, Christian Fink, Stefano Zaffagnini, Juan Carlos Monllau, Guri Ekås, Lars Engebretsen, Christian Nührenbörger, Romain Seil Link to the article Summary. Anterior cruciate ligament (ACL) injuries in children and adolescents are a relevant health and economic burden and their incidence increases at a higher rate than in adults. These injuries compromise the quality of life, affect the development of the knee joint as well as its future functionality, and may lead to early onset of osteoarthritis. Because of their young age, these patients are furthermore at high risk for secondary intraarticular soft tissue damage and re-injury of the ACL. The relatively small number of pediatric ACL injuries in single hospitals, necessitates international multicenter studies to collect meaningful prospective data and long-term outcomes in a young patient population. As a result, there are few high-quality studies on the treatment of pediatric ACL rupture, and the evidence base of current treatment recommendations is insufficient. Thus, the Paediatric Anterior Cruciate Ligament Monitoring Initiative (PAMI) was created in 2013. The registry is designed to collect and analyze data on the diagnosis and treatment of ACL injuries in children and adolescents and to provide a basis for the development of international evidence-based guidelines. Since 2018, patients with a skeletal age of 8-14 years in girls and 8-16 years in boys, respectively, have been recruited for the PAMI registry in various international centers, and the number of recruiting centers as well as the number of patients is increasing constantly. Analysis of the data from the first three years of the project provides epidemiological data and suggests initial trends. It is evident that the project is well established and in international demand. A future challenge is to ensure the long-term durability of PAMI and the dissemination of scientific findings.

Inauguration de la « SportFabrik » à Oberkorn
28/11/2022
Communiqué par : ministère des Sports / Luxembourg Institute for High Performance in Sports (LIHPS) Le vendredi 25 novembre 2022, le ministre des Sports, Georges Engel, et le président du conseil d'administration du LIHPS, André Hoffmann, ont inauguré officiellement la « SportFabrik », située à Oberkorn. Cette infrastructure de pointe, née d'une idée commune du ministère des Sports, de la Ville de Differdange, du Comité olympique et sportif luxembourgeois (COSL) et du Centre médical olympique luxembourgeois (CMOL), place le Luxembourg en première ligne en matière de mesure d'analyse du mouvement, de prévention des blessures et de retour au sport chez le sportif de haut niveau en Europe. Géré par le Luxembourg Institute for High Performance in Sports (LIHPS), en collaboration avec son partenaire scientifique, le Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science (LIROMS), le laboratoire biomécanique de mouvement au sein de la SportFabrik a pour but de promouvoir le sport de haut niveau, la médecine et les sciences du sport.

Réunion internationale des centres de recherche olympiques : Rencontre d’experts au Luxembourg
23/11/2022
Le Luxembourg a eu l’honneur d’accueillir la réunion annuelle des 11 centres internationaux de recherche de la Commission médicale et scientifique du Comité International Olympique. Le Luxembourg est représenté dans cet illustre groupe d’experts du « IOC Research Center for the protection of the Athletes’ Health » par le « Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science » (LIROMS), qui représente la communauté francophone dans le consortium dit ReFORM (« Réseau Francophone Olympique de Recherche en Médecine du Sport ») avec 4 autres centres de recherche de Paris, Montréal, Genève et Liège. Pendant 3 jours, cette rencontre à huis clos a permis de discuter des dernières découvertes dans les domaines de l’épidémiologie, de la biomécanique, de la prévention, du diagnostic et du traitement des blessures sportives, dans le cadre d’échanges animés au plus haut niveau scientifique, et de les aborder sous de nombreux angles géographiques et culturels différents. En tant que membre du Comité International Olympique (CIO), S.A.R. le Grand-Duc a reçu le président du « Comité Olympique et Sportif Luxembourgeois », Monsieur André Hoffmann, le président du LIROMS, Prof. Dr Romain Seil, le président de la commission médicale et ancien vice-président du CIO, Prof. Uğur Erdener, le directeur médical du CIO, Dr Richard Budgett, ainsi que des représentants de tous les centres de recherche. En collaboration avec la « Amsterdam Collaboration on Health and Safety in Sports » (ACHSS), ReFORM a organisé les deux jours suivants un symposium ouvert à tous et réunissant plus de 150 participants. Il était consacré aux thèmes principaux de la sécurité, de la santé mentale et de la prévention des blessures dans le sport. L’objectif du symposium était d’améliorer la coopération interdisciplinaire entre tous les participants, d’élargir leur base de connaissances et de garantir le transfert de connaissances entre la recherche et la pratique dans le but ultime d’améliorer la santé des athlètes de tous les niveaux sportifs. Source: http://teamletzebuerg.lu/2022/10/reunion-internationale-des-centres-de-recherche-olympiques-rencontre-dexperts-au-luxembourg/

Les compléments alimentaires et l’athlète de haut niveau: synthèse ReFORM de la position de consensus du Comité International Olympique
21/11/2022
Erik Sesbreno, Steve Hein, Eve Tiollier, Valentin Lacroix, Gabrielle Ostiguy, Carole Maître, Anne-Charlotte Dupont, Renaud Siboni, Romain Seil, Géraldine Martens From : Maughan, R.J., Burke, L.M., Dvorak, J., Larson-Meyer, D.E., Peeling, P., Phillips, S.M. et al. (2018). IOC consensus statement: dietary supplements and the high-performance athlete. British Journal of Sports Medicine, 52(7): 439-455. Lien vers l’article complet Lien vers la traduction complète Résumé La nutrition contribue généralement de manière modeste mais précieuse à de bonnes performances chez les athlètes de haut niveau, et les complémentsalimentaires peuvent apporter une contribution mineure à ce programme nutritionnel. Néanmoins, l’utilisation de compléments est largement répandue à tous les niveaux du sport. Les produits décrits comme des compléments ont différents objectifs, notamment (1) prévenir et corriger les carences en micronutriments, (2) fournir des formes pratiques d’énergie et de macronutriments, et (3) apporter des avantages directs en termes de performance ou (4) des avantages indirects comme soutenir l’entraînement intense. L’utilisation appropriée de certains compléments peut être bénéfique à l’athlète, mais d’autres peuvent nuire à sa santé, à ses performances et/ou à sa à sa réputation (s’il en résulte une violation des règles antidopage). Une évaluation nutritionnelle complète doit être effectuée avant de prendre toute décision concernant des compléments. Les compléments supposés améliorer directement ou indirectement les performances représentent la majorité des produits proposés aux athlètes, mais seuls quelques-uns (parmi lesquels la caféine, la créatine, des substances tampons spécifiques et le nitrate) ont des avantages avérés. Toutefois, les réponses sont influencées par les modalités et le contexte d’utilisation et peuvent varier considérablement d’un individu à l’autre en raison de facteurs tels que la génétique, le microbiome et les habitudes alimentaires. Les compléments destinés à améliorer les performances doivent être soigneusement testés lors de l’entraînement ou de simulation de compétition avant d’être utilisés en compétition. L’ingestion involontaire de substances interdites dans le cadre des codes antidopage qui régissent le sport de haut niveau est un risque connu de la prise de compléments. La protection de la santé de l’athlète et la prise de conscience du danger potentiel doivent être prioritaires ; il est fortement recommandé de demander l’avis et l’aide de professionnels experts en la matière avant qu’un athlète ne commence à utiliser des compléments.

Evaluation modalities for the anatomical repair of chronic ankle instability
18/11/2022
Pietro Spennacchio, Christophe Meyer, Jon Karlsson, Romain Seil, Caroline Mouton & Eric Hamrin Senorski Link to the article Abstract. Purpose. Several evaluation modalities are reported in the literature dealing with the operative treatment of chronic ankle instability (CAI) both to establish the CAI diagnosis leading to the surgical indication and to assess the effectiveness of ankle stabilisation procedure. The purpose of this study is to present an overview of the pre- and postoperative evaluation modalities reported in the literature dealing with CAI operative treatment. The comprehensive analysis of the different modalities chosen by researchers is expected to suggest critical points in current evaluation ability of CAI surgical treatment. Methods. Systematic review of the literature on surgical treatment of CAI through anatomic procedures. Pubmed, Embase and Cochrane electronic databases were analysed, from 2004 to 2018. Results. One-hundred-and-four studies met inclusion in this systematic review. 88 out of 104 studies analysed preoperative mechanical laxity of the ankle to depict the ligamentous insufficiency related to the subjective feeling of functional instability. Stress radiographs and manual stress examination of the ankle were the two most common modalities to evaluate joint laxity, reported in 67 and 53 studies, respectively. Clinical Outcome Measurement Scales (COMs) is the most common evaluation modality (102 out of 104 studies) to assess CAI surgical outcome. The American Orthopaedic Foot and Ankle Society Ankle-Hindfoot scale (AOFAS) and the Karlsson score are the most frequent COMs, reported in the 66% and 33%, respectively of the included literature. The radiographic analysis of ankle laxity after stabilisation procedures is the second most frequent postoperative evaluation modality, reported in 55 out 104 studies. Conclusions. There is a lack of standardization among researchers related to both the criteria to establish the CAI diagnosis leading to the surgical indication and the modality chosen to evaluate the effectiveness of surgical treatment. Future standardization of evaluation modalities in the CAI population is desirable to increase consistency of reported data.

Applying ethical standards to guide shared decision-making with youth athletes
17/11/2022
Clare L Ardern, Hege Grindem, Guri Ranum Ekås, Romain Seil, Michael McNamee Link to the article Despite the vast quantity of information available to patients, parents and clinicians, high-quality information and knowledge remains in relatively short supply.1 The benefits of an active lifestyle are incontrovertible. However, youth athletes have substantial risk for sports-related injuries to the musculoskeletal system and the brain.2 3 These potential dangers are known to clinicians who are helping youth athletes and their parents make sound decisions about injury management and sports participation. In the face of these challenges, how does the clinician fulfil his or her duty of care to youth athletes? The aim of this editorial is to illustrate how different ethical standards can help guide better shared decisions in sports medicine clinical practice. Youth athletes are a particularly vulnerable group because their life plans are still developing. Adding to this complexity is an increasing trend towards professionalisation in youth sport. When arriving at a decision in a clinical dilemma, one or several ethical standards may help the decision-making team evaluate if a decision is ethically justifiable. The 2018 International Olympic Committee consensus on paediatric ACL injury4 outlined six ethical standards that may apply to different situations in sports medicine clinical practice.

Charge et risque de blessure dans le sport : Synthèse ReFORM de la déclaration de consensus du Comité International Olympique
14/11/2022
G. Guilhem a, b; F. Brocherie a,b; R. Siboni a, f, g; R. Seil a, c, d, f; G.Martens a; F. Delvaux a, e a - ReFORM IOC Research Centre for Prevention of Injury and Protection of Athlete Health, Paris, France b - Laboratory Sport, Expertise and Performance (EA 7370), French Institute of Sport (INSEP), Paris, France c - Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science (LIROMS), Luxembourg, Luxembourg d - Clinique du sport, centre hospitalier de Luxembourg, Luxembourg, Luxembourg e - Physical Medicine and Sport Traumatology Department, Sport S2, University and University Hospital of Liege, Liège, Belgique f - Department of Orthopedic Surgery, Centre hospitalier de Luxembourg, LuxembourggDepartment of Orthopedic Surgery, Maison Blanche Hospital, Reims University, Reims, France Lien vers l’article de synthèse RÉSUMÉLes athlètes de haut niveau sont exposés à des charges d’entraînement en constante augmentation et à des calendriers de compétitions de plus en plus denses. Les travaux de recherche récents indiquent que la gestion de la charge constitue un déterminant majeur du risque de blessure. Le Comité International Olympique a constitué un groupe d’experts pour examiner le niveau d’évidence scientifique de la relation entre la charge (définie au sens large comme intégrant des changements rapides de la charge d’entraînement et de compétition, la densité des calendriers des compétitions, la charge psychologique et les déplacements) et les problèmes de santé dans le sport. Cet article résume les résultats qui établissent un lien entre la charge et le risque de blessure chez les athlètes, et propose aux athlètes, aux entraîneurs et au staff des recommandations pratiques pour gérer la charge d’entraînement. Cette déclaration de consensus inclut des recommandations touchant à (1) la prescription de la charge d’entraînement et de compétition et (2) la surveillance de la charge d’entraînement et de compétition, le statut psycho-logique, le bien-être des athlètes et les blessures. Sur la base de ce travail, nous avons identifié des priorités de recherche.
Prefrontal Cortex Oxygenation During Endurance Performance: A Systematic Review of Functional Near-Infrared Spectroscopy Studies
09/11/2022
Jonas De Wachter, Matthias Proost, Jelle Habay, Matthias Verstraelen, Jesús Díaz-García, Philip Hurst, Romain Meeusen, Jeroen Van Cutsem and Bart Roelands Link to the article Introduction: A myriad of factors underlie pacing-/exhaustion-decisions that are made during whole-body endurance performance. The prefrontal cortex (PFC) is a brain region that is crucial for decision-making, planning, and attention. PFC oxygenation seems to be a mediating factor of performance decisions during endurance performance. Nowadays, there is no general overview summarizing the current knowledge on how PFC oxygenation evolves during whole-body endurance performance and whether this is a determining factor. Methods: Three electronic databases were searched for studies related to the assessment of PFC oxygenation, through near-IR spectroscopy (NIRS), during endurance exercise. To express PFC oxygenation, oxygenated (HbO2) and deoxygenated hemoglobin (HHb) concentrations were the primary outcome measures. Results: Twenty-eight articles were included. Ten articles focused on assessing prefrontal oxygenation through a maximal incremental test (MIT) and 18 focused on using endurance tasks at workloads ranging from low intensity to supramaximal intensity. In four MIT studies measuring HbO2, an increase of HbO2 was noticed at the respiratory compensation point (RCP), after which it decreased. HbO2 reached a steady state in the four studies and increased in one study until exhaustion. All studies found a decrease or steady state in HHb from the start until RCP and an increase to exhaustion. In regard to (non-incremental) endurance tasks, a general increase in PFC oxygenation was found while achieving a steady state at vigorous intensities. PCF deoxygenation was evident for near-to-maximal intensities at which an increase in oxygenation and the maintenance of a steady state could not be retained. Discussion/Conclusion: MIT studies show the presence of a cerebral oxygenation threshold (ThCox) at RCP. PFC oxygenation increases until the RCP threshold, thereafter, a steady state is reached and HbO2 declines. This study shows that the results obtained from MIT are transferable to non-incremental endurance exercise. HbO2 increases during low-intensity and moderate-intensity until vigorous-intensity exercise, and it reaches a steady state in vigorous-intensity exercise. Furthermore, ThCox can be found between vigorous and near-maximal intensities. During endurance exercise at near-maximal intensities, PFC oxygenation increases until the value exceeding this threshold, resulting in a decrease in PFC oxygenation. Future research should aim at maintaining and improving PFC oxygenation to help in improving endurance performance and to examine whether PFC oxygenation has a role in other performance-limiting factors.

Management of anterior cruciate ligament revision in adults: the 2022 ESSKA consensus part I—diagnostics and preoperative planning
07/11/2022
Thomas Tischer, Philippe Beaufilis, Roland Becker, Sufian S. Ahmad, Marco Bonomo, David Dejour, Karl Eriksson, Giuseppe Filardo, Matthias J. Feucht, Alberto Grassi, Adrian Wilson, Jacques Menetrey, Nicolas Pujol, Martin Rathcke, Romain Seil, Marc J. Strauss & Vincenzo Condello Link to the article Abstract. Purpose. The aim of this ESSKA consensus is to give recommendations based on evidence and expert opinion to improve diagnosis, preoperative planning, indication and surgical strategy in ACL revision. Methods. The European expert surgeons and scientists were divided into four groups to participate in this consensus. A “literature group” (four surgeons); “steering group” (14 surgeons and scientists); “rating group” (19 surgeons) and finally “peer review group” (51 representatives of the ESSKA-affiliated national societies from 27 countries). The steering group prepared eighteen question–answer sets. The quality of the answers received grades of recommendation ranging from A (high-level scientific support), to B (scientific presumption), C (low level scientific support) or D (expert opinion). These question–answer sets were then evaluated by the rating group. All answers were scored from 1 to 9. The comments of the rating group were incorporated by the steering group and the consensus was submitted to the rating group a second time. Once a general consensus was reached between the steering and rating groups, the question–answer sets were submitted to the peer review group. A final combined meeting of all the members of the consensus was held to ratify the document. Results. The literature review for the diagnosis and preoperative planning of ACL revision revealed a rather low scientific quality. None of the 18 questions was graded A and six received a grade B. The mean rating of all the questions by the rating group was 8.4 ± 0.3. The questions and recommendations are listed below. Conclusion. ACL revision surgery is a widely debated subject with many different opinions and techniques. The literature reveals a poor level of standardisation. Therefore, this international consensus project is of great importance. ESSKA - the European Society for Sports Traumatology, Knee Surgery and Arthroscopy Webpage

IOC Research Centres Meeting and 2nd ReFORM Prevention Days
02/11/2022
The Annual Meeting of the International Olympic Committee (IOC) Research Centres took place in Luxembourg, from October 11 to 14, along with the 10 other World Research Centres, located in South Africa, in Australia, Canada, Denmark, the United States, Great Britain, Japan, Norway, the Netherlands, and Qatar. This meeting allowed the ReFORM group - French-speaking Olympic Sports Medicine Research Network to present all its projects , but also to address the following topics: “The impact of the menstrual cycle and pregnancy on sports performance in women” - Dr. Juliana Antero, “Injury prevention in sprinters "Fulgur Project” - Dr. Gael Guilhem and even to discuss “News in the management of ACL injuries “ - Prof. Dr. Romain Seil. The participants of the meeting could learn more about the projects carried out in the other IOC Research Centres and to discuss the improvements/collaborations that could be undertaken about Injury Prevention and Protection of Athlete Health.

Results of a tri-national online survey on the current status of sports injury prevention among members of the German-Speaking Orthopaedic Sports Medicine Society (GOTS)
24/10/2022
C. Lutter 1; R. Seil 2, 3; R. Best 4; A. Gokeler 5; T. Patt 6; W. Krutsch 7; C. Grim 8; T. Tischer 1 1 - Department of Orthopedics, University Medical Center, Rostock, Germany 2 - Department of Orthopaedic Surgery, Centre Hospitalier de Luxembourg-Clinique d'Eich, Luxembourg, Luxembourg 3 - Luxembourg Institute of Health, Luxembourg. 4 - Sportklinik Stuttgart, Stuttgart, Germany 5 - Department Exercise & Health, Exercise Science and Neuroscience, University of Paderborn, Paderborn, Germany 6 - Bergman Clinics, Delft, Netherlands W Krutsch 7 - SportDocsFranken, Nürnberg; Department of Trauma Surgery, University Medical Centre Regensburg, Regensburg, Germany 8 - Department of Orthopedic, Trauma and Hand Surgery, Klinikum Osnabrück, Germany Link to the article Abstract. Objectives To assess the current opinions and state of knowledge in primary sports injury prevention among members of the German-Speaking Society for Orthopaedic and Traumatologic Sports Medicine (GOTS). Methods On 21 August 2019, a web-based questionnaire was sent to the members of the tri-national society GOTS (Austria, Germany and Switzerland). The survey was online until 21 November 2019 and included twenty-two questions, which were divided into five sections: 1) general importance of prevention (n = 4), 2) specifications of the study population (n = 3), 3) implementation of prevention (n = 8), 4) improvement opportunities in prevention (n = 4) and 5) future research areas (n = 3). Results A total of 272 participants completed the survey, representing a total survey participation of 17.7 % of all members. The study population consisted of orthopaedic surgeons (55 % with surgical and 21 % with non-operative orientation), medical students (10 %), physical therapists (8 %) and sports scientists (4 %). Ninety-four percent of all participants stated that they considered the importance of sports injury prevention to be “very high” (68 %) or “high” (26 %). However, almost 70 % of all participants stated that they spend less than one hour per week on injury prevention work. The term “prevention” was clearly defined and practicable for only 40 %, understandable but difficult to implement for 51 %, and unclear and difficult to implement for 9 % of the participants. Seventy-two percent of respondents were aware of existing prevention programs such as “Stop-X” or “FIFA 11 +”, whereas 28 % of participants were uninformed regarding these programs. Conclusions A strong divergence was identified between participants’ perception of the importance of sports injury prevention and the existing implementation of preventive measures. Future funding of prevention programs, expansion of research strategies for injury prevention and better financial reimbursement are of utmost importance.
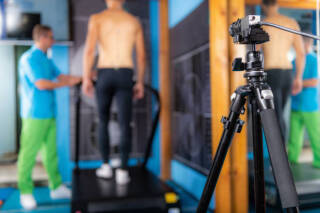
Does prevention pay off? Economic aspects of sports injury prevention: a systematic review
19/10/2022
Christoph Lutter 1, Christophe Jacquet 2, 3, Evert Verhagen 4, Romain Seil 2, 3, Thomas Tischer 1 1 - Department of Orthopedics, University Medical Center Rostock, Rostock, Germany 2 - Department of Orthopaedic Surgery, Centre Hospitalier de Luxembourg-Clinique d'Eich, Luxembourg, Luxembourg 3 - Luxembourg Institute of Health, Luxembourg, Luxembourg 4 - Amsterdam Collaboration on Health & Safety in Sports, Department of Public and Occupational Health, Amsterdam Movement Sciences, Amsterdam UMC, University Medical Centers – Vrije Universiteit Amsterdam, Amsterdam, The Netherlands Link to the article Abstract Objective To identify, summarise and critically assess economic evaluation studies on sports injury prevention strategies. Design Systematic review. Data sources PubMed, SportDiscuss. Eligibility criteria for selecting studies The current literature was searched following Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines. Economic analyses published since 2010 were checked for inclusion. The methodological quality of the studies was assessed using the Oxford Level of Evidence for economic and decision analysis; underlying randomised controlled trials (RCTs) were rated according to the Physiotherapy Evidence Database (PEDro) Scale, and risk of bias was assessed using the Revised Cochrane risk-of-bias tool. Results Ten studies fulfilled the inclusion criteria. The quality assessment revealed limited data quality. For trial-based analysis, underlying RCTs were of good quality and had a low risk of bias. Prevention concepts for general injury reduction showed effectiveness and cost savings. Regarding specific injury types, the analysis of the studies showed that the best data are available for ankle, hamstring and anterior cruciate ligament injuries. Measures using specific training interventions were the predominant form of prevention concepts; studies investigating these concepts showed cost-effectiveness with total cost savings between €24.82 and €462 per athlete. Conclusion Injury prevention strategies that were studied are cost-effective. However, estimates and outcomes vary throughout the included studies, and precluded pooling of existing data. Knowledge about the cost-effectiveness of evaluated prevention measures will help improve the acceptance and application of prevention initiatives.
Meniscal ramp lesions: rediscovering the past
17/10/2022
Riccardo Cristiani 1, 2; Anders Stålman 1, 2; Karl Eriksson 3, 4; Per Hamberg 4, Jack Lysholm 5 & Romain Seil 6, 7 1 - Department of Molecular Medicine and Surgery, Stockholm Sports Trauma Research Center, Karolinska Institutet, Stockholm, Sweden 2 - Capio Artro Clinic, FIFA Medical Centre of Excellence, Sophiahemmet Hospital, Valhallavägen 91, 11486 Stockholm, Sweden 3 - Department of Orthopaedics, Stockholm South Hospital, Stockholm, Sweden 4 - Karolinska Institutet, Stockholm, Sweden 5 - Umeå University, Umeå, Sweden 6 - Sports Clinic, Centre Hospitalier de Luxembourg-Clinique d’Eich, 78 Rue d’Eich, 1460 Luxembourg, Luxembourg 7 - Sports Medicine and Science, Luxembourg Institute of Research in Orthopaedics, Luxembourg, Luxembourg Link to the article Most of the relevant literature [5, 8, 15, 16, 21, 32, 37] reports that meniscal ramp lesions were first described by Strobel in 1988 [34]. Like many others, I (the first author) was under the same impression. However, during my visit to Prof. Romain Seil in Luxembourg (as a recipient of the ESSKA DePuy Knee Arthroscopy Fellowship), I learnt that these lesions were described in Sweden before by Per Hamberg, Jan Gillquist and Jack Lysholm [17]. It was back in 1983, when Hamberg et al. [17] published their study “Suture of new and old peripheral meniscus tears”. This prospective study was carried out from January 1977 to June 1980. The term “ramp lesion” had not been created at that time and that is why the authors called these lesions “vertical peripheral tears of the meniscus”. They diagnosed these tears through the Gillquist view with a 30- or 70-degree arthroscope and, if a tear was identified, a repair was performed through a mini-arthrotomy behind the posterior oblique ligament. Using their technique, the edges of the tear were debrided with a curette or a scalpel and two-to-four interrupted 2-0 Vicryl sutures were used to repair the meniscus back to the capsule. At a mean follow-up of 18 months, the authors reported clinical healing (no meniscal symptoms) in 84% of their patients. In addition, 64% of these patients underwent a second-look arthroscopy showing that all the repaired tears had healed. The authors therefore recommended the systematic exploration of the posteromedial compartment of the knee and repair of these tears, even in chronic cases, as they can be expected to heal after repair. These findings were quite revolutionary. At that time, several authors recommended total meniscectomy for peripheral tears of the meniscus in combination with ligament injuries [24, 25, 31], even though complete meniscectomy had already been associated with knee osteoarthritis and increased laxity [11, 14, 18, 26]. DeHaven et al. [12] and Cassidy and Shaffer [7] reported the healing of meniscal tears repaired soon after injury, but this was not proven by second-look arthroscopy. With their study, Hamberg et al. [17] were the first to describe the meniscus tear that was later named “ramp lesion” by Strobel [34]. According to Hamberg and Lysholm, one of the reasons why they discovered these tears was because of the routine use of the trans-patellar Gillquist portal which allowed easier exploration of the posteromedial ramp area. Even though, since the 1980s, the Swedish pioneers continued systematically to explore the ramp area and repair ramp lesions, these lesions were neither discussed nor the subject of research for almost two decades when they were eventually highlighted again in South Korea by Ahn et al. in the early 2000s [2, 3]. In a recent editorial commentary, Seil [29] hypothesised that one of the reasons for the two-decade neglect of these injuries might be that orthopaedic surgeons have focused too much on the anterior cruciate ligament (ACL) itself, thereby paying less attention to the other intra- or extra-articular structures. Despite knowledge of the association of these tears with ACL injuries, the systematic exploration of the posteromedial ramp area has not been emphasised for decades.

The SFA Datalake platform and Anterior Cruciate Ligament Tear Registry of the French Society of Arthroscopy (SFA): rationale, statutes and plans
10/10/2022
Mathieu Thaunat 1, Nicolas Bouguennec 2, Johannes Barth 3, Younes Boulhaia 4, Jaafar Sbihi 5, François-Xavier Gunepin 6, Romain Letartre 7, Thomas Rousseau 8, Etienne Cavaignac 9, Nicolas Pujol 10, Alexandre Netten 11, Caroline Mouton 12, the Francophone Arthroscopy Society (SFA) 13 Link to the article 1 - Ramsay Santé, Hôpital Privé Jean Mermoz, Centre Orthopédique Santy, 24 Avenue Paul Santy, 69008 Lyon, France 2 - Clinique du Sport de Bordeaux-Mérignac, Bordeaux, France 3 - Clinique des Cèdres, 21 Avenue Albert Londres, 38130 Echirolles, France 4 - Centre Hospitalier Lannion-Trestel, 22303 Lannion cedex, France 5 - Clinique Juge, 116 Rue J. Mermoz, 13008 Marseille, France 6 - Clinique Mutualiste de la Porte de l’Orient, 3 Rue Robert de La Croix, 56100 Lorient, France 7 - Ramsay Santé, Hôpital Privé la Louvière, 126 Rue de la Louvière, 59800 Lille, France 8 - Clinique Mutualiste Catalane, 60 Rue Louis Mouillard, 66000 Perpignan, France 9 - Clinique Universitaire du Sport, 1 Place du Docteur Joseph Baylac, 31300 Toulouse, France 10 - Centre Hospitalier de Versailles, 177 Rue de Versailles, 78150 Le Chesnay, France 11 - Groupe Santé CHC, Boulevard Patience et Beaujonc 2, 4000 Liège, Belgique 12 - Department of Orthopaedic Surgery, Centre Hospitalier Luxembourg – Clinique d’Eich, Luxembourg - Luxembourg Institute of Research in Orthopaedics, Sports Medicine and Science, Luxembourg 13 - 15 Rue Ampère, 92500 Rueil-Malmaison, France Abstract. SFA Datalake is the registry platform of the French Society of Arthroscopy (SFA). It was designed to collect and store data on arthroscopic orthopedic surgery and joint-sparing surgery in French-speaking countries. The anterior cruciate ligament (ACL) tear registry is the first registry to be set up based on SFA Datalake. Registries are intended to enable systematic standardized data collection, and provide information for surgeons to improve clinical practice and results. The ACL tear registry was designed in the light of guidelines, the literature and existing registries. Data are collected prospectively on a secure on-line application accessible via a computer or smartphone. Data collection is organized according to clinical examination results, preoperative findings, and follow-up data based on patient-administered subjective quality of life questionnaires. The pilot committee consists of 5 SFA board members, appointed for 2 years.

"Master of Science Sports Medicine" in Luxembourg in July 2022
05/10/2022
From 04 to 09 July 2022, the 4th module of the study course "Master of Science Sports Medicine" took place in Luxembourg under the direction of Dr. Christian Nührenbörger and Prof. Romain Seil. This course, jointly launched by the University of Krems (Austria) and the Society in Orthopaedic and Traumatologic Sports Medicine (GOTS) in 2018, comprises a total of 8 modules taking place in Austria, Germany, Switzerland and Luxembourg. As the field of sports medicine is not offered as an independent specialist training in the German-speaking countries, the aim of this innovative interdisciplinary Master programme is to offer interested doctors further training at the latest scientific level across the entire spectrum of sports medicine and thus to ensure competent medical care for athletes at all levels of performance - from amateur to professional sports.

Put the promotion of physical activity for people with non-communicable diseases on the political agenda in Luxembourg!
03/10/2022
Alexis Lion 1, 2; Anne Frisch 3, 4; Lucienne Thommes 5; Arno Bache 6; Anik Sax 7; Romain Seil 3, 2; Axel Urhausen 3, 2; Daniel Theisen 8; Charles Delagardelle 1, 3 1 - Federation Luxembourgeoise des Associations de Sport de Santé, Strassen, Luxembourg2 - Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science, Luxembourg, Luxembourg, Luxembourg3 - Centre Hospitalier de Luxembourg, Luxembourg, Luxembourg 4 - Medizinische Sport Gruppen fuer Personen mit Orthopaedischen & Metabolischen Stoerungen, Luxembourg, Luxembourg5 - Fondation Cancer, Luxembourg, Luxembourg6 - Ministère de la Santé, Luxembourg, Luxembourg7 - Oeuvre Nationale de Secours Grande-Duchesse Charlotte, Leudelange, Luxembourg8 - ALAN Maladies Rares Luxembourg, Bascharage, Luxembourg Link to the article Abstract Issue/problem. In 1984, cardiologists and cardiac patients created an association offering physical activity (PA) for people with cardiovascular diseases in Luxembourg (0.6 million inhabitants). During the last 20 years, several associations created therapeutic PA for people with a wide range of non-communicable diseases (NCDs). Today more than 70 hours of therapeutic PA are weekly offered. Nevertheless, the organization of these PA is incomplete and not enough patients benefit from it. Description of the problem. Sustainability of privately organized courses is challenging. Despite a governmental financial support, the organization of PA offer remains mainly based on the idealism of a limited number of volunteers. However, this kind of commitment is disappearing and jeopardizes a correct offer of therapeutic PA. Only a minority of physicians are referring their patients on a regular basis and only a minority of them are engaging in an active lifestyle. Results. A project was launched in 2013 to compile, monitor and promote the therapeutic PA offered by different associations. As a result of this project, six associations created a sport federation in 2016 destined to improve the organization of therapeutic PA for people with NCDs. In 2018, the federation obtained an increase in the financial support from the Ministry of Health. The same year, a campaign promoted the therapeutic PA but had no impact on the number of patients counselled about therapeutic PA (26.6%) and on the physician's knowledge of the therapeutical PA offer (21%). The federation is now trying to develop and implement deeper actions, such as a PA referral scheme. Lessons. The collaborative and synergetic work of the different associations offering PA for people with NCDs bundled their activities resulting in an increased consideration and support from the Ministry of Health. Nevertheless, structural improvements should be conducted to increase sustainably the number of physically active patients. Main messages The promotion and the organization of a valuable and sustainable therapeutic PA for patients with NCDs must be professionalized and publicly supported. . A larger strategic vision needs to be developed by the government and healthcare providers to organize and support preventive medicine in Luxembourg. .
CONSENSUS STATEMENT ON DATA TO BE ENTERED IN THE ACL TEAR REGISTRY: SFA - DATALAKE
29/09/2022
Nicolas Bouguennec 1, MathieuThaunat 2, Johannes Barth 3, Etienne Cavaignac 4, François-Xavier Gunepin 5, Romain Letartre 6, Alexandre Netten 7, Nicolas Pujol 8, Thomas Rousseau 9, Jaafar Sbihi 10, Caroline Mouton 7,11, the Francophone Arthroscopy Society (SFA) 12 Link to the article 1 - Clinique du Sport de Bordeaux-Mérignac, 33700 Merignac, France 2 - Ramsay Santé, Hôpital Privé Jean Mermoz, Centre Orthopédique Santy, 24 Avenue Paul Santy, 69008 Lyon, France 3 - Clinique des Cèdres, 21 Avenue Albert Londres, 38130 Echirolles, France 4 - Clinique Universitaire du Sport, 1 Place du Docteur Joseph Baylac, 31300 Toulouse, France 5 - Clinique Mutualiste de la Porte de l’Orient, 3 Rue Robert de La Croix, 56100 Lorient, France. Centre Hospitalier Lannion-Trestel, 22303 Lannion cedex, France 6 - Ramsay Santé Hôpital Privé la Louvière, 126 Rue de la Louvière, 59800 Lille, France 7 - Rue des Pervenches 30, Seraing 4100, Belgium 8 - Centre Hospitalier de Versailles, 177 Rue de Versailles, 78150 Le Chesnay, France 9 - Clinique Mutualiste Catalane, 60 Rue Louis Mouillard, 66000 Perpignan, France 10 - Clinique Juge, 116 Rue J. Mermoz, 13008 Marseille, France 11 - Department of Orthopaedic Surgery, Centre Hospitalier Luxembourg – Clinique d’Eich, Luxembourg - Luxembourg Institute of Research in Orthopaedics, Sports Medicine and Science, Luxembourg Abstract. Introduction: Anterior cruciate ligament (ACL) reconstruction is a frequent procedure, with room for improvement by rehabilitation measures and associated peripheral and meniscal surgeries that are currently under assessment, requiring follow-up. Outside France, there have been ACL registries for 20 years now. The French Arthroscopy Society (SFA) decided to set up an ACL tear registry within its SFA DataLake registry platform. Material and Method:. This article presents the methodology underlying the ACL Tear Registry: i.e., identification, definition and coding of essential and relevant data. A test phase comprised an initial assessment to improve data quality and overall coherence, to optimize data-entry time for patients and practitioners, who are the guarantors of the registry’s use and efficacy. Results:. The SFA DataLake ACL Tear Registry was made available to SFA members in December 2021. It aims to enable a review of practices for surgeons, early detection of failure of procedures and implants, with rates of failure and abnormal complications, and identification of prognostic factors for outcome, especially regarding original items that do not figure in previous registries. Conclusion:. SFA DataLake strikes a balance between “indispensable” and “original” items. The choice of contents and data quality is founded on a robust methodology with overall coherence, enabling analysis of large cohorts and comparisons with the literature and other registries. However, it remains to assess rates of data entry and item relevance as the Registry progresses.

The Effects of Mental Fatigue on Physical Performance: A Systematic Review
23/09/2022
Jeroen Van Cutsem, Samuele Marcora, Kevin De Pauw, Stephen Bailey, Romain Meeusen & Bart Roelands Link to the article Abstract Background Mental fatigue is a psychobiological state caused by prolonged periods of demanding cognitive activity. It has recently been suggested that mental fatigue can affect physical performance. Objective Our objective was to evaluate the literature on impairment of physical performance due to mental fatigue and to create an overview of the potential factors underlying this effect. Methods Two electronic databases, PubMed and Web of Science (until 28 April 2016), were searched for studies designed to test whether mental fatigue influenced performance of a physical task or influenced physiological and/or perceptual responses during the physical task. Studies using short (<30 min) self-regulatory depletion tasks were excluded from the review. Results A total of 11 articles were included, of which six were of strong and five of moderate quality. The general finding was a decline in endurance performance (decreased time to exhaustion and self-selected power output/velocity or increased completion time) associated with a higher than normal perceived exertion. Physiological variables traditionally associated with endurance performance (heart rate, blood lactate, oxygen uptake, cardiac output, maximal aerobic capacity) were unaffected by mental fatigue. Maximal strength, power, and anaerobic work were not affected by mental fatigue. Conclusion The duration and intensity of the physical task appear to be important factors in the decrease in physical performance due to mental fatigue. The most important factor responsible for the negative impact of mental fatigue on endurance performance is a higher perceived exertion.
The posterior cruciate ligament–posterior femoral cortex angle: a reliable and accurate MRI method to quantify the buckling phenomenon of the PCL in ACL‐deficient knees
21/09/2022
Renaud Siboni 1, 2 · Charles Pioger 1, 3 · Caroline Mouton 1, 4 · Romain Seil 1, 4, 5 Link to the article 1 - Department of Orthopaedic Surgery, Centre Hospitalier Luxembourg-Clinique d’Eich, 78 Rue d’Eich,1460 Luxembourg, Luxembourg 2 - Medicine and Science, Luxembourg, Luxembourg Department of Orthopaedic Surgery, Reims Teaching Hospital, Hôpital Maison Blanche, 45 Rue Cognacq-Jay, 51092 Reims, France 3 - Department of Orthopaedic Surgery, Ambroise Paré Hospital, Paris Saclay University, 9, avenue Charles de Gaulle, 92100 Boulogne-Billancourt, France 4 - Luxembourg Institute of Research in Orthopaedics, Sports Medicine and Science, Luxembourg, Luxembourg 5 - Human Motion, Orthopaedics, Sports Medicine and Digital Luxembourg Institute of Research in Orthopaedics, Sports Methods, Luxembourg, Luxembourg Abstract. Purpose. The aim was to validate a new MRI method to measure the buckling phenomenon of the PCL, representative of anterior tibial translation, by comparing its reliability and accuracy to identify anterior cruciate ligament (ACL)-deficient knees with existing methods. Methods. Patients were selected retrospectively and separated into a group of primary ACL injuries and ACL-intact knees. Exclusion criteria were: skeletal immaturity, PCL or a concomitant collateral ligament injury, signs of osteoarthritis (> 1 Kellgren and Lawrence score), tibial plateau fracture, previous ACL reconstruction or displaced meniscal bucket handle tear. The assessment of the curvature of the anterolateral bundle of the PCL was performed on T2 sagittal MRI slices according to 3 methods: (1) the PCL angle (PCLA), (2) the PCL inclination angle (PCLIA) and (3) a new method: the PCL-posterior cortex angle (PCL–PCA), representing the angle between the vertical part of the PCL-ALB and the posterior diaphyseal cortex of the femur. For each method, the inter- and intra-observer reliability was measured. The ability to discriminate both ACL-deficient and ACL-intact knees was evaluated using ROC curves. Results. Twenty-four patients were included in each group. Intra-observer reliability was excellent for all 3 methods (ICCs > 0.90). Inter-observer reliability was excellent for the PCL–PCA (ICC > 0.90) and good for the PCLA and the PCLIA (ICCs between 0.75 and 0.90). The PCL–PCA had the highest precision (lowest standard error of measurement: 2.7°). It yielded an excellent discrimination between the ACL and CTL groups (AUC 0.80 [0.67–0.93]) with the highest sensitivity (71% [52.8–89.2]) and specificity (88% [75–100]) for a positive threshold when the angle was ≤ 22.7°. The PCLA and PCLIA methods led to acceptable discrimination and lower sensitivities and specificities (PCLA: AUC 0.71, sensitivity 63%, specificity 79%, threshold ≤ 117.9°; PCLIA: AUC 0.62, sensitivity 50%, specificity 83%, threshold ≤ 21.4°). Conclusion. In comparison with previously described methods, the PCL–PCA was the most reliable and accurate method to measure the PCL buckling phenomenon on MRI in anterior cruciate ligament (ACL)-deficient knees. It offers an easy and objective method for the follow-up of ACL-injured patients and can therefore be recommended for routine use.

Origin and outcome of Osgood-Schlatter disease in preadolescent football players
19/09/2022
Hartmut Gaulrapp a; Christian Nuehrenboerger b, Lisa-Marie Walther c a - Facharztpraxis für Orthopädie und Kinderorthopädie München, Leopoldstr. 25, 80802 München, Gaulrapp Deutschland b - Clinique du Sport, Centre Hospitalier de Luxembourg, Luxemburg c - Biologische Arbeits- und Gesundheitspsychologie, Universität Konstanz, Walther Deutschland Link to the article Summary. Background. Chronic braking load on knee joints in football/soccer represents a risk for developing Osgood-Schlatter disease (OSD). This study examines the sportspecific risk for OSD and resting complaints after healing. Material and methods. All consecutive patients between 2015 and 2019 complaining on local pain and swelling at the TT due to sport acitivities were prospectively (level III) included. Patientś disciplines and dominant legs were recorded. Results. Among a total of 126 patients (101 boys, 25 girls) complaining an average of 6.7 months (0.5-36 months), average age at diagnosis 12.1 years (boys 12.5, girls 10.7 years), 116 were active in sports, 74 of them in disciplines with asymmetrical load like football/soccer, handball, track and field or fencing. Among 46 football players affected unilaterally 32 (69.6 % p < 0.01) had OSD at their standing leg, whereas in symmetrical disciplines the dominant leg was affected only in 8 out of 33 cases. Conclusion. Only in football/soccer the standing leg is far more prone to OSD than the shooting leg, whereas for symmetrical disciplines there is no statistical correlation. Male gender and age represent typical epidemiologic factors. Further risk or outcome criteria cannot be determined. BMI, growth spurts and muscle shortening are not significant co-aspects. OSD mean duration is 19.5 months with no significant difference in relation to discipline. 74 % of all MOS patients report on resting local pain in kneeing. Sport modification including more balanced load in shooting and standing could be a clue to secondary prevention.

Harcèlement et abus (violence non accidentelle) dans le sport : synthèse ReFORM de la position de consensus du Comité International Olympique
13/09/2022
A. Gagnon a, b; K. Seil a, c; A. Ruffault a, d, e; E. Anckaer t, f; R. Siboni g, h; R. Seil a, c, i; G. Martens a a - ReFORM IOC Réseau francophone olympique de la recherche en médecine du sport, France b - Institut National du Sport du Québec (INS), Montréal, QC, Canada c - Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science (LIROMS), Luxembourg d - Laboratory “Sport, Expertise, and Performance” (EA 7370), French Institute of Sport (INSEP), Paris, France e - Unité de Recherche Interfacultaire Santé & Société (URiSS), Université de Liège, Liège, Belgique f - Institut national du Sport, de l’Expertise et de la Performance (INSEP), Paris, France g - Department of Orthopedic Surgery, Centre hospitalier de Luxembourg, Luxembourg h - Department of Orthopedic Surgery, Maison Blanche Hospital, Reims University, Reims, France i - Clinique du sport, Centre hospitalier de Luxembourg, Luxembourg Link to the article RÉSUMÉMalgré ses avantages bien reconnus, le sport a aussi des influences négatives sur la santé, le bien-être et l’intégrité des athlètes dues à la violence non accidentelle perpétrée via le harcèlement et les abus. Tous les athlètes ont le droit de pratiquer un ‘sport sécuritaire', défini comme un environnement sportifrespectueux, équitable et exempt de toute forme de violence non accidentelle envers les athlètes. Pourtant, ces problèmes représentent un angle mort pour de nombreuses organisations sportives par peur d’un préjudice de réputation, ignorance, silenceou collusion. Cette déclaration de consensus élargit la Déclaration de consensus du CIO de 2007 sur le harcèlement et les abus sexuels dans le sport, en présentant des preuves supplémentaires de plusieurs autres types de harcèlement et d’abus—psychologique, physique et négligence. Les athlètes de tout âge et de tout type sont exposés à ces problèmes mais les études confirment que les athlètes de haut niveau, handicapés, enfants et lesbiennes/gay/bisexuels/transsexuels (LGBT) sont les plus exposés, que la violence psychologique est au cœur de toutes les autres formes et que les athlètes peuvent aussi en être les auteurs. Le harcèlement et la violence naissent de préjugés s’exprimant à travers des écarts de pouvoir. Les auteurs utilisent divers mécanismes interpersonnels, notamment la violence avec contact, sans contact/verbale, virtuelle, l’imprudence, l’intimidation et le bizutage. Une attention est portée aux risques particuliers auxquels sont exposés les athlètes enfants, les athlètes porteurs d’un handicap et les athlètes LGBT. Les impacts sur l’athlète individuel et sur l’organisation sont examinés. Lesparties prenantes du sport sont encouragées à considérer les paramètres sociaux plus généraux de ces problèmes, notamment les cultures du secret et de la déférence qui facilitent trop souvent les abus, plutôt que de s’intéresser simplement aux causes psychopathologiques. La promotion d’un sport sécuritaire est une tâche urgente et s’inscrit dans l’impératif international plus large d’une bonne gouvernance dans le sport. Une approche multiorganismes systématique de la prévention est la plus efficace, impliquant les athlètes, les membres de leur entourage, les directeurs sportifs, les médecins et thérapeutes, les éducateurs et les organismes de justice pénale. Des solutions structurelles et culturelles, ainsi que des recommandations pratiques, sont suggérées pour les organisations sportives, les athlètes, la médecine du sport et les disciplines apparentées, ainsi que les scientifiques et chercheurs spécialisés dans le sport.La prévention efficace et l’éradication des abus et du harcèlement envers les athlètes reposent sur l’efficacité du leadership par les grandes organisations sportives nationales et internationales.

The future of meniscus science: international expert consensus
07/09/2022
Nicholas N DePhillipo 1; Robert F LaPrade 2; Stefano Zaffagnini 3; Caroline Mouton 4, 5; Romain Seil 4, 5, 6; Philippe Beaufils 7 1 - Oslo Sports Trauma Research Center, 4014 Ulleval Stadion, 0806, Oslo, Norway. Nickd.atc@gmail.com. 2 - Twin Cities Orthopedics, Edina, MN, USA. 3 - Rizzoli Orthopedic Institutes of Bologna, Bologna, Italy. 4 - Department of Orthopaedic Surgery, Centre Hospitalier de Luxembourg, Clinique d'Eich, Luxembourg city, Luxembourg. 5 - Sports Medicine and Science, Luxembourg Institute of Research in Orthopaedics, Luxembourg city, Luxembourg. 6 - Human Motion, Orthopaedics, Sports Medicine and Digital Methods, Luxembourg Institute of Health, Luxembourg city, Luxembourg. 7 - Centre Hospitalier de Versailles, Versailles, France. Link to the article Abstract Purpose: The purpose of this study was to evaluate the main focus areas for research and development for furthering the state of meniscus science in 2021. Methods: An electronic survey including 10 questions was sent in a blind fashion to the faculty members of the 5th International Conference on Meniscus Science and Surgery. These faculty served as an expert consensus on the future of research and development areas of meniscus science. Survey responses were analyzed using descriptive statistics and ranking weighted averages were calculated to score survey questions. Results: Of the 82 faculty, 76 (93%) from 18 different countries completed the survey (84% male, 16% female). The highest ranked future research and development focus areas were meniscus repair, biologics, osteotomy procedures, addressing meniscus extrusion, and the development of new therapies for the prevention of posttraumatic osteoarthritis. Currently, the most 'valuable' type of biologic reported for meniscus treatment was platelet-rich plasma. The main reported global research limitation was a lack of long-term clinical outcomes data. The most promising emerging medical technologies for improving meniscus science were 3-D printing, personalized medicine, and artificial implants. Conclusions: This survey suggests that the future of meniscus science should be focused on meniscal preservation techniques through meniscus repair, addressing meniscal extrusion, and the use of orthobiologics. The lack of long-term clinical outcomes was the main reported research limitation globally for meniscus treatment. Future product development utilizing emerging medical technologies suggest the use of 3-D printing for meniscal transplants/scaffolds, personalized treatment, and bioengineering for artificial implants.
Mental Fatigue - Associated Decrease in Table Tennis Performance: Is There an Electrophysiological Signature?
02/09/2022
Jelle Habay, Matthias Proost , Jonas De Wachter, Jesús Díaz-García, Kevin De Pauw, Romain Meeusen, Jeroen Van Cutsem and Bart Roelands Link to the article Abstract Mental fatigue (MF) is a psychobiological state negatively impacting both cognitive and physical performance. Although recent research implies that some table tennis (TT) performance outcomes are impaired by MF, open skill sports such as TT require a more detailed overview of MF-related performance decrements. Moreover, research into MF and sport-specific psychomotor performance lacks the inclusion of brain-related measurements to identify MF mechanisms. Eleven experienced TT players participated in this randomized counterbalanced crossover trial. Participants were either required to perform an individualized Stroop task (MF condition) or watch a documentary (control condition). The primary outcomes were reaction time on a sport-specific visuomotor task and EEG activity throughout the trial. The subjective feeling of MF was significantly different between both conditions and confirmed that the MF condition induced the mentally fatigue state of participants (p < 0.001), though no behavioral indicators (i.e., decrease in performance on Stroop and flanker task) of MF. MF worsened reaction time on the visuomotor task, while other secondary measurements remained largely ambiguous. Spectral power (i.e., decreases in upper α band and θ band) was influenced by MF, while ERPs measured during the visuomotor task remained unaltered. The present study confirms that MF negatively impacts table tennis performance, specifically inhibitory stimuli during the visuomotor task. These findings also further augment our understanding of the effects of MF on human performance.

Effect of shoe cushioning on landing impact forces and spatiotemporal parameters during running: results from a randomized trial including 800+ recreational runners
01/09/2022
Laurent Malisoux 1, Nicolas Delattre 2, Christophe Meyer 3, Paul Gette 3, Axel Urhausen 4, Daniel Theisen 5 1 - Physical Activity, Sport & Health research group, Luxembourg Institute of Health, Luxembourg, Grand-Duchy of Luxembourg. 2 - Movement Sciences Department, Decathlon Sports Lab, Villeneuve d'Ascq, France. 3 - Human motion, Orthopaedic, Sports medicine and Digital methods unit, Luxembourg Institute of Health, Luxembourg, Grand-Duchy of Luxembourg. 4 - Sports Clinic, Centre Hospitalier de Luxembourg, Luxembourg, Grand-Duchy of Luxembourg. 5 - ALAN - Maladies Rares Luxembourg, Bascharage, Grand-Duchy of Luxembourg. Link to the article Abstract In a recent randomized trial including 800+ recreational runners, injury risk was lower in those who received the Soft shoe version compared to those using the Hard version (Hazard ratio = 1.52; 95% Confidence Interval = 1.07-2.16). Here, we investigated the effect of shoe cushioning on ground reaction forces (GRF) and spatiotemporal parameters in the same cohort, with a special focus on Vertical Impact Peak Force (VIPF) and Vertical Instantaneous Loading Rate (VILR). Healthy runners (n = 848) randomly received one of two shoe prototypes that differed only in their cushioning properties (Global stiffness: 61 ± 3 and 95 ± 6 N/mm in the Soft and Hard versions, respectively). Participants were tested on an instrumented treadmill at their preferred running speed. GRF data was recorded over 2 min. VIPF was higher in the Soft shoe group compared to the Hard shoe group (1.53 ± 0.21 vs. 1.44 ± 0.23 BW, respectively; p < 0.001). However, the proportion of steps with detectable VIPF was lower in the Soft shoe group (84 vs. 97%, respectively; p < 0.001) and Time to VIPF was longer (46.9 ± 8.5 vs. 43.4 ± 7.4 milliseconds, respectively; p < 0.001). No significant differences were observed for VILR (60.1 ± 13.8 vs. 58.9 ± 15.6 BW/s for Soft and Hard shoe group, respectively; p = 0.070) or any other kinetic variable. These results show that the beneficial effect of greater shoe cushioning on injury risk in the present cohort is not associated with attenuated VIPF and VILR. These GRF metrics may be inappropriate markers of the shoe cushioning-injury risk relationship, while delayed VIPF and the proportion of steps displaying a VIPF could be more relevant.

Utilisation de plasma enrichi en plaquette (PRP) en médecine du sport : synthèse ReFORM de la position de consensus du CIO
30/08/2022
L. de Garie a; J.- F. Kaux b, c; M. Crema b, d; D. Hannouche b, e; C. Nührenbörger b, f, g; R. Seil b, f, g; G. Martens b, c Link to the article a - Institut national du sport du Québec (INS), Montréal, QC, Canada b - ReFORM IOC Research Centre for Prevention of Injury and Protection of Athlete Health, Paris, France c - Physical Medicine and Sport Traumatology Department, Sport S2, FIFA Medical Centre of Excellence, FIMS Collaborative Centre of Sports Medicine, University and University Hospital of Liege, Liege, Belgique d - Institut national du sport, de l’expertise et de la performance (INSEP), Paris, France e - Department of Orthopaedic Surgery and Traumatology, Geneva University Hospitals, Geneva, Suisse f - Clinique du sport, centre hospitalier de Luxembourg, Luxembourg g - Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science, Luxembourg Introduction La déclaration de consensus du Comité International Olympique (CIO), relatif à l’utilisation de plasma enrichi en plaquettes (PRP) en médecine du sport (Figure 1), a pour objectif de présenter « les preuves scientifiques de l’efficacité clinique du PRP, son potentiel ergogène et sa sûreté, et de concilier toute disparité entre sa médiatisation et la science sous-jacente qui encourage son utilisation. » [1]. Bien que le consensus date de 2010, il reste aujourd’hui d’actualité, quel que soit le domaine d’application (muscles, tendons, articulations). Malgré des niveaux de preuves limités, les praticiens de l’appareil musculosquelettique ont commencé à utiliser le PRP pour traiter les problèmes de cartilage dès 2003. L’utilisation du PRP s’est accélérée, en particulier chez les athlètes souffrant de blessures sportives, notamment chez les compétiteurs de haut niveau pour lesquels un retour rapide à leur pratique est indispensable. Base scientifique Le principe de base de l’utilisation du PRP dans la pratique médicale est de faciliter l’action du plasma autologue et des protéines dérivées des plaquettes qui contiennent différents facteurs de croissance ayant un rôle important dans la cicatrisation des tissus lésés. De plus, il crée un échafaudage de fibrine dans la zone affectée pouvant agir comme une matrice temporaire pour la croissance et la différenciation cellulaire, contribuant ainsi à la réparation du tissu abîmé. Les différents produits de PRP sont des concentrés de plaquettes obtenus à partir de sang autologue et de moyens techniques de traitement extracorporel du sang tels que des récupérateurs/séparateurs de cellules sanguines, des centrifugeuses ou des méthodes de filtration. Le volume recueilli peut contenir des concentrations variables en facteurs de croissance et en globules rouges et blancs. Cette diversité va dès lors influencer la composition et l’efficacité potentielle du matériel biologique actif.

Failure of primary ACL repair with dynamic intraligamentary stabilization may result in a high risk of two-stage ACL reconstruction: a case series of ten patients
25/08/2022
Riccardo Cristiani , Caroline Mouton, Renaud Siboni, Charles Pioger, and Romain Seil Link to the article Abstract Purpose: Dynamic Intraligamentary Stabilization (DIS) is a technique for the repair of acute anterior cruciate ligament (ACL) injuries. The purpose of this study was to investigate the potential challenges of ACL reconstruction (ACLR) fol- lowing failure of DIS. Methods: A retrospective analysis of patients with failure of primary ACL repair performed with DIS was undertaken. Failure was defined as abnormal knee laxity (positive Lachman and/or pivot shift) and/or severely restricted range of motion. Medical and surgical records were reviewed and preoperative standard anteroposterior and lateral X-rays were assessed. Results: Between July 2015 and May 2022, 10 patients (3 males, 7 females, median age 28 years, range 18–52 years) with failure of DIS were referred to and surgically treated at a single centre. In four patients, single-stage ACLR was performed following the removal of the tibial monoblock. In six patients, arthrofibrosis and excessive tibial tunnel enlargement following the removal of the monoblock prevented single-stage ACLR. These patients underwent arthroscopic arthrolysis and tibial tunnel bone grafting as a first-stage revision procedure. Conclusion: In the present case series, single-stage ACLR was performed in only four (40%) of ten patients following failure of ACL repair with DIS. Arthrofibrosis and excessive tibial tunnel enlargement following the removal of the monoblock prevented single-stage ACLR in six (60%) patients. It is important for clinicians to inform patients that, in the event of failure of ACL repair with DIS, they may run a high risk of undergoing two-stage ACLR.

Risk factors and prevention strategies for shoulder injuries in overhead sports: an updated systematic review
22/08/2022
Matthias Wilhelm Hoppe , Joana Brochhagen, Thomas Tischer, Knut Beitzel, Romain Seil and Casper Grim Link to the article Abstract Purpose: The aim of this systematic review was to update the knowledge on risk factors and prevention strategies for shoulder injuries in overhead sports with special emphasis on methodological quality. Methods: All methodological procedures were performed in line with a previous systematic review by Asker et al. (2018). The literature search was conducted in the PubMed, Google Scholar, Cochrane, and SPORT-Discuss databases. Due to the risk of bias assessment, only studies with at least an acceptable methodological quality were included.A best-evidence synthesis was performed to clarify the evidence and direction of the risk factors and prevention strategies. Results: A total of nine studies were included in the data extraction process. One study had a high and eight stud- ies had an acceptable methodological quality. Seven cohort studies investigated risk factors and two randomised controlled trails evaluated prevention strategies. Moderate evidence was found for two non-modifiable (playing position, gender) and three modifiable factors (shoulder rotational strength, scapular dyskinesia, shoulder prevention programme) that were associated with the shoulder injury risk. All further risk factors had moderate and no associa- tion with risk (shoulder rotational ROM, joint position sense) or limited (history of shoulder/elbow pain, age, training experience, training volume, school grade, playing level), and conflicting evidence (setting). Conclusions: There is moderate evidence for two non-modifiable (playing position, gender) and three modifiable factors (shoulder rotational strength, scapular dyskinesia, shoulder prevention programme) being associated with the shoulder injury risk in overhead sports.

General Practitioners do not Counsel more Physical Activity after a Public Health Campaign
18/08/2022
Lion A. 1, 2, 3; Lethal J. 1; Delagardelle C. 1, 2, 3, 4; Seil R. 3, 5, 6; Urhausen A. 3, 6, 7; Theisen D. 8 Link to the article 1 - FÉDÉRATION LUXEMBOURGEOISE DES ASSOCIATIONS DE SPORT DE SANTÉ, Strassen, Luxembourg 2 - ASSOCIATION LUXEMBOURGEOISE DES GROUPES SPORTIFS POUR CARDIAQUES, Strassen, Luxembourg 3 - LUXEMBOURG INSTITUTE OF RESEARCH IN ORTHOPAEDICS, SPORTS MEDICINE AND SCIENCE, Luxembourg, Luxembourg 4 - CENTRE HOSPITALIER DE LUXEMBOURG, Department of Cardiology, Luxembourg, Luxembourg 5 - CENTRE HOSPITALIER DE LUXEMBOURG, Department of Orthopedic Surgery, Luxembourg, Luxembourg 6 - LUXEMBOURG INSTITUTE OF HEALTH, Sports Medicine Research Laboratory, Luxembourg, Luxembourg 7 - CENTRE HOSPITALIER DE LUXEMBOURG, Sports Clinic, Luxembourg, Luxembourg 8 - ALAN – MALADIES RARES LUXEMBOURG, Kockelscheuer, Luxembourg Summary A physical activity (PA) promotional campaign was launched in June 2018 to raise awareness of the health benefits of PA in patients with chronic diseases in Luxembourg. This study aimed to evaluate the behavior of general practitioners (GPs) regarding PA counselling before and after the campaign. The campaign consisted of advertisement broadcasts on national TV/radio in June and July 2018 and comprised a toolkit (flyers and a PA evaluation tool) sent in September 2018 to all medical doctors registered in Luxembourg. PA counselling behaviors were evaluated in 59 and 53 GPs who answered a standardized questionnaire before and after the campaign, respectively. Interviewed GPs declared having advised only a small proportion of their patients regarding PA participation before and after the campaign (29% and 24%, respectively; p<0.001). The campaign had no impact on the GPs’ awareness (21%) about the national program offering PA for patients with chronic diseases. Lack of time and knowledge were identified as the main barriers to engaging in PA counselling. Overall, GPs encouraged only a small proportion of their patients to engage more in PA, and the awareness campaign failed to change their PA counselling behavior, at least in the short term. Barriers to PA promotion within primary healthcare should be addressed before implementing new awareness campaigns targeting healthcare professionals.
“I never made it to the pros...” Return to sport and becoming an elite athlete after pediatric and adolescent anterior cruciate ligament injury—Current evidence and future directions
12/08/2022
Eric Hamrin Senorski · Romain Seil · Eleonor Svantesson · Julian A. Feller · Kate E. Webster · Lars Engebretsen Kurt Spindler · Rainer Siebold · Jón Karlsson · Kristian Samuelsson Link to the article Abstract The management of anterior cruciate ligament (ACL) injuries in the skeletally immature and adolescent patient remains an area of controversy in sports medicine. This study, therefore, summarizes and discusses the current evidence related to treating pediatric and adolescent patients who sustain an ACL injury. The current literature identifies a trend towards ACL reconstruction as the preferred treatment option for ACL injuries in the young, largely justified by the risk of further structural damage to the knee joint. Worryingly, a second ACL injury is all too common in the younger population, where almost one in every three to four young patients who sustain an ACL injury and return to high-risk pivoting sport will go on to sustain another ACL injury. The clinical experience of these patients emphasizes the rarity of an athlete who makes it to elite level after a pediatric or adolescent ACL injury, with or without reconstruction. If these patients are unable to make it to an elite level of sport, treatment should possibly be modified to take account of the risks associated with returning to pivoting and strenuous sport. The surveillance of young athletes may be beneficial when it comes to reducing injuries. Further research is crucial to better understand specific risk factors in the young and to establish independent structures to allow for unbiased decision-making for a safe return to sport after ACL injury.

Déficit énergétique relatif dans le sport (RED-S) : Synthèse ReFORM de la position de consensus du CIO
08/08/2022
Erik Sesbreno, Suzanne Leclerc, Anne-Charlotte Dupont, Eve Tiollier, Carole Maitre, Steve Hein, Valentin Lacroix, Romain Seil, Géraldine Martens Lien vers l’article de synthèse From : Mountjoy, M., Sundgot-Borgen, J. K., Burke, L. M., Ackerman, K. E., Blauwet, C., Constantini, N., Lebrun, C., Lundy, B., Melin, A. K., Meyer, N. L., Sherman, R. T., Tenforde, A. S., Torstveit, M. K., & Budgett, R. (2018). IOC consensus statement on relative energy deficiency in sport (RED-S): 2018 update. British Journal of Sports Medicine, 52(11), 687–697. IntroductionEn 2014, le CIO a publié une déclaration de consensus intitulée « Au-delà de la triade de l’athlète féminine : le déficit énergétique relatif dans le sport (RED-S) ». Le syndrome du RED-S fait référence à « une altération du fonctionnement physiologique due à un déficit énergétique relatif, et comprend mais sans s’y limiter, des perturbations du métabolisme, du cycle menstruel, de la santé osseuse, de l’immunité, de la synthèse des protéines et de la santé cardiovasculaire ». Le facteur étiologique de ce syndrome est une faible disponibilité énergétique (FDE). La publication de la déclaration de consensus sur le RED-S a stimulé l’activité dans le domaine de la science sur la triade de l’athlète féminine, incluant notamment une certaine controverse initiale suivie de nombreuses publications scientifiques portant sur :1. Les paramètres de santé identifiés dans le modèle conceptuel du RED-S 2. Le déficit énergétique relatif chez les athlètes masculins.3. Le mesure de la FDE.4. Les paramètres de performance identifiés dans le modèle conceptuel du RED-S Les auteurs du consensus du CIO sur le RED-S se sont retrouvés pour fournir un résumé mis à jour des progrès scientifiques intermédiaires dans le domaine du déficit énergétique relatif avec, pour objectif ultime, de stimuler les avancées dans la sensibilisation au RED-S, l’application clinique et la recherche scientifique afin de combler les lacunes des connaissances actuelles. Faible disponibilité énergétique (FDE) La FDE, qui sous-tend le concept du RED-S, est une inadéquation entre l’apport énergétique d’un athlète (alimentation) et l’énergie dépensée lors de l’effort, ne laissant pas suffisamment d’énergie pour soutenir les fonctions requises par le corps pour maintenir une santé et des performances optimales. En pratique, la disponibilité énergétique (DE) est définie ainsi :Disponibilité énergétique (DE)= Apport énergétique (AE) (kcal) –Dépense énergétique à l’effort (DEE) (kcal) /Masse maigre (MM) (kg)où la dépense énergétique à l’effort (DEE) est calculée comme l’énergie supplémentaire dépensée pendant l’effort, en plus de celle nécessaire à la vie quotidienne, et où le résultat global est exprimé par rapport à la masse maigre (MM), prenant ainsi en considération les tissus du corps les plus actifs sur le plan métabolique. Des essais en laboratoire rigoureusement contrôlés chez des femmes ont montré qu’une DE optimale pour une fonction physiologique saine est généralement atteinte pour une DE de 45 kcal/kg MM/jour (188 kJ/kg MM/jour). En même temps, bien que certaines mises en garde soient formulées au regard des réponses différentielles des divers systèmes du corps, bon nombre de ces systèmes sont essentiellement perturbés à partir d’une DE < 30 kcal/kg MM/jour (125 kJ/kg MM/jour), ce qui en fait historiquement un seuil cible pour la FDE. Toutefois, de récentes preuves suggèrent que ce seuil ne prédit pas l’aménorrhée chez toutes les femmes. En outre, et malgré les différences de corpulence et d’âge pubertaire, il est noté qu’une DE de 30 kcal/kg/MM équivaut à peu près au taux métabolique au repos (TMR) moyen.Puisque la FDE s’est révélée robuste pour expliquer les paramètres métaboliques et de santé sous-optimaux tant en laboratoire que sur le terrain,il semble logique qu’une évaluation de la DE puisse servir d’outil diagnostique dans la prévention et la prise en charge du RED-S.

Anatomic reconstruction of lateral ankle ligaments: is there an optimal graft option?
05/08/2022
Pietro Spennacchio, Romain Seil , Caroline Mouton, Sebastian Scheidt, Davide Cucchi Link to the article Abstract Purpose: Different graft options are available for the reconstruction of lateral ankle ligaments to treat chronic ankle instability (CAI), which fall in two categories: allografts and autografts. This study aims to provide an updated comparison of the clinical outcomes after stabilisation procedures using allografts and autografts, to correctly advise the clinician during the choice of the best material to be used for the reconstruction of the lateral ligamentous complex of the ankle. Methods: A systematic review was performed to analyse the use of autografts and allografts for anatomic reconstruction of the lateral ligamentous complex of the ankle in CAI patients. The presence of a postoperative assessment through outcome measures with proofs of validation in the CAI population or patient's subjective evaluation on the treatment were necessary for inclusion. The quality of the included studies was assessed through the modified Coleman Methodology Score (mCMS). Relevant clinical outcome data were pooled to provide a synthetic description of the results in different groups or after different procedures. Results: Twenty-nine studies (autograft: 19; allograft: 9; both procedures: 1) accounting for 930 procedures (autograft: 616; allograft: 314) were included. The average mCMS was 55.9 ± 10.5 points. The Karlsson-Peterson scale was the most frequently reported outcome scale, showing a cumulative average post- to preoperative difference of 31.9 points in the autograft group (n = 379, 33.8 months follow-up) and of 35.7 points in the allograft group (n = 227, 25.8 months follow-up). Patient satisfaction was good or excellent in 92.8% of autograft (n = 333, 65.2 months follow-up) and in 92.3% of allograft procedures (n = 153, 25.0 months follow-up). Return to activity after surgery and recurrence of instability were variably reported across the studies with no clear differences between allograft and autograft highlighted by these outcomes. Conclusions: The systematic analysis of validated CAI outcome measures and the patient's subjective satisfaction does not support a specific choice between autograft and allograft for the reconstruction of the ankle lateral ligamentous complex in CAI patients. Both types of grafts were associated to a postoperative Karlsson-Peterson score superior to 80 points and to a similar rate of patient's subjective satisfaction.
Medial meniscus ramp and lateral meniscus posterior root lesions are present in more than a third of primary and revision ACL reconstructions
03/08/2022
Amanda Magosch, Caroline Mouton, Christian Nührenbörger & Romain Seil Link to the article Abstract Purpose The purpose of this study was (1) to describe the meniscus tear pattern in anterior cruciate ligament (ACL)-injured patients, with a special focus on medial meniscus (MM) ramp lesions and lateral meniscus (LM) root tears and (2) to determine whether patient and injury characteristics were associated with meniscus tear patterns. Methods. Data from 358 cases of ACL primary and revision reconstruction surgeries were extracted from a center-based registry. During arthroscopy, the presence of associated meniscus lesions was documented by systematically inspecting the anterior and posterior tibiofemoral compartments. With a special focus on MM ramp lesions and LM root tears, groups of different injury tear patterns were formed. Chi-square tests were used to determine whether these groups differed with respect to various patient and injury characteristics, including gender, previous ipsilateral ACL injuries, the injury’s relation to sport, person contact during injury and the type of ACL tear. Median age at surgery and body mass index were compared between groups using the Kruskal–Wallis test. Significance was set at p < 0.05. Results. Two hundred and thirty-nine ACL injuries (67%) showed additional meniscal injuries, of which 125 (52%) involved the MM ramp and/or the LM root. Ramp lesions were more frequent in males (23% vs 12% in females, p < 0.01), in contact injuries (28% vs 16% in non-contact, p < 0.05) and in complete ACL tears (21% vs 5% in partial, p < 0.05). Combined injuries of the MM ramp and the LM root showed a higher percentage of contact injuries compared to non-contact injuries (10% vs 4%, p < 0.05). Conclusion. Two-thirds of all ACL injuries showed a concomitant meniscus injury, of which half involved the biomechanically relevant, but previously often undiagnosed RLMM or the PRLM. These findings provide evidence that until recently about half of ACL-associated meniscus injuries were not properly identified. Ramp lesions were more frequent in males, contact injuries and in complete ACL tears. These findings stress the need for a systematic assessment and a better understanding of the pathomechanism of these specific injuries which may have an important impact on knee biomechanics and the outcome of ACL reconstruction.

Cardiovascular Stress in Football Referees
02/08/2022
Urhausen A 1, 3, 4; Vivas JP 1 ; Lambert C 2 ; Weiler B 1 1 - CENTRE HOSPITALIER DE LUXEMBOURG, Sports Clinic , Luxembourg, Luxembourg 2 - UNIVERSITY OF WITTEN/HERDECKE, Department of Trauma and Orthopedic Surgery, Cologne Merheim Medical Center, Cologne, Germany 3 - LUXEMBOURG INSTITUTE OF HEALTH, Human Motion, Orthopaedics, Sports Medicine and Digital Methods, Luxembourg, Luxembourg 4 - LUXEMBOURG INSTITUTE OF RESEARCH IN ORTHOPAEDICS, SPORTS MEDICINE AND SCIENCE, Luxembourg, Luxembourg Link to the article Summary Problem: As opposed to athletes, the cardiovascular strain of referees during a competition is neither systematically explored nor included in their cardiovascular screening programs. Methods: Twenty-one referees from the two upper Luxemburgish football divisions were monitored during and after a match with an ambulatory Holter electrocardiogram. The results were compared to a sports cardiological check-up including a maximal incremental test on the treadmill. Results: During the match, the referees evolved in average 17%, 32%, 34% and 17% in the “regenerative” (<80% of the HR of individual anaerobic threshold, IAT), “extensive” (80 - 87.5% IAT), “intensive” (87.6 - 102.5% IAT) and “high intensive” (>102.5% IAT) zones. During the match, the mean (154 ± 11 bpm, mean ±SD) and maximal HR (180 ± 10 bpm) were only slightly lower than at the IAT (161 ± 9 bpm) and the end of the treadmill test (183 ± 11 bpm), respectively. ECG only revealed minor arrhythmias both during Holter monitoring and ergometry on the treadmill, but a higher incidence of premature beats during the 1.5h of the match than during the 15.5h off-match period. One referee showing significant ST segment depressions during the match suffered from a sudden cardiac exercise-associated event two years later. Conclusion: Football referees experience significant cardiovascular strain. A systematic endurance training is indispensable for football referees. Regular health monitoring, including a maximal exercise test on a treadmill ergometer, should be recommended not only for athletes but also for football referees.

Patient demographic and surgical characteristics in anterior cruciate ligament reconstruction: a description of registries from six countries - Luxembourg, USA, Denmark, Norway, Sweden, UK
29/07/2022
Heather A Prentice 1, Martin Lind 2, Caroline Mouton 3, Andreas Persson 4, 5, Henrik Magnusson 6, Ayman Gabr 7, Romain Seil 3, Lars Engebretsen 4, 5, Kristian Samuelsson 8, Jon Karlsson 8, Magnus Forssblad 9, Fares S Haddad 10, Tim Spalding 11, Tadashi T Funahashi 12, Liz W Paxton1, Gregory B Maletis 13 1 - Surgical Outcomes and Analysis, Kaiser Permanente, San Diego, California, USA 2 - Division of Sports Surgery, Department of Orthopaedics, Aarhus University Hospital, Aarhus, Denmark 3 - Department of Orthopaedic Surgery, Clinique d’Eich-Centre Hospitalier de Luxembourg, Luxembourg, Luxembourg 4 - Department of Orthopaedic Surgery, Oslo University Hospital, Oslo, Norway 5 - Norwegian Knee Ligament Registry, Orthopaedic Department, Haukeland University Hospital, Bergen, Norway 6 - Division of Physiotherapy, Department of Medical and Health Sciences, Linköping University, Linköping, Sweden 7 - Trauma and Orthopaedic Department, University College London Hospitals, NHS Foundation Trust, London, UK 8 - Department of Orthopaedic Surgery, Sahlgrenska Academy, University of Gothenburg, Sahlgrenska University Hospital, Mölndal, Sweden 9 - Stockholm Sports Trauma Research Center, Karolinska Institutet, Stockholm, Sweden 10 - Department of Trauma and Orthopaedics, University College London Hospitals, London, UK 11 - University Hospitals Coventry and Warwickshire (UHCW), Coventry, UK 12 - Department of Orthopaedics, Southern California Permanente Medical Group, Irvine, California, USA 13 - Department of Orthopaedics, Southern California Permanente Medical Group, Baldwin Park, California, USA Link to the article Abstract Objective Findings from individual anterior cruciate ligament reconstruction (ACLR) registry studies are impactful, but how various registries from different countries compare with different patient populations and surgical techniques has not been described. We sought to describe six ACLR registry cohorts to understand variation across countries. Methods Five European registries and one US registry participated. For each registry, all primary ACLR registered between registry establishment through 31December 2014 were identified. Descriptive statistics included frequencies, proportions, medians and IQRs. Revision incidence rates following primary ACLR were computed. Results 101 125 ACLR were included: 21 820 in Denmark, 300 in Luxembourg, 17 556 in Norway, 30 422 in Sweden, 2972 in the UK and 28 055 in the US. In all six cohorts, males (range: 56.8%–72.4%) and soccer injuries (range: 14.1%–42.3%) were most common. European countries mostly used autografts (range: 93.7%–99.7%); allograft was most common in the US (39.9%). Interference screw was the most frequent femoral fixation in Luxembourg and the US (84.8% and 42.9%), and suspensory fixation was more frequent in the other countries (range: 43.9%–75.5%). Interference was the most frequent tibial fixation type in all six cohorts (range: 64.8%–98.2%). Three-year cumulative revision probabilities ranged from 2.8% to 3.7%. Conclusions Similarities in patient demographics and injury activity were observed between all cohorts of ACLR. However, graft and fixation choices differed. Revision rates were low. This work, including >100 000 ACLR, is the most comprehensive international description of contemporary practice to date.

Sportverletzungen der unteren Extremität
27/07/2022
Sports injuries of the lower extremity J. Paul 1 · R. Seil 2, 3, 4 · T. Tischer 5 1 - Rennbahnklinik, Muttenz, Basel, Schweiz2 - Abteilung für Orthopädie, Centre Hospitalier de Luxembourg – Clinique d’Eich, d’Eich, Luxembourg, Luxemburg 3 - Sports Medicine and Science (LIROMS), Luxembourg Institute of Research in Orthopedics, Luxembourg, Luxemburg 4 - Human Motion, Orthopaedics, Sports Medicine and Digital Methods, Luxembourg Institute of Health, Luxembourg, Luxemburg 5 - Klinik für Orthopädie und Unfallchirurgie, Malteser Waldkrankenhaus St. Marien, Erlangen, Deutschland Link to the article Arthroskopie volume 35, pages 83–84 (2022) Liebe Leserin, lieber Leser, liebe Freunde des Sports, sportliche Aktivität hat in unserer modernen Gesellschaft einen hohen Stellenwert erreicht. Der Ausgleich des Arbeitsalltags findet oftmals bei sportlichen Aktivitäten statt. Hierbei ist die individuelle Spanne der Ausprägung sportlicher Aktivität enorm groß, und sowohl der Umfang als auch die Intensität variieren individuell stark. Etwas anders ist der Leistungssport zu betrachten, bei welchem das Erzielen einer hohen Leistung – meist im Wettkampf – im Fokus steht. Unabhängig davon, mit welchem Sport und auf welchem Niveau unsere Gesellschaft aktiv ist, treten sowohl Unfälle als auch Überlastungsschäden am Bewegungsapparat auf. Diese gilt es zu erkennen und zu therapieren. Dabei spielt die Prävention eine erhebliche Rolle, damit es gar nicht so weit kommt; dies wird jedoch in einem weiteren Themenheft der Arthroskopie und Gelenkchirurgie separat behandelt. Auch im Kindes- und Jugendalter nehmen akute Verletzungen im Sport wie Brüche, Prellungen und Zerrungen, aber eben auch Überbelastungsschäden des Stütz- und Bewegungsapparats zu. Leider stecken die präventiven Maßnahmen für diese Überlastungsschäden noch in den Kinderschuhen, und obwohl schon viele Konzepte bekannt und ausgearbeitet sind, findet nur eine unzureichende Umsetzung in der Praxis statt. Oftmals spielt ein übermäßiger Ehrgeiz in der Familie oder im Sportverein/-verband eine maßgebliche Rolle, und erste Zeichen von Überlastungsschäden werden übersehen oder ignoriert. Die Prävention von Unfällen und Überlastungsschäden am Bewegungsapparat spielt eine erhebliche Rolle Aufgrund der großen Relevanz dieser Themen freut es uns, dass wir für diese Ausgabe der Arthroskopie und Gelenkchirurgie ein Team von renommierten Autorengruppen gewinnen konnten, um ein abwechslungsreiches Heft zum Thema Sportverletzungen der unteren Extremität zu erstellen. Die Themen sind bewusst gleichmäßig topographisch zwischen Hüfte/Becken, Knie und Fuß/Sprunggelenk verteilt. Die Beiträge sollen gezielt einen pragmatischen Überblick sowohl von häufigen Pathologien als auch von selteneren Pathologien, welche häufig übersehen oder nicht erkannt werden, aufzeigen. Das „femoroazetabuläre Impingement im Sport“ und der „Leistenschmerz beim Sportler“ haben sich leider zu einem mit mittlerweile in hoher Frequenz auftretenden Beschwerdebild etabliert und sind differenzialdiagnostisch schwierig zu erfassen. Wir hoffen, dass Sie nach der Lektüre der beiden Artikel sicher mit diesen Pathologien umgehen können. Bezüglich des Kniegelenks soll Ihnen diese Ausgabe Einblicke in den „Hochleistungssport“ sowie einen Überblick über die „Osteochondrosis dissecans im Rahmen sportassoziierter Verletzungen“ geben. Eine häufig übersehene Problematik im Bereich der Unterschenkel ist das „chronische Logensyndrom beim Sportler“, und wir hoffen, dass Sie nach der Lektüre auch hier die Pathologie souverän diagnostizieren und ggf. behandeln können. Abschließend werden die „akuten und chronischen Läsionen der Peronealsehnen“ für Sie erläutert. Wir hoffen, wir konnten für Sie eine interessante Ausgabe der Arthroskopie und Gelenkchrirurgie mit dem Themenheft zu Sportverletzungen der unteren Extremität zusammenstellen und wünschen Ihnen viel Freude beim Lesen sowie Ihnen und Ihren Patienten einen verletzungsfreien Sport! Ihre Jochen Paul Romain Seil Thomas Tischer
Unusual Cause of Lumbar Pain in Elite Sports: Two Case Reports of Sacral Stress Fractures
22/07/2022
Hoffmann F. 1, Heinz L. 1, Mouton C. 1, 2, Seil R. 1, 2, 3, Nührenbörger C. 1, 2 1 - CENTRE HOSPITALIER DE LUXEMBOURG, Sports Clinic, Luxembourg, Luxembourg 2 - LUXEMBOURG INSTITUTE OF RESEARCH IN ORTHOPAEDICS, SPORTS MEDICINE AND SCIENCE, Luxembourg, Luxembourg 3 - LUXEMBOURG INSTITUTE OF HEALTH, Human Motion, Orthopaedics, Sports Medicine and Digital Methods, Luxembourg, Luxembourg Link to the article Summary Nonspecific lower back and buttock pain can significantly limit performance in athletes and can be of different origins. Sacral stress fractures are a rare and, in many cases, undiagnosed cause of lower back pain, which can lead to a substantial loss of time before a full return-to-sports is achieved with full athletic performance.The main risk factors of sacral stress fractures include repetitive full weight-bearing activities, short-term increases in exercise intensity or duration, and excessive energy deficit. Knowledge of the injury pattern, high clinical suspicion, and early MRI examination lead to a timely diagnosis. Therapeutically, load reduction with avoidance of high impact activities for at least 6 weeks is indicated initially, followed by dosed and progressive load increase. In parallel, supplementation with calcium and vitamin D is recommended. Athletes with recurrent stress fractures, regardless of region, should be evaluated for a “Female Athlete Triad” or its male counterpart, as well as endocrinologic risk factors. Preventive measures are possible for stress fractures but are not specific to sacral stress fractures. We describe two clinical case scenarios, one of a professional soccer player and one of an elite track and field athlete with sacral stress fractures as the cause of nonspecific lumbar pain.

Santé mentale chez les athlètes de haut niveau : Synthèse ReFORM de la position de consensus du CIO
18/07/2022
A. Ruffault a, b, c; A. Gagnon c, d; K. Seil c, e; R. Seil c, e, f; G. Martens c a - Laboratory “Sport, Expertise, and Performance” (EA 7370), French Institute of Sport (INSEP), Paris, France b - Unité de recherche interfacultaire santé & société (URiSS), université de Liège, Liège, Belgique c - ReFORM IOC Research Centre for Prevention of Injury and Protection of Athlete Health, CHU de Liège, 1, avenue de l’Hôpital, 4000 Liège, Belgique d - Institut national du sport du Québec (INS), Montréal, QC, Canada e - Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science (LIROMS), Luxembourg, Luxembourg f - Clinique du sport, centre hospitalier de Luxembourg, Luxembourg, Luxembourg Lien vers l’article de synthèse From : Reardon, C. L., Hainline, B., Aron, C. M., Baron, D., Baum, A. L., Bindra, A., … Engebretsen, L. (2019). Mental health in elite athletes: International Olympic Committee consensus statement. British Journal of Sports Medicine, 53(11), 667-699. RÉSUMÉLes symptômes et troubles de santé mentale sont courants parmi les athlètes de haut niveau, peuvent avoir des manifestations associées au sport au sein de cette population et affecter les performances. La santé mentale est inséparable de la santé physique, puisqu’il apparaît que les symptômes et troubles de santé mentale augmentent le risque de blessure physique et retardent la récupération ultérieure. Il n’existe pas de preuves ou de recommandations basées sur un consensus pour le diagnostic et la prise en charge des symptômes et troubles de santé mentale chez les athlètes de haut niveau. Le diagnostic doit différencier les traits de caractère propres aux athlètes de haut niveau des maladaptations psychosociales.Les stratégies de prise en charge doivent aborder tous les éléments contributifs aux symptômes de santé mentale et tenir compte des facteurs biopsychosociaux propres aux athlètes pour maximiser les bénéfices et minimiser les préjudices. La prise en charge doit impliquer à la fois le traitement des athlètes individuels affectés et l’optimisation des environnements dans lesquels les athlètes de haut niveau s’entraînent et concourent. Pour promouvoir une approche factuelle plus normalisée des symptômes et troubles de santé mentale chez les athlètes de haut niveau, un groupe de travail de consensus du Comité International Olympique a procédé à une évaluation critique de l’état actuel des connaissances scientifiques et a émis des recommandations.
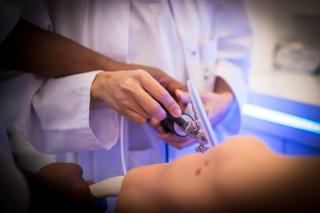
ACL surgical trends evolve in the last five years for young European surgeons: results of the survey among the U45 ESSKA members
15/07/2022
S. Cerciello 1, 2, 3 ; M. Ollivier 4 ; B. Kocaoglu 5 ; R. S. Khakha 6 ; R. Seil 7, 8, 9 1 - A. Gemelli University Hospital Foundation IRCCS, Catholic University, Rome, Italy 2 - Marrelli Hospital, Crotone, Italy 3 - Casa Di Cura Villa Betania, Rome, Italy 4 - Institute for Locomotion, Department of Orthopedics and Traumatology, Aix Marseille University, APHM, CNRS, ISM, Sainte-Marguerite Hospital, Marseille, France 5 - Department of Orthopaedics and Traumatology, Acibadem University Faculty of Medicine, Istanbul, Turkey 6 - King’s College, London, UK 7 - Department of Orthopaedic Surgery, Centre Hospitalier de Luxembourg-Clinique, D’Eich 78 Rue d’Eich, 1460 Luxembourg, Luxembourg 8 - Sports Medicine Research Laboratory, Luxembourg Institute of Health, 76 Rue d’Eich, 1460 Luxembourg, Luxembourg 9 - Sports Medicine and Science, Luxembourg Institute of Research in Orthopaedics, 76 Rue d’Eich, 1460 Luxembourg, Luxembourg Link to the article Abstract Purpose: Although the outcomes of ACL reconstruction are generally satisfying, there are several patients who do not regain their pre-injury sporting level and suffer persistent symptoms. Orthopaedic practice has evolved significantly over the last five years to address these drawbacks. The aim of the present survey was to analyze the changes in the approach to ACL reconstruction among a population of young ESSKA surgeons dedicated to ACL surgery. Methods: The survey was uploaded on the ESSKA website and was accessible to members under the age of 45. The ESSKA society has 1035 U45 members involved in multiple aspects of Orthopaedic practice. One hundred and forty questionnaires were returned. Several aspects of ACL surgery were investigated at baseline and 5 years prior. They included general details such as the volume of ACL reconstructions per surgeon per year, the graft choice in cases of low and high demanding patients, the technique for femoral tunnel drilling and the preferred device for femoral fixation. The approach to the management of damage to peripheral structures, as well as meniscal ramp and root tears were also investigated. Results: Hamstrings and quadrupled semitendinosus were the preferred graft choice in low-demanding patients (92.9%) while quadriceps tendon is gaining popularity in contact sport practitioners (from 4.3 to 10.7%). The percentage of surgeons using femoral screws had decreased from 37.9 to 29.3 while the percentage of those who used buttons increased from 52.9 to 69.3%. Extra-articular procedures (antero-lateral ligament (ALL) or lateral tenodesis have become popular. The percentage of surgeons who perform an additional peripheral reconstruction rose from 28.5 to 71.5%. Of those who perform the meniscal repair more than 50% of patients rose from 14.3 to 27.9%. Similarly, the percentage of surgeons who performed a medial meniscus ramp lesion repair rose from 29.4 to 54.7%. While the percentage of those who choose to perform a transtibial pull-out repair of lateral meniscus root tears significantly rose from 17.9 to 59.3%. Conclusions: The present survey among under 45 years old ESSKA surgeons yields some notable findings. The new evidence on the impact of injuries on peripheral structures and menisci is stimulating surgeons towards a more anatomic approach if identified at the time of ACL reconstruction. This evidence will probably influence future research and decision-making.

The 5th International Meniscus Conference comes to ESSKA's hometown of Luxembourg
13/07/2022
Link to the article On 7-9 July 2022, Luxembourg became the international capital of meniscus science and surgery when it hosted the 5th International Conference on Meniscus Science and Surgery, an event organised under the patronage of ESSKA. In 2010, the first edition of "The Meniscus" was held in Ghent (Belgium) under the lead of Rene Verdonk and Philippe Beaufils. The goal of this first congress was exclusively to share international expertise on this small but important piece of human tissue. Although meniscus surgery was already extremely frequent, science around the meniscus, its injuries or lesions and related surgical procedures was underrepresented at meetings and even in the scientific literature. Hence, it deserved to be promoted and the sub-title of the congress "From Cradle to Rocker" reflected this desire to cover all related topics, from basic research to clinical practice. The spirit of the first congress was reinforced at the following editions: Versailles in 2013, Porto in 2016 and Bologna in 2019. Because of the important activity around the meniscus among European surgeons and scientists and as home of the headquarters of many Institutions of the European Community and ESSKA, Luxembourg was the ideal place to organise the 5th edition, as well as to start an active collaboration with ESSKA. This edition was organised under the lead of Romain Seil, past president of ESSKA. More than 450 delegates from 40 countries including many of the world's most renowned specialists in the field met at the European Convention Center in Kirchberg for an intense scientific exchange. A true and unexpected success after two cancellations of the congress due to the sanitary crisis and related restrictions. A specific ESSKA session aimed at presenting the European state of the art in meniscus surgery. This session was an ideal opportunity to present the ESSKA European Specialists Core Curriculum and its specific aspects around knee surgery but also to promote the ESSKA consensus on degenerative and traumatic tears as well as to highlight some aspects of the ACL revision consensus related to the menisci. On top of the medical subjects, Mr Jean Asselborn, Luxembourg's Minister of Foreign Affairs provided a well-received lecture on the current political situation in Europe. Photo - Left to right: Savvas Papasavvas, Jean Asselborn and Romain Seil at the Meniscus Congress in Luxembourg.

Pushing the boundaries? Challenges and ethical considerations for hip and knee joint arthroplasty in elite athletes
11/07/2022
Géraldine Martens 1, Charles Pioger 2,3, Renaud Siboni 3,4 Matthieu Ollivier 5, Jean-Marie Fayard 6, Patrick Djian 7, Jean-Noel Argenson 5, Patricia Thoreux 8,9, Romain Seil 3 Link to the article 1 - Physical Medicine and Sport Traumatology Department, Central University Hospital of Liege, Liege, Belgium 2 - Department of Orthopaedic Surgery, Ambroise Paré University Hospital, Boulogne-Billancourt, France 3 - Department of Orthopedic Surgery, Centre Hospitalier de Luxembourg, Luxembourg, Luxembourg 4 - Department of Orthopedic Surgery, Hospital Maison Blanche, Reims, Champagne-Ardenne, France 5 - Institute of Locomotion, Hopital Sainte-Marguerite, Marseille, Provence-Alpes-Côte d’Azur, France 6 - Centre Orthopédique Santy, Hôpital Privé Jean Mermoz, Lyon, France 7 - Chirurgie Orthopédique et Traumatologique, Clinique Nollet, Paris, France8 - Institut de Biomécanique Humaine Georges Charpak, Arts et Métiers ParisTech, Université Sorbonne Paris Nord, Paris, France 9 - Pôle Médical, Institut National du Sport, de l’Expertise et de la Performance, Paris, France As the world of elite-level sports continues to evolve in parallel with the evolution of medicine, new and sometimes unexpected challenges keep arising. The duration of sports careers has increased along with life expectancy, as well as with sport training and competition loads. Sports activities may lead to a higher risk of severe osteoar- thritis (OA) in young patients due to discipline-specific factors such as high velocity/impact, frequent pivoting or repetitive joint loading.1 Therefore, specific medical attention and sometimes major surgical interventions such as total joint arthroplasty may be required in particular cases. Initially designed to improve quality of life during later decades of life, joint replacement surgery has been one of the most important medical achievements of the late 20th century. With many motivated young athletes pushing the limits to resume sports after surgery, the growing surgical expertise for minimally invasive procedures, and the evolution of implants, there is a trend for patients to undergo arthroplasty surgery at an increasingly younger age.2 In elite athletes, the risk of developing end-stage OA and undergoing arthroplasty is higher than the general population, often at an earlier age.1 3 Reports about the return to elite-level sports after joint replacement are scarce. A case series reported that elite athletes were able to resume sports activity at a professional level following hip resurfacing arthro- plasty, across a wide range of high-impact sports like tennis, soccer, track & field, and long-distance running.4 That series followed individual examples reported by the public press (eg, Andy Murray in tennis, Quentin Robinot in table tennis and Floyd Landis in cycling), thus receiving high media attention. It could be foreseen that sports medicine prac- titioners and orthopaedic surgeons will increasingly be faced by younger patients of various athletic levels expressing the desire to undergo hip or knee arthroplasty to continue their athletic careers at the highest possible level.

How to Tackle Mental Fatigue: A Systematic Review of Potential Countermeasures and Their Underlying Mechanisms
07/07/2022
Matthias Proost, Jelle Habay, Jonas De Wachter, Kevin De Pauw, Ben Rattray, Romain Meeusen, Bart Roelands, Jeroen Van Cutsem Link to the article Abstract. Introduction. Mental fatigue (MF) is a psychobiological state that impairs cognitive as well as physical performance in different settings. Recently, numerous studies have sought ways to counteract these negative effects of MF. An overview of the explored countermeasures for MF is, however, lacking. Objectives. The objective of this review is to provide an overview of the different MF countermeasures currently explored in literature. Countermeasures were classified by the timing of application (before, during or after the moment of MF) and type of intervention (behavioural, physiological and psychological). Methods. The databases of PubMed (MEDLINE), Web of Science and PsycINFO were searched until March 7, 2022. Studies were eligible when MF was induced using a task with a duration of at least 30 min, when they assessed MF markers in at least two out of the three areas wherein MF markers have been defined (i.e., behavioural, subjective and/or [neuro]physiological) and used a placebo or control group for the countermeasure. Results. A total of 33 studies investigated one or more countermeasures against MF. Of these, eight studies assessed a behavioural countermeasure, 22 a physiological one, one a psychological countermeasure and two a combination of a behavioural and psychological countermeasure. The general finding was that a vast majority of the countermeasures induced a positive effect on behavioural (e.g., task or sport performance) and/or subjective MF markers (e.g., visual analogue scale for MF or alertness). No definitive conclusion could be drawn regarding the effect of the employed countermeasures on (neuro)physiological markers of MF as only 19 of the included studies investigated these measures, and within these a large heterogeneity in the evaluated (neuro)physiological markers was present.
Paradigmewiessel an der Meniskuschirurgie
06/07/2022
Reportage Guy Seyler Vun en Donneschdeg bis e Samschdeg ass zu Lëtzebuerg en internationale medezinesche Kongress, wou et exklusiv ëm de Meniskus geet. Am Konferenzzentrum um Kierchbierg gi fir dës 3 Deeg 400 Dokteren a Wëssenschaftler aus iwwer 40 Länner erwaart. Den intensive Programm ass mat Exposéen, Debaten, Video - Demonstratiounen an Ateliere gutt gefëllt.Well d'Agrëffer um Meniskus zu den heefegsten Operatiounen zielen, ass dat e Sujet, deen och den normale Stierflechen dierft interesséieren. Aus deem Grond ass e Mëttwoch den Owend am Amphitheater vum CHL eng Konferenz zu deem Thema, wou jiddereen invitéiert ass, egal op Spezialist, Sportler oder einfachen Interessent. Original Publikatioun

Sportmedizinisches Novum
01/07/2022
Rédaction : Daniel BALTES Actuelle Ausgabe FLAMBEAU Die aktuelle Ausgabe der Deutschen Zeitschrift für Sportmedizin ist luxemburgisch. Denn: Alle sechs der veröffentlichten Beiträge entspringen einer Luxemburger Feder. Ein Blick auf die gewonnenen Erkenntnisse. Citius, altius, fortius – Das Motto der Olympischen Spiele (Schneller, höher, stärker) ist ein Ebenbild dessen, wofür der Sportstehen soll. Er strebt nach stetiger Verbesserung, nach dem Brechen von Bannen, dem Fällen von Rekorden. Auch in einer der wohl wichtigsten Rahmendisziplinen der Bewegungskunst herrschen diese Prinzipien. Die Sportmedizin ist stets auf der Suche nach neuen Errungenschaften und Erkenntnissen, nach Verbesserungen der eigenen Methoden. Diesem Ziel und damit auch dem Olympischen Motto wurde eine Gruppe Luxemburger Ärzte und Sportwissenschaftler Anfang dieses Jahres mehr als gerecht, als sie mit gleich sechs verschiedenen Beiträgen zur Sportmedizin ihr Forschungsfeldweiterentwickelten und zugleich eine Art Rekord aufstellten. Die Deutsche Zeitschrift für Sportmedizin wurde 1950 wiedergegründet und veröffentlicht seither regelmäßig mittlerweile monatlich wissenschaftlich-informative Berichte rundum das Thema der Sportmedizin. Dabei kam es schon in vergangenen Ausgaben immer wieder zu einzelnen Luxemburger Beiträgen. Die aktuelle Nummer liefert jedoch ein Novum: Jeder einzelne Beitrag in dieser Auflage entspringt nämlich einer Luxemburger Feder. Eine derart geballte Power aus Luxemburg gab es bis dato noch nie, weder in der Deutschen Zeitschrift für Sportmedizin noch in einem anderen sportmedizinischen Organ.

Le développement athlétique des jeunes : synthèse ReFORM de la position de consensus du CIO
30/06/2022
Mickey Moroz, Gabrielle Ostiguy, François Delvaux, Christian Nuehrenboerger, Stéphanie Nguyen, Jean-François Kaux, Maximilian Schindler, Romain Seil, Géraldine Martens Lien vers l'article complet From : Bergeron, M. F., Mountjoy, M., Armstrong, N., Chia, M., Côté, J., Emery, C. A., … Engebretsen, L. (2015). International Olympic Committee consensus statement on youth athletic development. British Journal of Sports Medicine, 49(13), 843–851. RÉSUMÉLa santé, la forme physique et les autres avantages de la pratique du sport chez les jeunes sont bien connus. Cependant, toutes les parties prenantes impliquées– plus particulièrement les jeunes athlètes–sont confrontées à des défis considérables lorsqu’elles tentent de maintenir une participation et une réussite inclusives, durables et agréables pour tous les niveaux d’accomplissement athlétique individuel. Dans le but de promouvoir une approche plus unifiée et fondée sur des données probantes du développement des jeunes athlètes, le CIO a procédé à une évaluation critique de l’état actuel de la science et de la pratique du développement des jeunes athlètes et a présenté des recommandations pour le développement de jeunes athlètes en bonne santé, résilients et performants, tout en offrant des possibilités de participation et de réussite sportives à tous les niveaux. Le CIO invite en outre toutes les instances dirigeantes de la jeunesse et des autres sports à adopter et à mettre en œuvreces principes directeurs recommandés.

Sport-related concussion in childhood and adolescence
28/06/2022
Nina Feddermann - Demont a,b, Andreas Meyer - Heim c, Christian Nuehrenboerger d,e, Philippe M.Tscholl f,g Link to the article a - Klinik für Neurologie und Klinisches Neurozentrum, Universität und Universitätsspital Zürich, Switzerland b - Swiss Concussion Center, Schulthess Klinik, Zürich, Switzerland c - Kinder-Reha Schweiz, Universitäts-Kinderspital Zürich, Switzerland d - Sports Clinic, Centre Hospitalier de Luxembourg – Clinique d’Eich, Luxembourg, Luxembourg Institute of Research in Orthopaedics, Sports Medicine and Science, Luxembourg f - Department of Orthopaedic Surgery and Traumatology, Geneva University Hospitals, Geneva, Switzerland g - ReFORM IOC Research Centre for Prevention of Injury and Protection of Athlete Health, University Hospitals Geneva, Geneva, Switzerland Summary Due to the specific anatomy and the development process, children and adolescents have a higher risk of concussion especially during sports. In the case of concussion, other structures, such as e.g. the equilibrium organ or the cervical spine, may also be affected, and therefore different symptoms may occur. Diagnosis should identify causes of all relevant symptoms and findings. There are special assessment criteria for children and adolescents. Therapy is carried out according to the guidelines of the respective medical societies. Physical and cognitive rest is recommended for the first 1-2 days. Return to school, education and sports should be controlled, gradual and symptom-limited with the support of the caring environment.

Running in Handball
27/06/2022
Leonard Achenbach, Lior Laver, Romain Seil & Kai Fehske Link to the article Abstract Handball and beach handball are two fast-paced, athletic ball games. It is characterized by a high number of quick high-intensity movements interspersed with regular periods of recover and either played on solid ground or sand. Handball is characterized by rapid changes of game speed, and therefore athletes have to be well trained in both aerobic and the anaerobic areas to be able to compete over 60 (handball) or 20 (beach handball) minutes. Team managers need to be aware of the growing frequency of these high-intensity phases during matches to train their players accordingly. Knowledge regarding prevention of injuries has improved substantially in the last 15 years. By means of reducing previously identified risk factors, injury risk and thus injury incidence could be shown to be reducible by implementing regular, neuromuscular injury prevention exercises into practices and before matches. This chapter demonstrates the most up-to-date findings.

Les lésions méniscales et l'arthrose du genou : 5 questions au Prof. Dr Romain Seil
24/06/2022
Dans cette vidéo le Prof. Dr Romain Seil répond aux 5 questions suivantes : C’est quoi un ménisque ?. Comment les lésions méniscales se produisent-elles ?. Quels sont les symptômes en cas de lésion du ménisque ?. Comment soigne-t-on une lésion du ménisque ?. L’arthrose après une atteinte du ménisque: une fatalité ?.

Continuous table tennis is associated with processing in frontal brain areas: an EEG approach
20/06/2022
A. Visser, D. Büchel, T. Lehmann, J. Baumeister Link to the article Abstract Coordinative challenging exercises in changing environments referred to as open-skill exercises seem to be beneficial on cognitive function. Although electroencephalographic research allows to investigate changes in cortical processing during movement, information about cortical dynamics during open-skill exercise is lacking. Therefore, the present study examines frontal brain activation during table tennis as an open-skill exercise compared to cycling exercise and a cognitive task. 21 healthy young adults conducted three blocks of table tennis, cycling and n-back task. Throughout the experiment, cortical activity was measured using 64-channel EEG system connected to a wireless amplifier. Cortical activity was analyzed calculating theta power (4–7.5 Hz) in frontocentral clusters revealed from independent component analysis. Repeated measures ANOVA was used to identify within subject differences between conditions (table tennis, cycling, n-back; p < .05). ANOVA revealed main-effects of condition on theta power in frontal (p < .01, ηp2 = 0.35) and frontocentral (p < .01, ηp2 = 0.39) brain areas. Post-hoc tests revealed increased theta power in table tennis compared to cycling in frontal brain areas (p < .05, d = 1.42). In frontocentral brain areas, theta power was significant higher in table tennis compared to cycling (p < .01, d = 1.03) and table tennis compared to the cognitive task (p < .01, d = 1.06). Increases in theta power during continuous table tennis may reflect the increased demands in perception and processing of environmental stimuli during open-skill exercise. This study provides important insights that support the beneficial effect of open-skill exercise on brain function and suggest that using open-skill exercise may serve as an intervention to induce activation of the frontal cortex.
An in-depth Analysis of the Side Hop Test in Patients 9 Months Following Anterior Cruciate Ligament Reconstruction
15/06/2022
Urhausen AP. 1,2, Gette P. 3, Mouton C. 2,4, Seil R. 2,3,4, Cabri J. 2,5, Theisen D. 6 1 - NORWEGIAN SCHOOL OF SPORT SCIENCES, Department of Sports Medicine, Norway, Oslo 2 - LUXEMBOURG INSTITUTE OF RESEARCH IN ORTHOPEDICS, SPORTS MEDICINE AND SCIENCE, Luxembourg, Luxembourg 3 - LUXEMBOURG INSTITUTE OF HEALTH, Department of Population Health, Human Motion, Orthopaedics, Sports Medicine and Digital, Luxembourg, Luxembourg 4 - CENTRE HOSPITALIER DE LUXEMBOURG, Department of Orthopaedic Surgery, Luxembourg, Luxembourg 5 - VRIJE UNIVERSITEIT BRUSSEL, Faculty of Medicine, Department Gerontology, Belgium, Brussel 6 - ALAN – MALADIES RARES LUXEMBOURG, Luxembourg, Luxembourg Link to the article Summary Purpose: The current criterion to evaluate 30-second side hop (SH) test performance following anterior cruciate ligament reconstruction (ACLR) is limited to the absolute number of jumps, neglecting the quality of execution. This study aims to assess the relevance of spatiotemporal and force plate derived parameters during the SH test. Methods: Seventeen patients nine months post-surgery and 27 healthy controls were instructed to realize a maximal number of jumps during 30 seconds over a 40 cm-distance. Spatiotemporal and force plate derived variables were recorded from two force plates: number of jumps, flight time, contact time, jump distance, vertical impact force, average and instantaneous vertical loading rate. Group (patients and controls) by leg (non-operated/first tested and operated/second tested) interactions were tested using a mixed model analysis of variance. Results: Patients performed a similar number of jumps compared to controls. No differences were found for spatiotemporal and force plate derived parameters, neither for lateral nor medial jumps. High interindividual spread of impact peak forces existed in both groups. Discussion: Patients 9 months following ACLR and successful rehabilitation can safely perform strenuous lateral hops similar to controls. Although the force plate derived parameters during the SH test were normalized compared to controls, impact peak forces outlined particularly high loading parameters in some participants. Applying biomechanical analysis in association to the commonly used clinical parameters helps to point out individual and potentially harmful loading strategies during the SH test.
The Clinical and Scientific Impact of an Institutional ACL Registry: Luxembourgish Experience
09/06/2022
Mouton C. 1,2, Nührenbörger C. 1,2, Magosch A. 1, Hoffmann A. 1, Pape D. 1,2,3, Seil R. 1,2,3 1 - CENTRE HOSPITALIER DE LUXEMBOURG, Sports Clinic, Luxembourg, Luxembourg 2 - LUXEMBOURG INSTITUTE OF RESEARCH IN ORTHOPAEDICS, SPORTS MEDICINE AND SCIENCE, Luxembourg, Luxembourg 3 - LUXEMBOURG INSTITUTE OF HEALTH, Human Motion, Orthopaedics, Sports Medicine and Digital Methods, Luxembourg, Luxembourg Link to the article Summary A standardized clinical pathway/registry for ACL injuries was developed in 2011 in our institution to monitor patient, injury and clinical profiles on a systematic basis regardless of operative or non-operative treatment. It was aimed from the very beginning for both patient care and research purposes. The aim of this paper is to share the Luxemburgish experience of this in-house registry, from its organization to the results of its publications. Our findings indicated that there was not only a big interindividual variability of physiological knee structures, but also of injury types, thereby showing that isolated ACL injuries were rare and that a personalized medicine approach of ACL injuries is required. Our findings about individual patient profiles, structural soft-tissue damage such as meniscal injuries, as well as factors contributing to the potential decompensation of knee laxity over time are some of the major discoveries over the last decade. Other findings such as the periodicity of ACL injuries in organized team ball sports, the high variability of knee morphology, references to understand the course/progression of ACL reconstructed patients and movement analyses are also of great value to reach high quality in patient care and continuous innovation in knee surgery.

The Luxembourg Institute for High Performance in Sports (LIHPS) recruits the Sports Scientist with a specialisation in biomechanics ( full time permanent contract )
03/06/2022
Main tasks: Cover all biomechanical topics in the day-to-day operations of the LIHPS, including testing and advising on best practices based on scientific principles to maximise sports performance . Provide support and advice to athletes and coaches on sports science topics, particularly in combat and racquet sports . Coordinate LIHPS support activities for the above-mentioned sports categories . Provide biomechanical expertise in the areas of strength & conditioning, return to sport and injury prevention. Reinforce the teams involved in testing and evaluating the individual abilities of the athletes to improve performance and individualise training and prevention programmes. Work as an integral member of a team of dedicated LIHPS experts in all relevant areas of high performance sport. Required qualifications: Master’s degree in sports science with a specialisation in biomechanics or a similar field related to high performance sports. 5 years of professional experience in high performance sports, preferably in sports biomechanics or a similar field. Advanced knowledge and experience in collecting and analysing in-lab and field-based biomechanical data (e.g., motion capture, force plates, IMU, EMG, etc.) of elite athletes. Advanced programming skills (Matlab or similar) for the analysis of biomechanical data. Continued professional development in a sport and exercise science related field. Knowledge and experience in the above-mentioned sports categories is an advantage. Certification as a sports coach is an advantage. Fluency in English and French or German is required, Luxembourgish is an advantage. Flexibility and excellent communication skills Interested candidates are requested to send their applications with CV, cover letter and copies of certificates and diplomas by 24 June 2022 to: Luxembourg Institute for High Performance in Sports M. Alwin de Prins3, route d'ArlonL-8009 Strassen or info@lihps.lu .

Winners of the KSSTA Best Paper Award 2022
30/05/2022
We are proud to annoce that Dr. Caroline Mouton and Prof. Dr. Romain Seil are the winners of the KSSTA Best Paper Award 2022 as co-authors by the paper written by Prof. Dr. Michael T. Hirschmann. Congratulations! Link to the article Photo from the left: Thomas Bauer - ESSKA Congress 2022 President, Jacques Menetrey - ESSKA Past President, Dr. Caroline Mouton and Prof. Dr. Michael T. Hirschmann

À l'attention des Kinésithérapeutes, Médecins du Sport et Médecins Généralistes
20/05/2022
De la part de Docteur Pietro Spennacchio, Chirurgien Orthopédiste - Clinique du Sport Eich - CHL Chers Collègues, Je suis actuellement engagé dans une étude faisant partie d'un projet de doctorat de recherche sur l'instabilité de cheville, en convention avec la Sahlgrenska University of Gothenburg. Mon objective est de valider un score fonctionnel utile pour évaluer l'efficacité des différents traitements conservateurs/chirurgicales proposées pour l'instabilité de cheville, et ainsi aider le choix des meilleures stratégies thérapeutiques possibles. Je me permets donc de demander votre support à tel projet en mettant en contact avec moi les patients souffrant d’une instabilité chronique de la cheville (histoire d’entorses récidivantes de la cheville depuis plusieurs mois) afin de pouvoir recueillir les données nécessaires à l’etude Je tiens à souligner que l’étude n’a pas comme objective de recruter de patients pour un éventuel traitement chirurgical, mais uniquement l’analyse de l’état actuel des sujets à travers un examen objective et la compilation de questionnaires inhérents la pathologie de la cheville. Mon contact direct pour tous renseignements ultérieurs et/ou pour les patients intéressés à telle évaluation est le suivant : spennacchio.pietro@chl.lu Merci de votre support !

Gestion de la douleur chez les athlètes de haut niveau : synthèse ReFORM de la position de consensus du CIO
16/05/2022
Link to the article P.M. Tscholl, B. Forthomme, J. Cabri, S. Le Garrec, J.-F. Kaux, P. Edouarda, A. Bourgeois, R. Seil, G. Martens Introduction La déclaration de consensus du CIO sur la gestion de la douleur chez les athlètes de haut niveau émet des recommandations visant à harmoniser les pratiques et à promouvoir une approche multimodale de cette problématique. L’utilisation importante d’antalgiques et d’anti-inflammatoires lors de compétitions de haut niveau montre combien la douleur est un aspect important de la vie des sportif.ve.s. Plusieurs sondages auprès des médecins du sport en charge d’athlètes de haut niveau ont montré que ces médicaments ne sont pas uniquement prescrits pour traiter la blessure et diminuer la douleur ressentie, mais également pour poursuivre la pratique sportive, voire même prévenir des douleurs qui pourraient survenir à l’effort. La bonne gestion de la douleur chez l’athlète de haut niveau reste un champ hautement complexe, nécessitant des notions tant pharmacologiques que cliniques. Une approche multidisciplinaire somatique est nécessaire dans les douleurs chroniques, accompagnée d’une prise en charge biopsychosociale, tout en appliquant les conventions et les règles de bonnes pratiques et de lutte contre le dopage pour maintenir la santé physique et mentale de l’athlète. Faire le bon diagnostic pour choisir le bon traitement L’origine de la douleur, son historique, les facteurs impliqués, représentent la base pour la compréhension et le choix du traitement. Une douleur aiguë post-traumatique ne peut pas être comparée à une douleur chronique, ni à une douleur récurrente ou de type surcharge (Tableau I). L’information douloureuse peut parvenir des tissus endommagés ou d’une inflammation, souvent concomitante en post-traumatique (douleur nociceptive ou inflammatoire), du nerf lui-même (douleur neuropathique lors d’une Stratégies de prise en charge de la douleur. Les options non-pharmacologiques ou non-médicamenteuses sont à envisager en première intention ; elles prennent en compte les facteurs neurobiologiques, psychologiques et cognitifs, contextuels et environnementaux. L’éducation du patient joue un rôle primordial, non seulement pour la compréhension de l’origine multifactorielle de la douleur mais aussi pour optimiser la compliance au traitement. Les différentes modalités thérapeutiques, actives ou passives, s’envisagent de manière individuelle Monitorer l’efficacité du traitement choisi L’objectif du traitement vise à ramener l’athlète à son meilleur niveau de performance, sans douleur et en évitant la récidive. Le/la sportif.ve doit comprendre que l’efficacité thérapeutique n’est pas toujours corrélée avec la guérison tissulaire et ne dépend pas uniquement de l’entrée nociceptive. La communication des objectifs et des différentes étapes de la prise en charge ainsi que la responsabilisation de l’athlète dans ce processus restent essentielles pour maintenir sa confiance et sa Situation particulière Les parathlètes constituent un groupe particulier dans la prise en charge de la douleur. En effet, ils présentent régulièrement des douleurs fantômes ou localisées sur un moignon, parfois de la spasticité ou encore des douleurs en lien avec leur déficience spécifique. Une approche spécialisée s’avère essentielle pour traiter des douleurs chroniques et/ou neuropathiques dans ce contexte. Questions éthiques et culturelles La perception de la douleur ainsi que sa verbalisation peuvent changer en fonction de l’origine de l’athlète, du type de sport pratiqué mais aussi du sexe. Le choix libre et volontaire du/de la sportif.ve de participer à une activité physique « malgré la douleur » ne semble pas toujours évident. Le corps médical se doit d’appliquer le code médical du CIO, insistant sur le fait que « la santé et le bien-être des athlètes sont prioritaires et l’emportent sur les aspects compétitifs, économiques,...

Way for improvement: Primary survey on concussion knowledge of sports stakeholders in three European countries
03/05/2022
Link to the article A.Thibaut, J.-F.Kaux, G.Marten, A.Urhausen, P.Tscholl, D.Hannouche, S.Le Garrec, M.Crema, L.Winkler, J.Cabri, S.Leclerc Objective. Evaluate knowledge on concussion management in three countries participating to the ReFORM group. Methods. In this cross-sectional survey, the target population consisted of eighty-five participants of an educational conference on concussion's management given in Switzerland, Luxembourg and Belgium in September 2019. Thirty-eight participants responded an online anonymous survey out of 85 (45%). They answered to 22 multiple choice questions regarding their knowledge on concussion diagnosis, management and treatment prior the conference. Two were excluded (not working in sport nor healthcare professionals). Participants were medical doctors (28%), healthcare professionals (41.5%), coaches (14%), physical trainers (5.5%), or stakeholders from different positions in sport (11%). Numbers of years working in sport varied from 34% > 15 years, 41% for 5–15 years and 25% for 0–4 years. Level of sport involved included recreational, international and professional athletes. Results. In total, 50% of the participants were not aware of international guidelines for the management of concussions, 76% and 83% were not familiar with the stepwise “return to sport” and “return to learn” protocols, respectively. Ninety-two percent responded that an education program for athletes would be necessary. Important discrepancies were found on who is responsible for recognition and diagnostic of concussion (e.g., physician, physiotherapist or coach) and its assessment and management tools. Conclusion. This pilot survey highlights the lack of common knowledge about concussion diagnosis, management and treatment. A larger survey is underway to better identify specific needs of each country in the ReFORM group and offer adapted training programs.
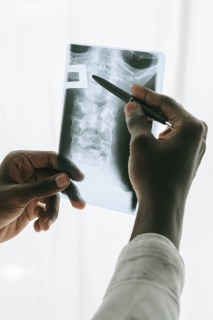
L’instabilité controlatérale du bassin, le valgus du genou et l’hyperpronation du pied sont-ils des signes cliniques fréquemment observé chez les coureurs à pied blessés ?
27/04/2022
Presentation on the Congrèss National de Médicine et traumatologie du sport Amandine Bodson, Jan Cabri, Roland Krecke, Paul Gette ABSTRACT Le nombre de coureurs augmente considérablement chaque année et, par conséquent, le nombre de blessures de surcharge. De précédentes recherches ont démontré que certains paramètres cinématiques peuvent être liés a ces blessures. Trois paramètres cinématiques peuvent engendrer ces lésions : l’instabilité controlatérale du bassin, le valgus du genou et l’hyperpronation du pied. Objectifs : Identifier si les trois variables cinématiques susmentionnées sont des signes cliniquement pertinents d'une éventuelle blessure. Vérifier si on observe des différences dans la cinématique entre les membres inférieurs. Enfin, analyser s'il existe une corrélation entre la localisation de la lésion et les trois paramètres cinématiques pour les jambes blessées des coureurs. Des analyses biomécaniques de la course sur tapis roulant ont été réalisées sur 50 coureurs blessés et 13 coureurs non blessés à l'aide d'un système d’analyse de mouvement tridimensionnel (9 caméras Miqus System, Qualisys AB, Gothenburg, Suède). Sept variables cinématiques, pendant la phase d'appui, ont été comparées entre les coureurs blessés et les coureurs sains tout en contrôlant leur vitesse de course. Afin d'éliminer la redondance et d'augmenter la puissance de notre modèle statistique, seules trois variables sont restées pertinentes : l'angle maximal d'ADD de la hanche, l'angle maximal d'ADD du genou et l'angle maximal d'éversion de l'arrière-pied. Résultats : La MANCOVA n'a révélé aucune différence significative entre les groupes de coureurs blessés et non blessés(p=0,164)pourlesvariablescontrôlantl’instabilitécontrolatéraledubassin,levalgusdugenouet l’hyperpronation du pied avec la vitesse comme covariable. Cependant, des différences significatives entre les participants masculins et féminins pour le pic d'ADD de la hanche (p=0.006) ont été trouvées. Les femmes démontrent une ADD de hanche plus importante que les hommes (moyenne= 16,9° ; SD 3,8 et 14° ; SD 4,0 respectivement). La vitessedecourseainfluencéplusieursvariablescinématiques,àsavoirl'ADDmaximaledelahanche(p=0,002)et l'éversion maximale de l'arrière-pied (p= < 0,001). Les résultats du test T de l'échantillon apparié ont révélé que les membres inférieurs de la population de coureurs blessés ne présentaient pas de différences significatives en ce qui concerne les angles du pic d'ADD de la hanche (p=0,372), du genou (p=0,343) et du pic d'éversion de l'arrière-pied (p=0,804) lors de la phase d’appui. Quant à l'analyse de régression logistique multiple, la relation entre l'ensemble des variablesetlalocalisationdelablessuren'amontréaucunerelationsignificativepourlepied(p=0,535),la jambe inférieure (p=0,017), le genou (p=0,465) ou la hanche (p=0,109). Conclusion : Les paramètres cinématiques de l’instabilité controlatérale du bassin, du valgus du genou et de l’hyperpronation du pied sont influencés par le type de population, la vitesse de course et la localisation de la blessure. Une sous-classification de la présentation cinématique de chaque blessure liée à la course à pied pourrait aider les cliniciens dans leur processus de raisonnement clinique et pourrait cibler la stratégie d'intervention.

Visit from Norwegian School of Sport Sciences
25/04/2022
On the 25th of April 2022, we received a visit from three researchers of the Sports Medicine Department of the Norwegian School of Sport Sciences (NSSS): Caroline Kooy Tveiten, Marie Pedersen and Anouk Urhausen. All three are connected to the Oslo Sports Trauma Research Center and work in the field of ACL injuries. Meeting in the Sportfabrik (Differdange). Left to Right: Caroline Kooy Tveiten, Marie Pedersen and Anouk Urhausen


Luxembourg Academy of Sports Medicine, Physiotherapy & Science - Program
15/02/2022
The program of the 2022 sports science lectures is online Link to the program

Dr Caroline MOUTON is the winner of the JEO Young Researcher Award in Clinical Science
09/02/2022
The Jury of the JEO Award for Young Researcher in Clinical Science has selected Dr Caroline MOUTON as the winner of the JEO Award for Young Researcher in Clinical Science. https://jeo.esska.org LIROMS is very proud to work with Dr Caroline MOUTON as a scientific collaborator from CHL. Congratulations to her! Link to the article

The knee in elite level sports
09/02/2022
Link to the article Magosch A., Mouton C., Seil R., Tischer T., Urhausen A.P., 17 January 2022 Arthroskopie - https://doi.org/10.1007/s00142-022-00517-7 The knee joint is one of the most frequently injured body regions in many sports. Particularly in elite sports, knee injuries are often severe injuries accounting for long periods of absence from several weeks to months and significantly influencing the athlete’s career. In addition to the acute injury the high risk of recurrent injuries and long-term effects as well as secondary injuries and a continuing high impact on the knee joint play an important role in elite sports. A better understanding of the injury circumstances and identification of risk factors are therefore crucial to improve primary prevention strategies. Furthermore, a comprehensive understanding of the structural damage occurring after an injury is also necessary to continually optimize therapeutic interventions. The rapid development of technology in recent years has considerably contributed to a better understanding of the total amount of knee injuries and their origin. Due to the rapid improvement of novel therapeutic and particularly surgical procedures, medicine is increasingly succeeding in helping elite athletes to regain their previous performance level even in the case of complex injuries; nevertheless, professional and elite athletes require individually adapted treatment options and rehabilitation measures in order to ensure a rapid return to sport.
Osteochondrosis dissecans of the knee joint in the athlete
09/02/2022
Brockmeyer M., Nührenbörger C., Seil R., Madry H. Osteochondrosis dissecans am Kniegelenk beim Sportler. Arthroskopie (2022). https://doi.org/10.1007/s00142-022-00515-9 Link to the article Abstract The treatment of osteochondritis dissecans (OD) of the knee represents a not uncommon challenge in the clinical routine. This is especially the case for physically active patients, players in mass sports and competitive athletes as the long recovery times associated with the treatment of OD are often not compatible with the heightened expectations of young athletes. In such cases, the treatment of OD is normally stage adjusted. This requires a temporally adapted and individual treatment concept. Despite the existing treatment guidelines, the decision for conservative or surgical treatment is not infrequently complicated by the limited diagnostic accuracy of the imaging procedures. As the current scientific literature on the ability of patients to resume sporting activities after OD and the influence of the strain of the sport on the short-term and long-term outcomes after OD treatment is low, further high-quality clinical studies are needed.

COSL Medical Directors' Hearing
25/01/2022
Link to the website LIROMS president Prof. Dr. Romain Seil was received by his Royal Highness the Grand Duke of Luxembourg. Photo © Maison du Grand-Duc / Kary Barthelmey

ReFORM webinar: Safesport 21/01/2022 - Luxembourg Academy of Sports Medicine, Physiotherapy & Science
23/01/2022
If you missed the webinar from January 21st, you will find it here : https://www.youtube.com/watch?v=dzrv8SmbLJA https://reform-sportscimed.org/webinaire-reform-sur-la-prevention-des-abus-dans-le-sport/?bmid=8d7bc0ffd9b3&source_from=invitation

Five years-results of a nationwide database on sudden cardiac events in sports practice in Luxembourg
19/01/2022
Link to the article Besenius E., Cabri J., Delagardelle C., Stammet P., Urhausen A. (2022). Five years-results of a nationwide database on sudden cardiac events in sports practice in Luxembourg. Dtsch Z Sportmed. 2022; 73: 24-29. doi:10.5960/dzsm.2021.505 The aim of this project was to create a national database to determine sports-related sudden cardiac event (SCE) burden in Luxembourg. Systematic data collection was carried out from 2015 until 2019 (5 years). Cases of SCE met the following criteria: (1) any major cardiac adverse event, (2) occurring during or until one hour after a sports activity (3) on national territory or outside Luxembourg by a Luxembourgish resident or sports license hol- der. The victim or family were contacted to inquire on the SCE by means of a standardized questionnaire. In total, 43 SCE cases were registered. The incidence was 2.6 cases/year/100000 physically active inhabitants. The 43 events occurred in 41 persons (40 males, 1 female), at an average age of 49.7 years. Seventeen events were fatal. The most concerned sports were cycling (17 cases), followed by football (5), and run- ning (4). Twenty-four victims suffered a sudden cardiac arrest, of which 16 received cardiopulmonary resuscitation (CPR). Eight (33%) of those survived. The survival rate was highest in patients receiving immediate CPR after SCE. The incidence of SCE related to sports in Luxembourg is rela- tively high and mainly affects middle-aged men during cycling. Bystander CPR significantly improves the chances of survival.

Exercise-Based Injury Prevention in High-Level and Professional Athletes: Narrative Review and Proposed Standard Operating Procedure for Future Lockdown-Like Contexts After COVID-19
05/01/2022
Link to the article Martens G, Delvaux F, Forthomme B, Kaux J-F, Urhausen A, Bieuzen F, Leclerc S, Winkler L, Brocherie F, Nedelec M, Morales-Artacho AJ, Ruffault A, Macquet A-C, Guilhem G, Hannouche D, Tscholl PM, Seil R, Edouard P and Croisier J-L (2021) Exercise-Based Injury Prevention in High-Level and Professional Athletes: Narrative Review and Proposed Standard Operating Procedure for Future Lockdown-Like Contexts After COVID-19. Front. Sports Act. Living 3:745765. doi: 10.3389/fspor.2021.745765 Sports injury prevention has become an essential field of sports medicine and science. It aims at reducing the impact of injuries on sports participation and improving long-term health (Engebretsen and Bahr, 2005). Implementing exercise- based prevention programs has been shown to be efficient in reducing the occurrence of injuries (Lauersen et al., 2014) but is still poorly applied on the field (Bahr et al., 2015). The major COVID-19 pandemic might have further compromised this implementation by drastically restricting daily life and physical activities. As most communities are preparing to live with the SARS-CoV-2 virus for a long haul, and since successive lockdown-like situations are likely to happen in the future either from this virus, other pandemics or other similar contexts, there is a need to anticipate and establish future recommendations to help exercise-based prevention program implementation in field contexts. The aim of this work was therefore two-fold: (1) to review the current literature on the impact of COVID-19 on sports participation and identify potential gaps in terms of injury prevention and (2) to provide Standard Operating Procedure to promote and conduct exercise-based injury prevention in high-level or professional athletes under lockdown-like contexts, based on both the available literature and the international sports medicine and science experiences.
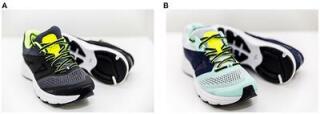
Relevance of Frequency-Domain Analyses to Relate Shoe Cushioning, Ground Impact Forces and Running Injury Risk: A Secondary Analysis of a Randomized Trial With 800+ Recreational Runners
11/11/2021
Link to the article Malisoux L, Gette P, Backes A, Delattre N, Cabri J and Theisen D (2021) Relevance of Frequency-Domain Analyses to Relate Shoe Cushioning, Ground Impact Forces and Running Injury Risk: A Secondary Analysis of a Randomized Trial With 800+ Recreational Runners. Front. Sports Act. Living 3:744658. doi: 10.3389/fspor.2021.744658 Running is characterized by the repetition of many, almost identical movements with limited variations (Mann et al., 2015). During the stance phase of each step, a ground reaction force (GRF) is applied to the body. The shape of the vertical component of the GRF over time is approximately that of a mass-spring impact (McMahon and Cheng, 1990). In most runners, two distinct peaks are easily detectable on a plot of the vertical GRF vs. time (Malisoux et al., 2021). The first peak (Fz1, often termed vertical impact peak force) occurs within the first 50 ms after initial contact and is referred to as the impact peak, while the second peak (Fz2) occurring approximately at mid stance phase is referred to as the active peak. Fz1 originates from the rapid deceleration of the support leg segments at initial contact, although the magnitude of the peak mainly depends on the contribution of the rest of the body. Fz2 is associated with the active motion of the rest of the body when the center of mass reaches its minimum vertical position during the stance phase (Bobbert et al., 1991). While Fz1 may not always be visually detectable in time-domain plots in runners with specific foot strike patterns (i.e., mid-and forefoot strike), (Lieberman et al., 2010), some studies provided evidence of a vertical impact force in all strike patterns (Gruber et al., 2011, 2017). The cumulative load applied to the musculoskeletal system resulting from several thousand steps taken during each training session may lead to an overuse injury, especially if inadequate recovery is provided between stress applications (Hreljac, 2004). For decades, it has been assumed that some running-related injuries are typically associated with the landing phase (e.g., stress fracture, tendinopathy), because of the stress resulting from the collision between the body and the ground (Cavanagh and Lafortune, 1980; Bobbert et al., 1991; Wit et al., 1995). The main arguments are that forces observed during distance running are 1.5–2 times larger than those occurring in walking, a rapid increase in force immediately follows initial contact, and a runner covering 20 km per week will cumulate more than 10,000 impacts on each leg over a seven-day period. During the landing phase, eccentric contractions are observed in some of the muscles controlling the movement (e.g., ankle-dorsiflexors or plantar flexors depending on the foot strike pattern, quadriceps muscles), which may cause large forces and high internal mechanical stress (Bobbert et al., 1991). Large muscular forces may also cause high stress on the tendons and their bony attachments. Consequently, biomechanical factors related to vertical GRF have often been studied during running, with Fz1, Fz2 and loading rate being among the most investigated variables. Surprisingly, the current knowledge on the relationship between impact force characteristics, such as Fz1 or vertical instantaneous loading rate, and injury risk is still inconsistent (Nigg et al., 2015; Theisen et al., 2016; Ceyssens et al., 2019). This is mainly due to small sample sizes, as well as differences in the populations investigated and study designs in research conducted so far (Nigg et al., 2015; Theisen et al., 2016; Ceyssens et al., 2019). Grimston et al. (1991) already observed a greater Fz1 in female runners with a history of stress fracture compared to non-stress-fracture runners, although the question whether these greater forces are a cause or a consequence of having suffered a stress fracture could not be addressed with such a study design. 25 years later, a meta-analysis confirmed that loading rate was higher in runners with a history of stress fracture (van der Worp et al., 2016). A similar effect was found from the studies that included runners with all running-related injury types compared with those without injuries. However, these conclusions are mostly based on case-control designs. A prospective study investigated impact forces as a potential injury risk factor in female runners, but no difference was observed between injured and uninjured runners (Davis et al., 2016). Secondary analyses showed that Fz1 and loading rates were greater in runners with a medically diagnosed injury compared to those who had never reported any previous injury. However, these results were based on a limited sample size (n = 32), the analysis was retrospective in nature, and running exposure (i.e., distance or hours of practice) was not taken into account, which severely limits the conclusions that can be drawn. Another plausible explanation for the inconsistent evidence could be that the relationship between impact forces and injury risk, if it exists, is not linear, but U-shaped. In this case, risk factors should not be analyzed as continuous variables, as in most previous studies, but instead be categorized using certain cutoffs (Bahr and Holme, 2003), thus transforming a continuous variable into a categorical or grouping variable. According to this method, runners with values in the upper or lower range of a given variable would be compared to a reference group, e.g., those with values within one standard deviation (SD) around the mean of the entire cohort. Despite the absence of prospective evidence on the role of impact force in injury development, it has been suggested that paradigms leading to a decrease or elimination of impact forces, such as changes in strike pattern (Lieberman et al., 2010; Cheung and Davis, 2011; Daoud et al., 2012) or increased shoe cushioning (Richards et al., 2009) would reduce injury risk. For instance, a 2-week gait retraining program aiming at lowering loading rate was effective in reducing injury risk in novice runners (Chan et al., 2018a). The protective effect of greater shoe cushioning has also been recently demonstrated in a randomized trial including 800+ recreational runners (Malisoux et al., 2020), where the participants having received the Soft shoe version had a lower injury risk compared to those having received the Hard version (Sub hazard rate ratio–SHR = 1.52; 95% Confidence Interval−95% CI = 1.07 to 2.16; Soft shoe group is the reference), (Malisoux and Theisen, 2020). In the same trial (Malisoux et al., 2020), all runners were tested in the allocated study shoes at baseline on an instrumented treadmill. One of the main findings was the greater Fz1 observed in the Soft shoe version (Malisoux et al., 2021). This may appear counterintuitive with regards to the initial goal of the cushioning systems (i.e., lower Fz1), but the observation was consistent with previous studies (Baltich et al., 2015; Chan et al., 2018b; Kulmala et al., 2018). An explanation for this “impact peak anomaly” has previously been provided (Shorten and Mientjes, 2011). The vertical GRF signal is actually a superimposition of low frequency (non-impact) and high-frequency (impact) load components (Shorten and Mientjes, 2011). In other words, the true impact force that originates from the collision of the lower leg segment with the ground is superimposed to the active force which depends primarily on the rest of the body (Bobbert et al., 1991). A previous study showed that softer shoes tend not only to attenuate the magnitude of the high-frequency impact peak, but also to delay its occurrence (Shorten and Mientjes, 2011). Consequently, the higher Fz1 observed in shoes with greater cushioning results from the greater relative contribution of the low-frequency load component to Fz1. Furthermore, Fz1 and loading rate were shown to be poorly correlated with tibial load bone metrics computed using a rigid body model (Matijevich et al., 2019), which suggests that Fz1 and loading rate may be unreliable indicators of musculoskeletal loading. Thus, the magnitude of Fz1 is not an appropriate indicator of impact intensity and running shoe impact alteration (Shorten and Mientjes, 2011; Matijevich et al., 2019; Malisoux et al., 2021). The main purpose of this study was to investigate whether the protective effect of the Soft shoe version observed previously (Malisoux et al., 2020) could be explained by an alteration of decomposed impact force characteristics using frequency-domain analyses. Therefore, the first objective of the study was to investigate the effect of shoe cushioning on the time, magnitude and frequency characteristics of peak forces using frequency-domain analyses by comparing baseline data from the two study groups (i.e., participants who received the Hard and Soft shoe version, respectively). We hypothesized that the Soft shoe version would be associated with a lower impact peak force, a delayed occurrence, and a lower vertical loading rate of the high-frequency signal (Shorten and Mientjes, 2011). Consistently, we also hypothesized that frequency of peak signal power, mean frequency, as well as power sum of the high frequency signal would be lower with the Soft shoe version. However, we did not expect any difference between the experimental groups in the magnitude and timing of the peak force of the low frequency signal. Our secondary objective was to investigate which of these force characteristics measured at baseline are prospectively associated with the risk of incurring a running-related injury. We hypothesized that a lower impact peak force, a delayed occurrence, and a lower vertical loading rate of the high-frequency signal would be associated with lower injury risk. We also expected that lower frequency of peak signal power, mean frequency, as well as power sum of the high frequency signal would be associated with lower injury risk.

Round table: Nutritional impact on injury preventions and immune system
02/11/2021
Video from the round table : Nutrional impact on injury preventions and immune system Speakers: T. Diderich, M. Jacobs, S. Rosquin (LIHPS, Luxembourg) Organised by the Luxembourgish Academy for Sports Medicine, Sports Physiotherapy and Sports Science

Training During the COVID‐19 Lockdown: Knowledge, Beliefs, and Practices of 12,526 Athletes from 142 Countries and Six Continents
26/10/2021
Link to the article LIROMS is proud to announce the publication of a major study co-authored by Prof. Axel Urhausen. Washif, J.A., Farooq, A., Krug, I. et al. Training During the COVID-19 Lockdown: Knowledge, Beliefs, and Practices of 12,526 Athletes from 142 Countries and Six Continents. Sports Med (2021). https://doi.org/10.1007/s40279-021-01573-z Objective Our objective was to explore the training-related knowledge, beliefs, and practices of athletes and the influence of lockdowns in response to the coronavirus disease 2019 (COVID-19) pandemic caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Methods Athletes (n = 12,526, comprising 13% world class, 21% international, 36% national, 24% state, and 6% recreational) completed an online survey that was available from 17 May to 5 July 2020 and explored their training behaviors (training knowledge, beliefs/attitudes, and practices), including specific questions on their training intensity, frequency, and session duration before and during lockdown (March–June 2020). Results Overall, 85% of athletes wanted to “maintain training,” and 79% disagreed with the statement that it is “okay to not train during lockdown,” with a greater prevalence for both in higher-level athletes. In total, 60% of athletes considered “coaching by correspondence (remote coaching)” to be sufficient (highest amongst world-class athletes). During lockdown, < 40% were able to maintain sport-specific training (e.g., long endurance [39%], interval training [35%], weightlifting [33%], plyometric exercise [30%]) at pre-lockdown levels (higher among world-class, international, and national athletes), with most (83%) training for “general fitness and health maintenance” during lockdown. Athletes trained alone (80%) and focused on bodyweight (65%) and cardiovascular (59%) exercise/training during lockdown. Compared with before lockdown, most athletes reported reduced training frequency (from between five and seven sessions per week to four or fewer), shorter training sessions (from ≥ 60 to < 60 min), and lower sport-specific intensity (~ 38% reduction), irrespective of athlete classification. Conclusions COVID-19-related lockdowns saw marked reductions in athletic training specificity, intensity, frequency, and duration, with notable within-sample differences (by athlete classification). Higher classification athletes had the strongest desire to “maintain” training and the greatest opposition to “not training” during lockdowns. These higher classification athletes retained training specificity to a greater degree than others, probably because of preferential access to limited training resources. More higher classification athletes considered “coaching by correspondence” as sufficient than did lower classification athletes. These lockdown-mediated changes in training were not conducive to maintenance or progression of athletes’ physical capacities and were also likely detrimental to athletes’ mental health. These data can be used by policy makers, athletes, and their multidisciplinary teams to modulate their practice, with a degree of individualization, in the current and continued pandemic-related scenario. Furthermore, the data may drive training-related educational resources for athletes and their multidisciplinary teams. Such upskilling would provide athletes with evidence to inform their training modifications in response to germane situations (e.g., COVID related, injury, and illness).

Sportmedica Congress 2021 - Welcome
18/10/2021
New methods in sports risk assessment and performance analysis - 16th October 2021 The International Sportmedica Congress will be organised in its 7th edition on 16th October 2021 by the Luxembourg Societies for Sports Medicine (SLMS) and Sports Physiotherapy (SLKS) together with the Luxembourg Academy of Sports Medicine, Physiotherapy and Science and its partners. The venue will be the "d'Coque" in Luxembourg. Previous editions covered a broad variety of topics: 1996 La force musculaire2000 L'évolution de l'entrainement du sportif2004 La pratique sportive chez l'enfant2008 Optimisation de l'activité physique2013 Sports Medicine and Science in Prevention and Rehabilitation: New Standards for Luxembourg2016 Wettkampfmedizin - Medicine in competition In 2021 the congress theme will be “New methods in sports risk assessment and performance analysis" featuring 5 international speakers. The aim is to organise a practice-oriented congress, the target audience being trainers, coaches, medical staff members, athletes, and scientists in the field. The different topics that will be treated are biomechanics, injury prevention, performance, anti-doping, and monitoring. The Sportmedica Congress will provide ample occasion to summarize existing knowledge and stimulate discussions between different stakeholders. The congress was postponed from 2020 to the 16th of October 2021 in an effort to organise a fruitful congress, all while respecting the necessary precautions due to the ongoing pandemic situation. The congress will thus be held as Covid-Check event, where the entry is reserved exclusively for people who have been vaccinated, recovered, or tested negative (either by means of an on-site self-test or by means of a certified negative result: PCR in the last 72h or antigen test in the last 48h). www.sportmedica.lu

Sportmedica Congress 2021 - Presentation Dr. Prof. Jan Cabri
18/10/2021
Innovative movement analysis - Jan Cabri, PhD, Prof - Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science www.sportmedica.lu

Sportmedica Congress 2021 - Presentation MD Detlef Thieme
18/10/2021
Innovative research in antidoping - Detlef Thieme, MD - Institute of Doping Analysis and Sports Biochemistry, Dresden, Germany www.sportmedica.lu

Sportmedica Congress 2021 - Presentation Dr. Prof. Bernd Grimm
18/10/2021
Wearable technology in sports and prevention – Bernd Grimm, PhD, Prof - Human Motion, Orthopaedics, Sports Medicine, Digital Methods @ Luxembourg Institute of Health www.sportmedica.lu

Sportmedica Congress 2021 - Presentation Dr. Prof. Christophe Ley
18/10/2021
The use of artificial intelligence in sports medicine - quo vadis? - Christophe Ley, PhD, Prof - Dept. Mathematics @ Université de Luxembourg www.sportmedica.lu

Sportmedica Congress 2021 - Presentation Dr. Prof. Caroline Nicol
18/10/2021
Running pattern dynamics in a simulated reduced gravity - Caroline Nicol, PhD, Prof - Institut des Sciences du Mouvement Etienne Jules Marey @ Aix-Marseille Université www.sportmedica.lu

Bulletin of the Luxembourg Society of Medical Sciences
12/10/2021
Link to the Bulletin Article from Prof. Dr med Axel URHAUSEN " Return to sport after Covid-19" page 35 to 38

Does prevention pay off? Economic aspects of sports injury prevention: a systematic review
01/10/2021
Link to the article Lutter C, Jacquet C, Verhagen E, Seil R, Tischer T. Does prevention pay off? Economic aspects of sports injury prevention: a systematic review. Br J Sports Med. 2021 Oct 1:bjsports-2021-104241. doi: 10.1136/bjsports-2021-104241. Objective: To identify, summarise and critically assess economic evaluation studies on sports injury prevention strategies. Design: Systematic review. Data sources: PubMed, SportDiscuss. Eligibility criteria for selecting studies: The current literature was searched following Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines. Economic analyses published since 2010 were checked for inclusion. The methodological quality of the studies was assessed using the Oxford Level of Evidence for economic and decision analysis; underlying randomised controlled trials (RCTs) were rated according to the Physiotherapy Evidence Database (PEDro) Scale, and risk of bias was assessed using the Revised Cochrane risk-of-bias tool. Results: Ten studies fulfilled the inclusion criteria. The quality assessment revealed limited data quality. For trial-based analysis, underlying RCTs were of good quality and had a low risk of bias. Prevention concepts for general injury reduction showed effectiveness and cost savings. Regarding specific injury types, the analysis of the studies showed that the best data are available for ankle, hamstring and anterior cruciate ligament injuries. Measures using specific training interventions were the predominant form of prevention concepts; studies investigating these concepts showed cost-effectiveness with total cost savings between €24.82 and €462 per athlete. Conclusion: Injury prevention strategies that were studied are cost-effective. However, estimates and outcomes vary throughout the included studies, and precluded pooling of existing data. Knowledge about the cost-effectiveness of evaluated prevention measures will help improve the acceptance and application of prevention initiatives.

Congratulations to our President Prof. Dr. Romain Seil who was awarded honorary member of the French Academy of Surgery
28/09/2021
Congratulations to our President Prof. Dr. Romain Seil who was awarded honorary member of the French Academy of Surgery by its President Prof. Henry Coudane from Nancy. The Academy has a long tradition and goes back to Louis the XIVth. Its goal is to display, recognize and promote excellence in surgery from France and related countries. It is a special honor to get this recognition for his clinical and scientific work from such a prestigious institution by one of Luxembourg’s big neighbour countries. This is of special value since such promotion of surgical science has no tradition in our small country.

VUB LUXEMBOURG CHAIR
19/09/2021
LIROMS is very proud of its partnership with the Vrije Univesiteit Brussel (VUB) to create the Luxembourg Chair for Translational Research in Human Motion, Sports Injury Prevention and Health. link

Developing, Implementing, and Applying Novel Techniques During Systematic Reviews of Primary Space Medicine Data
15/09/2021
Link to the article Winnard A, Caplan N, Bruce-Martin C, Swain P, Velho R, Meroni R, Wotring V, Damann V, Weber T, Evetts S, Laws J. Developing, Implementing, and Applying Novel Techniques During Systematic Reviews of Primary Space Medicine Data. Aerosp Med Hum Perform. 2021 Aug 1;92(8):681-688. doi: 10.3357/AMHP.5803.2021. PMID: 34503621. LIROMS supported a study aiming to identify new ways to review “space medicine” data done by the Aerospace Medicine and Rehabilitation Laboratory, Faculty of Health and Life Sciences, Northumbria University, Newcastle Upon Tyne, United Kingdom; the Department of Physiotherapy, LUNEX International University of Health, Differdange, Luxembourg; Human Performance in Space, International Space University, Strasbourg, France; the Space Medicine Team, ESA HRE-OM, European Astronaut Centre (EAC) and KBR GmbH, Cologne, Germany; and Blue Abyss, Liverpool, United Kingdom. Abstract BACKGROUND: The Aerospace Medicine Systematic Review Group was set up in 2016 to facilitate high quality and transparent synthesis of primary data to enable evidence-based practice. The group identified many research methods specific to space medicine that need consideration for systematic review methods. The group has developed space medicine specific methods to address this and trialed usage of these methods across seven published systematic reviews. This paper outlines evolution of space medicine synthesis methods and discussion of their initial application. METHODS: Space medicine systematic review guidance has been developed for protocol planning, quantitative and qualitative synthesis, sourcing gray data, and assessing quality and transferability of space medicine human spaceflight simulation study environments. RESULTS: Decision algorithms for guidance and tool usage were created based on usage. Six reviews used quantitative methods in which no meta-analyses were possible due to lack of controlled trials or reporting issues. All reviews scored the quality and transferability of space simulation environments. One review was qualitative. Several research gaps were identified. CONCLUSION: Successful use of the developed methods demonstrates usability and initial validity. The current space medicine evidence base resulting in no meta-analyses being possible shows the need for standardized guidance on how to synthesize data in this field. It also provides evidence to call for increasing use of controlled trials, standardizing outcome measures, and improving minimum reporting standards. Space medicine is a unique field of medical research that requires specific systematic review methods.

Are contralateral pelvic drop, knee valgus and foot overpronation clinically relevant signs in injured runners?
14/09/2021
Link to the presentation Amandine Bodson Biomechanics Master 2 - Université Claude Bernard Lyon 1Scientific Director: Prof Dr Jan Cabri (LIROMS)09-09-2021 Congratulations to Amandine Bodson who completed her Biomechanics Master's thesis. Amandine has performed an internship during 6 months at LIROMS. Background: The number of runners is increasing significantly each year and consequently also the number of overuse injuries. Previous research has demonstrated that kinematic parameters can be related to running injuries. Yet, we see three main kinematic parameters standing out from specific running related injuries: contralateral pelvic drop, knee valgus and foot overpronation. Objectives: To identify whether the three aforementioned kinematic variables are clinically relevant signs of possible structural injury. Secondly, to verify if differences in the kinematics between injured and non-injured legs are prevalent. Finally, to see if there is a correlation between the injury location and the three aforementioned kinematic parameters in the injured legs of runners tested.Design: Retrospective study Methods: Biomechanical treadmill running analyses were conducted on 50 injured and 13 non-injured runners using a 3-dimensional motion capture system (9 cameras Miqus System, Qualisys AB, Gothenburg, Sweden). Seven kinematic variables during the gait stance phase were compared between injured and healthy runners while controlling for speed. To eliminate redundancy and increase the power of our statistical model only three variables remained relevant: peak hip adduction angle, peak knee adduction angle and peak rearfoot eversion angle. Results: Results of the MANCOVA revealed no significant differences between the injured and non-injured runners' groups (p=0.164) for the variables controlling contralateral pelvic drop, knee valgus and foot overpronation with speed as covariate. However, significant differences between male and female participants for peak hip adduction (p=0.006) was found. Women demonstrate more hip adduction than men (mean=16.9°; SD 3.8 and 14°; SD 4.0 respectively). This difference can be explained by a larger pelvis width to femur length ratio in women than in men. In addition, running speed influenced several kinematic variables, i.e. peak hip adduction (p=0.002) and peak rearfoot eversion (p<0.001). A slower running speed was associated with reduced angle in peak hip adduction and peak rearfoot eversion The results of the paired sample T-test revealed that the injured and non-injured legs in the injured running population showed no significant differences with peak hip adduction (p=0.372), peak knee adduction (p=0.343) and peak rearfoot eversion (p=0.804) angles at mid-stance. As for the multiple logistic regression analysis, the relationship between the set of variables and injury location showed no significant relationship for foot (R2=0.043; p=0.535), lower leg (R2=0.190; p=0.017, knee (R2=0.038; p=0.465), or hip (R2=0.149; p=0.109). Conclusion: Contralateral pelvic drop, knee valgus and foot overpronation kinematic parameters are influenced by the population, running speed and injury location. For future research, a subclassification of the kinematic representation of each RRI could help clinician in their clinical reasoning process when evaluating runners and could target the intervention strategy development.
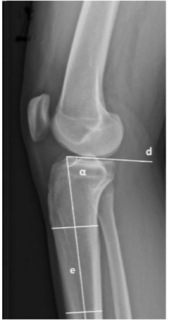
Side‐to‐side anterior tibial translation on monopodal weightbearing radiographs as a sign of knee decompensation in ACL‐deficient knees
31/08/2021
Link to the article Macchiarola L., Jacquet C., Dor J., Zaffagnini S., Mouton C., Seil R. Side-to-side anterior tibial translation on monopodal weightbearing radiographs as a sign of knee decompensation in ACL-deficient knees. Knee Surg Sports Traumatol Arthrosc. 2021 Aug 30. doi: 10.1007/s00167-021-06719-0. Epub ahead of print. PMID: 34459934. Abstract Purpose: To evaluate the influence of time from injury and meniscus tears on the side-to-side difference in anterior tibial translation (SSD-ATT) as measured on lateral monopodal weightbearing radiographs in both primary and secondary ACL deficiencies. Methods: Data from 69 patients (43 males/26 females, median age 27-percentile 25-75: 20-37), were retrospectively extracted from their medical records. All had a primary or secondary ACL deficiency as confirmed by MRI and clinical examination, with a bilateral weightbearing radiograph of the knees at 15°-20° flexion available. Meniscal status was assessed on MRI images by a radiologist and an independent orthopaedic surgeon. ATT and posterior tibial slope (PTS) were measured on the lateral monopodal weightbearing radiographs for both the affected and the contralateral healthy side. A paired t-test was used to compare affected/healthy knees. Independent t-tests were used to compare primary/secondary ACL deficiencies, time from injury (TFI) (≤ 4 years/ > 4 years) and meniscal versus no meniscal tear. Results: ATT of the affected side was significantly greater than the contralateral side (6.2 ± 4.4 mm vs 3.5 ± 2.8 mm; p < 0.01). There was moderate correlation between ATT and PTS in both the affected and healthy knees (r = 0.43, p < 0.01 and r = 0.41, p < 0.01). SSD-ATT was greater in secondary ACL deficiencies (4.7 ± 3.8 vs 1.9 ± 3.2 mm; p < 0.01), patients with a TFI greater than 4 years (4.2 ± 3.8 vs 2.0 ± 3.0 mm; p < 0.01) and with at least one meniscal tear (3.9 ± 3.8 vs 0.7 ± 2.2 mm; p < 0.01). Linear regression showed that, in primary ACL deficiencies, SSD-ATT was expected to increase (+ 2.7 mm) only if both a meniscal tear and a TFI > 4 years were present. In secondary ACL deficiencies, SSD-ATT was mainly influenced by the presence of meniscal tears regardless of the TFI. Conclusion: SSD-ATT was significantly greater in secondary ACL deficiencies, patients with a TFI greater than 4 years and with at least one meniscal tear. These results confirm that SSD-ATT is a time- and meniscal-dependent parameter, supporting the concept of gradual sagittal decompensation in ACL-deficient knees, and point out the importance of the menisci as secondary restraints of the anterior knee laxity. Monopodal weightbearing radiographs may offer an easy and objective method for the follow-up of ACL-injured patients to identify early signs of soft tissue decompensation under loading conditions.
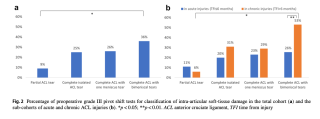
Grade III pivot shift as an early sign of knee decompensation in chronic ACL‐injured knees with bimeniscal tears
25/08/2021
Link to the article Magosch A, Jacquet C, Nührenbörger C, Mouton C, Seil R. Grade III pivot shift as an early sign of knee decompensation in chronic ACL-injured knees with bimeniscal tears. Knee Surg Sports Traumatol Arthrosc. 2021 Jul 23. doi: 10.1007/s00167-021-06673-x. Epub ahead of print. PMID: 34302192. Abstract Purpose: To analyse possible associations between the preoperative pivot shift (PS) test and both patient and injury characteristics in anterior cruciate ligament (ACL)-injured knees, considering previously neglected meniscal injuries such as ramp and root tears. The hypothesis was that a preoperative grade III PS was associated with the amount of intra-articular soft-tissue damage and chronicity of the injury. Methods: The cohort involved 376 patients who underwent primary ACL reconstruction (239 males/137 females; median age 26). Patients were examined under anesthesia before surgery, using the PS test. During arthroscopy, intra-articular soft-tissue damage of the injured knee was classified as: (1) partial ACL tear; (2) complete isolated ACL tear; (3) complete ACL tear with one meniscus tear; and (4) complete ACL and bimeniscal tears. Chi-square and Mann-Whitney U tests were used to evaluate whether sex, age, body mass index, sport at injury, mechanism of injury, time from injury and intra-articular damage (structural damage of ACL and menisci) were associated with a grade III PS. Intra-articular damage was further analyzed for two sub-cohorts: acute (time from injury ≤ 6 months) and chronic injuries (> 6 months). Results: A grade III PS test was observed in 26% of patients. A significant association with PS grading was shown for age, time from injury and intra-articular soft-tissue damage (p < 0.05). Further analyses showed that grade III PS was associated with intra-articular damage in chronic injuries only (p < 0.01). In complete ACL and bimeniscal tears, grade III PS was more frequent in chronic (53%) than in acute knee injuries (26%; p < 0.01). Patients with chronic complete ACL and bimeniscal tears had a grade III PS 3.3 [1.3-8.2] times more often than patients in the acute sub-cohort. Conclusion: In ACL-injured patients, a preoperative grade III PS was mainly associated with a higher amount of intra-articular soft-tissue damage and chronicity of the injury. Patients with complete chronic ACL injuries and bimeniscal tears were more likely to have a preoperative grade III PS than their acute counterparts. This suggests that grade III PS may be an early sign of knee decompensation of dynamic rotational knee laxity in chronic ACL-injured knees with bimeniscal lesions.
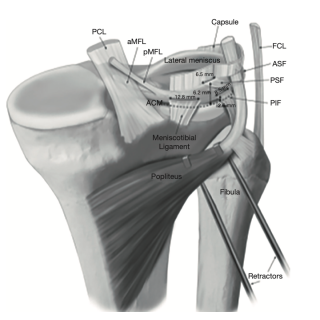
The hypermobile and unstable lateral meniscus: a narrative review of the anatomy, biomechanics, diagnosis and treatment options
25/08/2021
Link to the article Beel W, Macchiarola L, Mouton C, Laver L, Seil R. The hypermobile and unstable lateral meniscus: a narrative review of the anatomy, biomechanics, diagnosis and treatment options. Ann Joint 2021. https://dx.doi.org/10.21037/aoj-21-9 Objective: The purpose of this review is to improve the awareness of lateral meniscal hypermobility by describing its relevant anatomy, biomechanics, pathophysiology, imaging and arthroscopic findings as well as the treatment options. Background: The lateral meniscus is less stable than the medial meniscus. Its important posterior stabilizers are the popliteomeniscal fascicles, the posterior capsule, the meniscofemoral ligaments and the posterior meniscotibial ligament, which are divided by a bare area, the popliteal hiatus. Atraumatic insufficiency or rupture of one of these key structures may impact the mobility of the lateral meniscus and can lead to an unstable, hypermobile lateral meniscus. Lateral meniscus hypermobility can cause lateral knee pain and mechanical symptoms as locking. Ruptures of the popliteomeniscal fascicles are frequently associated with anterior cruciate ligament and posterolateral corner injuries. Their repair may be important to fully restore knee stability. Methods: This is a narrative overview of the literature synthesizing current knowledge about the hypermobile lateral meniscus. Anatomy, biomechanics, diagnosis and treatment of this entity was of particular interest for this review. Literature was retrieved from PubMed database, hand searches and cross-reference checking. Conclusions: Diagnosing lateral meniscus hypermobility is challenging since the magnetic resonance imaging are often unspecific and may show no structural alterations of the meniscus and its attachments. The only hint can be the patient’s history and clinical symptoms (e.g., locking). Ultimately, the diagnosis is confirmed during knee arthroscopy, when the lateral meniscus can be mobilized over 50% of the lateral tibial plateau or lateral femoral condyle while anterior probing or by using the aspiration function during arthroscopy. Treatment includes stabilizing the posterior lateral meniscus by repairing the injured structures. Therefore, a systematic arthroscopic evaluation of the lateral compartment is important to fully recognize the problem. Repair can be achieved arthroscopically with various suturing techniques used for meniscal repair with satisfactory results and low recurrence rates.

Technical note: rectangular femoral tunnel for anterior cruciate ligament reconstruction using a new ultrasonic device: a feasibility study
25/08/2021
Link to the article Seil R., Mouton C., Jacquet C. Technical note: rectangular femoral tunnel for anterior cruciate ligament reconstruction using a new ultrasonic device: a feasibility study. J Exp Orthop. 2021 Jul 22;8(1):53. doi: 10.1186/s40634-021-00373-8. PMID: 34296367; PMCID: PMC8298747. Abstract Purpose: The goal of this preliminary report was to show the use of novel Ultrasound (US) technology for anterior cruciate ligament (ACL) reconstruction surgery and evaluate its feasibility for the creation of a rectangular femoral bone tunnel during an arthroscopic procedure in a human cadaver model. Methods: Two fresh frozen human cadaver knees were prepared for arthroscopic rectangular femoral tunnel completion using a prototype US device (OLYMPUS EUROPA SE & CO. KG). The desired rectangular femoral tunnel was intended to be located in the femoral anatomical ACL footprint. Its tunnel aperture was planned at 10 × 5 mm and a depth of 20 mm should be achieved. For one knee, the rectangular femoral tunnel was realized without a specific cutting guide and for the other with a 10 × 5 mm guide. One experienced orthopedic surgeon performed the two procedures consecutively. The time for femoral tunnel completion was evaluated. CT scans with subsequent three-dimensional image reconstructions were performed in order to evaluate tunnel placement and configuration. Results: In the two human cadaver models the two 10 × 5x20mm rectangular femoral tunnels were successfully completed and located in the femoral anatomical ACL footprint without adverse events. The time for femoral tunnel completion was 14 min 35 s for the procedure without the guide and 4 min 20 s with the guide. Conclusion: US technology can be used for the creation of a rectangular femoral bone tunnel during an arthroscopic ACL reconstruction procedure. The use of a specific cutting guide can reduce the time for femoral tunnel completion. Additional experience will further reduce the time of the procedure.
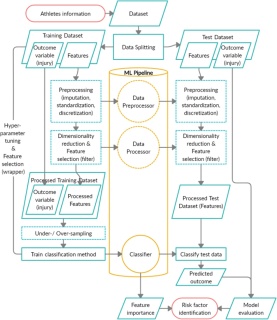
Machine learning methods in sport injury prediction and prevention: a systematic review
18/08/2021
Link to the article Van Eetvelde, H., Mendonça, L.D., Ley, C., Seil R. and Tischer T. Machine learning methods in sport injury prediction and prevention: a systematic review. J EXP ORTOP 8, 27 (2021). https://doi.org/10.1186/s40634-021-00346-x The most downloaded JEO Journal article from July was an overview article on machine learning methods in athlete injury prediction and prevention.Read this interesting article on the fast-developing capabilities of machine learning in orthopaedics.
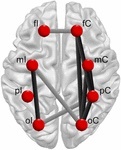
Functional Cortical Connectivity Related to Postural Control in Patients Six Weeks After Anterior Cruciate Ligament Reconstruction
21/07/2021
Link to the article Lehmann T., Büchel D., Mouton C., Gokeler A., Seil R. and Baumeister J. (2021) Functional Cortical Connectivity Related to Postural Control in Patients Six Weeks After Anterior Cruciate Ligament Reconstruction. Front. Hum. Neurosci.15:655116. doi: 10.3389/fnhum.2021.655116 Introduction Injuries to the anterior cruciate ligament (ACL) substantially affect knee joint laxity and cause long-term consequences for injured athletes. The accompanying functional impairments of an ACL tear thereby appear to extend beyond biomechanical alterations, comprising a loss of mechanoreceptors which consequently lead to diminished afferent input to higher levels of the sensorimotor system (Courtney et al., 2005; Kapreli et al., 2009). Although ACL injuries have repeatedly been shown to cause deficits in knee function even after surgical anterior cruciate ligament reconstruction (ACLR), knowledge about associated mechanisms of the sensorimotor system for compensating these functional impairments is still lacking (Ageberg, 2002). A growing amount of evidence has begun identifying clinically meaningful neuroplastic changes in the sensorimotor system following ACL injury. Investigations utilizing transcranial magnetic stimulation, for instance, have detected enhanced motor thresholds in the ACL injured limb, whereas functional magnetic resonance imaging or electroencephalography (EEG) studies observed increased activations of the motor areas and lower activations of somatosensory areas in these patients (Neto et al., 2019). Along with altered somatosensory information from the ACL, decreased innervation to the primary sensory cortex (Valeriani et al., 1999), as well as different corticospinal and motor cortex excitability (Pietrosimone et al., 2015; Grooms et al., 2017; Lepley et al., 2020) have been observed in patients after ACL reconstruction. As a consequence of increased motor thresholds of the injured limb and decreased responsiveness of motor areas, greater cortico-cortical stimulation is required to evoke efferent neural signaling in the motor cortex for properly controlling motion and stability of the knee joint (Lepley et al., 2020). Thus, patients with ACL injury have been shown to recruit motor areas to a larger extent than healthy individuals, indicating that cortical adaptations may facilitate the restoration of lower limb motor functions by driving compensatory synergistic muscle patterns (Courtney et al., 2005). Whereas initial findings have identified compensatory cortical patterns in patients after ACLR during proprioceptive tasks (Baumeister et al., 2008, 2011), little is known about the cortical mechanisms behind the postural deficiencies in this population. After ACLR and the following rehabilitation, many patients exhibit significantly decreased static postural stability as implied by increased center of pressure (CoP) excursions and velocities while standing on their injured limb (Lehmann et al., 2017). Although comprehensive evidence in the early postsurgical period is missing, postural stability in patients after ACLR was reported to deviate from both the preoperative level (Gokalp et al., 2016) and healthy controls (Parus et al., 2015) after the 4th and 8th week of surgery. With respect to these functional deficiencies in patients after ACLR, postural control reflects multimodal interactions within the sensorimotor system (Shumway-Cook and Woollacott, 2012). Recent findings from neuroimaging studies suggested that active contributions from the cortex continuously maintain and restore postural equilibrium (Wittenberg et al., 2017). Collectively, these EEG investigations demonstrated variations in power spectral density of theta (4–7 Hz), alpha-1 (8–10 Hz), and alpha-2 (10–12 Hz) frequency oscillations in frontal, motor, parietal, and occipital regions of the cortex. While it is suggested that theta band oscillations reflect a general brain integrative mechanism related to short term storage and manipulation of multimodal information for a given operation, alpha oscillations are related to the active inhibition of non-essential neuronal processing (Cheron et al., 2016), with alpha-1 reflecting global alertness of cortical areas and alpha-2 being associated with task-specific sensorimotor processing (Pfurtscheller and Lopes, 1999). Modulations of oscillatory activity during postural tasks therefore conceivably reflect direct or indirect interactions within complex transcortical and cortico-subcortical loops for detecting and counteracting postural instability (Wittenberg et al., 2017). The underlying functional relationships, as quantified by statistical interdependencies among distributed cortical regions, are referred to as functional connectivity (Friston, 2011). These connections show frequency-specific modulations within a fronto-parietal theta network and a parieto-occipital alpha network in response to postural instability and varying postural demands (Mierau et al., 2017; Varghese et al., 2019; Lehmann et al., 2020). In the light of injury-related increased postural sway (Lehmann et al., 2017), patients after ACLR may require stronger interactions of functionally interconnected sensorimotor areas for properly controlling postural stability (Rosen et al., 2019; Jiganti et al., 2020), as well as hip and knee movement (Criss et al., 2020) while standing on the injured limb. Investigations of structural white matter changes following ACLR further indicated that the hemisphere contralateral to the injured leg may be particularly affected by this neurostructural reorganization (Lepley et al., 2020). Therefore, the aim of the present case-control study is to explore leg dependent patterns of cortical connectivity related to postural control during single leg stances in patients 6 weeks following ACLR. It is hypothesized that patients after ACLR may show compensatory cortical mechanisms in terms of stronger functional connections within the theta and alpha networks compared to their matched controls. Furthermore, these cortical adaptations may specifically affect the stance on the injured limb. In this way, the current investigation may gain further insight into sensorimotor changes related to postural deficiencies after ACLR.

First Aggregation in Physiotherapy at the University of Porto
21/07/2021
Prof. Dr Jan CABRI was part of the jury for the aggregation exam in Physiotherapy at the FADEUP (Faculty of Sport of the University of Porto). The curricular unit report is entitled “Clinical Exercise: Emerging Trends and Research Approaches” and the theme of the lesson/seminar is “Physical Exercise as a Non-Pharmacological Treatment of Arterial Hypertension”.”
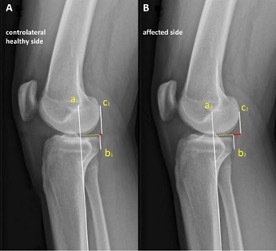
Presentation from Dr. Luca Macchiarola (MD - Orthopaedic Surgeon)
20/07/2021
Side-To-Side Anterior Tibial Translation on Monopodal Weightbearing Radiographs as a Sign of Knee Decompensation in ACL Deficient Knees Dr. Luca MACCHIAROLA (presenter), Dr. Christophe JACQUET, Dr Jeremie DOR, Prof. Stefano ZAFFAGNINI, Caroline MOUTON, Dr. Prof. Romain SEIL CHL EICH / LIROMS

Chief Scientific Expert nomination
14/07/2021
Congratulations! to Prof. Dr. Jan CABRI who has been appointed Chief Scientific Expert for the Luxembourg Institute for High Performance in Sports (LIHPS). https://lihps.lu/who-we-are/team/

Mental Fatigue and Sport‐Specific Psychomotor Performance: A Systematic Review
06/07/2021
Link to article Habay, J., Van Cutsem, J., Verschueren, J., De Bock, S., Proost, M., De Wachter, J., Tassignon, B., Meeusen, R., & Roelands, B. (2021). Mental Fatigue and Sport-Specific Psychomotor Performance: A Systematic Review. Sports medicine (Auckland, N.Z.), 51(7), 1527–1548. https://doi.org/10.1007/s40279-021-01429-6 Abstract Background Mental fatigue (MF) is a psychobiological state that impairs endurance performance in healthy athletes. Recently, multiple studies indicated that MF could also impair sport-specific psychomotor performance (SSPP). Neverthe- less, a systematic overview detailing the effects of MF on SSPP is currently lacking.Objective The objective of this study is to collate relevant literature and examine the effect of MF on SSPP. A secondary aim was to create an overview of the potential subjective and physiological factors underlying this MF effect. Methods PubMed (MEDLINE), Web of Science, PsycINFO and SPORTDiscus were searched (5th of November 2020). Studies were eligible when study outcomes encompassed any form of SSPP skill in a sport-specific context, the intervention was targeted to induce MF, and the population included healthy individuals. The presence of a manipulation check, to indicate the successful induction of MF, was obligatory for inclusion. Secondary outcomes were all outcomes (either physiological or psychological) that could explain the underlying mechanisms of the effect of MF on SSPP. Results In total, 21 papers were included. MF was successfully induced in all but two studies, which were excluded from further analysis. MF negatively impacts a myriad of SSPP outcomes, including decision-making, reaction time and accuracy outcomes. No changes in physiological outcomes, that could underlie the effect of MF, were reported. Subjectively, only ratings of perceived of exertion increased due to MF in some studies. Conclusions Overall, the selected papers indicated that MF negatively affects SSPP. Research that assesses brain function, while evaluating the effect of MF on SSPP is essential to create further insight.

Anti-Doping: New e-learning course for medical professionals
01/07/2021
Link to the article Anti-Doping: New e-learning course for medical professionals Prof. Dr. med. Axel URHAUSEN is a member of the NADA Medicine Group, which participated to this project. The National Anti Doping Agency of Germany, NADA, a civil law foundation by form, is the key body for clean sports in Germany. NADA has become the center of competence for anti-doping activities in Germany. NADA’s tasks are diverse and cover doping controls, education and prevention, medical and legal advice as well as international cooperation. Thereby, NADA Germany significantly contributes to the preservation of values in sports. NADA tackles the problem of doping in sports, cooperatively, on the national and international level, and supports all athletes who compete clean. A comprehensive e-learning course designed by the World Anti-Doping Agency (WADA) and translated by the National Anti-Doping Agency (NADA) is available for athletes' medical personnel. It can be accessed under the title "ADEL for medical professionals" on WADA's Anti-Doping Education and Learning (ADEL) website: adel.wada-ama.org/learn/public/learning_plan/view/36/adel-fur-medizinisches-fachpersonal-german The course begins by addressing ethical and moral aspects that physicians are confronted with in the care of athletes. The course then focuses on practical case studies, which are used to explain the anti-doping regulations that are important for physicians, the World Anti-Doping Code and the National Anti-Doping Code, the Prohibited List and the Standard for Therapeutic Use Exemptions. In addition, it will be made clear how physicians can support the athletes under their care in complying with the anti-doping regulations. To this end, the course presents the basics of doping prevention and the doping control system as well as legal aspects. Each of the four thematic modules concludes with a review of the knowledge acquired. At the end of the entire course, participants can expect a final examination. If they pass, the participants receive a corresponding certificate.
Does practice of meniscus surgery change over time?
28/06/2021
Link to the article Jacquet, C., Mouton, C., Becker, R., Koga H., Ollivier M., Verdonk P., Beaufils P., Seil R. Does practice of meniscus surgery change over time? A report of the 2021 ‘THE MENISCUS’ Webinar. J EXP ORTOP 8, 46 (2021). https://doi.org/10.1186/s40634-021-00365-8 Purpose. The aim of this paper was to report the results presented in the session “Does practice of meniscus surgery change over time?” of the 2021 MENISCUS webinar held online on January 30th 2021. Method. During the 2021 MENISCUS webinar, an evaluation of meniscus surgery practices was performed by analyzing: (1) The presentation of the results of a survey conducted among ESSKA members and assessing their current practices in the field of meniscus surgery, (2) Four reports by national experts analyzing the trends in Arthroscopic Partial Meniscectomy (APM) and meniscus repair procedures in their respective countries (France, Belgium, Germany and Japan). Results. (1) ESSKA Survey: Among the 461 respondents, 75% of surgeons claimed to perform more meniscus repairs and 85% less APM than 5 years ago. In ACL-associated meniscus injuries, a majority of surgeons (60%) indicated to perform a meniscal resection in less than 25% of cases. 25% declared to perform meniscus repair in ACL-associated meniscus injuries in less than 25% of cases and 37% in more than 50% of cases. Half of the respondents repair medial or lateral root tears in less than 25% of cases. Less than 20% of respondents were not familiar with the ESSKA consensus. (2) National trends: In France, between 2005 and 2017, the APM rate decreased by 21.4%, while the repair rate increased by 320%. In Belgium, between 2007 and 2017, the APM rate decreased by 28.6%. In Germany, between 2010 and 2017 the number of APM decreased by 30%, while the number of repair procedures increased by 55%. Finally, in Japan, between 2011 and 2016, the APM ratio (APM/meniscus procedures) decreased by 16% from 91 to 75% while the repair ratio increased from 9 to 25%. Conclusion. The 2021 ESSKA members' survey as well as statistics from 4 specifically examined countries (Belgium, France, Germany and Japan) suggest there has been a significant shift over the last years in the surgical management of meniscal lesions towards less APM and more conservative treatments.

Preliminary experience of an international orthopaedic registry: the ESSKA Paediatric Anterior Cruciate Ligament Initiative (PAMI) registry
28/06/2021
Link to the article Mouton, C., Moksnes, H., Janssen, R., Fink C., Zaffagnini S., Monllau JC., Ekås G., Engebretsen L., Seil R. Preliminary experience of an international orthopaedic registry: the ESSKA Paediatric Anterior Cruciate Ligament Initiative (PAMI) registry. J EXP ORTOP 8, 45 (2021). https://doi.org/10.1186/s40634-021-00366-7 Abstract Paediatric and adolescent ACL injuries are an emerging health burden, increasing at a higher rate than in adults. They compromise quality of life, affect knee structure and function, lead to the early development of osteoarthritis and are a serious economic burden due to shortened professional careers and subsequent surgeries. Up to 35% of children and adolescents will experience a second ACL injury and this population particularly at high risk of secondary intraarticular soft tissue degeneration and growth abnormalities. However, there is still a lack of high-quality outcome studies on this specific population and many knowledge gaps persist in the current treatment guidelines. It is currently unknown whether ACL reconstruction in this young population decreases the risk of irreversible secondary intraarticular soft tissue degeneration. Furthermore, it is not known whether return to high or elite level sports after paediatric ACL injury or reconstruction should be recommended. The relatively low number of paediatric ACL injuries seen in each hospital makes it necessary to conduct international multi-centre studies to collect robust data to provide evidence-based guidelines for the treatment of these injuries. The Paediatric Anterior Cruciate Ligament Initiative (PAMI) was thus started by the European Society of Sports Traumatology, Knee Surgery & Arthroscopy and opened for patient inclusion in 2018. This comprehensive overview of the first 2 years of the PAMI registry shows that the project is now well consolidated and accepted by the European orthopaedic community. Future challenges include ensuring additional external funding to ascertain long term sustainability and continuous dissemination of the knowledge acquired in scientific journals.

Return to sports after COVID-19 infection
16/06/2021
Video from the webinar held 16th June. Speakers: Dr S. Hein, Prof A. Urhausen, MD, PhD (CHL, Luxembourg) Organised by the Luxembourgish Academy for Sports Medicine, Sports Physiotherapy and Sports Science

Knee Arthroscopy: An Up-to-Date guide - Ramp lesions
14/06/2021
Link to the book Ramp lesions chapter. Seil R., Mouton C. Knee Arthroscopy: An Up-to-date guide - © Springer Nature Singapore Pte Ltd. 2021J. G. Kim (ed.), Knee Arthroscopy, https://doi.org/10.1007/978-981-15-8191-5_18 eBook ISBN978-981-15-8191-5 Hardcover ISBN978-981-15-8190-8 This book provides detailed guidance on knee arthroscopy that reflects the very latest advances in this ever-changing field. Among the techniques covered are reconstruction of the anterior and posterior cruciate ligaments, meniscal repair and transplantation, cartilage repair by means of osteochondral allograft transplantation and autogenous osteochondral transfer, medial patellofemoral ligament reconstruction, and high tibial osteotomy. In each case, clear descriptions of technique are supported by a wealth of high-quality illustrations, with identification of potential pitfalls and how to avoid them. In addition, the latest knowledge is presented on anatomy and biomechanics. The book is written by recognized experts in sports injuries and knee disorders. It will serve as an up-to-date reference for the experienced knee surgeon and an ideal source of information for all who wish to broaden their knowledge of and improve their skills in knee arthroscopy, whether general orthopaedists, orthopaedic trainees, or sports medicine physicians. Ramp lesions chapter (Seil R., Mouton C.) Ramp lesions to the posterior horn of the medial meniscus have recently received increased attention due to their high preva- lence in patients undergoing an anterior cru- ciate ligament reconstruction. The diagnosis of these lesions is rarely possible with preop- erative imaging and quite limited with routine anterior arthroscopic inspection of the knee joint. Visual inspection of the posteromedial compartment of the knee joint should thus systematically be carried out via a trans-notch view and meniscocapsular structures directly probed with a needle or visualized via a pos- teromedial portal. While the clinical impact of ramp lesions is not yet well established, recent biomechanical studies have shown increased anteroposterior and rotational laxi- ties when a ramp lesion is present. The latter may thus be a cause for postoperative persis- tent laxity potentially leading to the failure of ACL reconstructions. To date, it remains unclear whether all ramp lesions should be repaired as only a few publications report long-term outcomes after ramp lesion repair. This article provides an overview of the cur- rent knowledge on ramp lesions including their diagnosis, classification, biomechanical relevance as well as treatment and outcomes.

Specific Sports Related Injuries - Handball
14/06/2021
Link to the book Handball chapter - Landreau P., Laver L., Seil R., Popovic N. © ISAKOS 2021 S. Rocha Piedade et al. (eds.), Specific Sports-Related Injuries, https://doi.org/10.1007/978-3-030-66321-6_681 eBook ISBN978-3-030-66321-6 Hardcover ISBN978-3-030-66320-9 This book offers an overview of injury prevention and management for all most popular individual and team sports disciplines. Handball chapter (Landreau P., Laver L., Seil R., Popovic N.) Handball is one of the Olympic sports with the highest risk of injuries (13–17% of all athletes in Beijing, London, and Rio). In the 2012 Olympics, handball had the fourth highest injury score (22%) after taekwondo (39%), football (35%), and BMX (31%) and was ahead of other team sports like basketball (11%) and volleyball (6.9%). For some it would even be the highest risk ball sport. The risk of injuries is usually represented by the number of injuries occurring during a training or competitive match reported per 1000 exposure hours. The results in the literature are variable probably because some report only lesions caus- ing time-loss and others also include overuse.

Paperjam article - Medtech - 'CHL knee arthroscopy simulator receives €500,000'
09/06/2021
Link to the article Title: 'Le simulateur d’arthroscopie du genou du CHL reçoit 500.000 euros' published in Paperjam on June 8th, 2021 How can surgeons be prepared for a meniscus operation? With a simulator, developed by the Swiss start-up Virtamed, for Professor Romain Seil of the Centre Hospitalier de Luxembourg. With the help of a young Luxembourger, Claude Hoeltgen, the project has just received a grant of 500,000 euros.

High Incidence of Anterior Cruciate Ligament Injuries Within the First 2 Months of the Season in Amateur Team Ball Sports
08/06/2021
Link to the article Mouton, C., Gokeler, A., Urhausen, A., Nührenbörger, C., & Seil, R. (2021). High Incidence of Anterior Cruciate Ligament Injuries Within the First 2 Months of the Season in Amateur Team Ball Sports. Sports health, 19417381211014140. Advance online publication. https://doi.org/10.1177/19417381211014140 Background: The incidence of anterior cruciate ligament (ACL) injuries is commonly reported as an annual incidence rate. There is relatively little information about the seasonal aspects of these injuries. The aim of the current study was to analyze the distribution of ACL injuries during the season in nonprofessional soccer, handball, and basketball based on a retrospective analysis of a hospital-based registry.

Journée Kiné 2021 - Webinar June 2nd : Videos are now available!
03/06/2021
Videos from the Webinar June 2nd 2021. ACL CLINICAL PATHWAY: TRANSLATED EVIDENCE INTO CLINICAL PRACTICE Modérateurs: Romain SEIL, Prof. Dr. med, CHL. Danièle SCHAACK, PT; CHL. Topics presented: 1. Introduction - Jean-Paul Weydert 2. New developments in the management of severe knee injuries - Romain Seil, Prof. Dr. med 3. ACL clinical pathway - the CHL sports clinic model - Caroline Mouton, PhD 4. The importance of pre-habilitation of the injured athlete and the immediate post-operative care (Part 1) - Anne Frisch, PT, PhD 5. The importance of pre-habilitation of the injured athlete and the immediate post-operative care (Part 2) - Lisa Kirsch, PT 6. From the crutches back to functional activities - Louis Wennig 7. The return to training and performance (Part 1) - Nina Goedert PT 8. The return to training and performance (Part 2) - Jérôme Pauls, PT

Prevention of sports injuries in childhood and adolescence
26/05/2021
Link to the article. Nührenbörger C., Mouton C., Engelhardt M. Sports Orthop. Traumatol. 37, 10–17 (2021) Prävention von Sportverletzungen im Kindes- und Jugendalter. https://doi.org/10.1016/j.orthtr.2021.01.005 Sport in childhood and adolescence has many positive effects on a physical, psychological and social level as well as negative consequences such as sport injuries. There is a clear increase in acute and overuse injuries, with some serious long-term consequences on later life. In order to minimize the risk of injury, various preventive measures such as special exercise programs, age-appropriate training and competition loads, protective equipment, preventive sports medical examinations and competition support as well as rule changes have been introduced. The majority of them show positive results with a reduction in the number of injuries by 30 to 80%. However, there are still difficulties, in particular with the implementation of the prevention exercises, which in the future must be carried out with the cooperation of all structures that support sports at club, federation and school sports level as well as in sports and health policy. It is important that all supervising persons are convinced of the proven benefits of the early application of prevention exercises on health and performance in children and youth sports and that sports medicine science focuses even more on the evidence on prevention.

Influence of physical activity and sports training on obesity
26/05/2021
Link to the article. Thünenkötter T., Urhausen A. Einfluss von körperlicher Aktivität und sportlichem Training auf ÜbergewichtSports Orthop. Traumatol. 37, 18–25 (2021) https://doi.org/10.1016/j.orthtr.2020.11.009 For years, the prevalence of overweight and obesity has been increasing worldwide. Due to a variety of associated comorbidities, this represents a central challenge for the health care systems. The majority of the daily energy consumption of humans can be influenced by physical training. Endurance and strength training is recommended for weight reduction. This is one of the main focus of integrative treatment programs, along with the modification of nutrition and behavior. In an adipogenic environment, however, it is very difficult for most overweight and obese people to lose weight. Exercise, even without weight normalization, can help prevent overweight-associated diseases and thus reduce mortality. Physical activity, as a cost-effective intervention, has such a positive effect on health as hardly any other measure. For this reason, therapeutic efforts in overweight and obesity should not be aimed exclusively at weight reduction, but also and especially at increasing cardiorespiratory fitness.

Primary prevention of sports injuries and overuse
26/05/2021
Link to the article. Tischer T., Besenius E., Lutter C., Seil R. Primärprävention von Sportverletzungen und -schäden. Sports Orthop. Traumatol. 37, 4–9 (2021) https://doi.org/10.1016/j.orthtr.2021.01.011 Sport is an important part of our society and has far-reaching positive effects on our health. Unfortunately, some of these positive effects are lost again due to sports injuries. In the meantime, the evidence of prevention programs to avoid sports injuries in knee, hip, ankle and shoulder is well documented. The data is greatest for the knee joint, where up to 67% of anterior cruciate ligament injuries can be avoided in adolescents and young female adults. The shoulder is still the least studied area, where there are only a few randomized studies, but which could also show a significant reduction in injuries. Thus, the main challenge is to implement prevention programs in the daily training of athletes, while at the same time improving the registration of sports injuries and the training of all players. In the future, new technologies (sensors, artificial intelligence) will certainly play an important role.

Paperjam article : 'The stride analysed by 3D analysis'
25/05/2021
Link to the article Title: La foulée décortiquée par une analyse 3D by Prof. Dr. Jan Cabri in Paperjam on May 20th 2021 For the past year, the CHL has offered a laboratory for the analysis of movement in 3 dimensions. A godsend for runners, who are sometimes unaware of the source of the injuries that too often bring them to stop running. In running, chronic or overload injuries are frequent. And without seeing the patient in action, it is sometimes difficult for a doctor to determine the cause. Often, it is linked to the way of running or to a malformation, which can be benign but disabling in the long run. To overcome this problem, the Luxembourg Institute of Research in Orthopedics, Sports Medicine and Science (LIROMS) has set up the Human Motion Laboratory. "This laboratory has existed for about ten years," explains Professor Jan Cabri, Scientific Director at LIROMS. "But in the last year we have equipped it with three-dimensional motion analysis technology to analyse walking and running."
Webinar: What's new in orthopaedic surgery?
25/05/2021
Link to the video What's new in orthopaedic surgery? Languages: French and German Program: - Introduction - Prof. Dr Romain Seil- Introduction to the department - Dr Caroline Mouton- Foot tendinopathies - Dr Nicolien VanGiffen- Ankle and shoulder instability: current developments - Dr Pietro Spennacchio- Ligamentous injuries of the knee - Prof.. Dr Romain Seil- Degenerative meniscus damage - Dr Christophe Jacquet- Misalignment of the legs - Prof. Dr Dietrich Pape- Minimally invasive prosthetic surgery - Dr Victor David- Surgery for infections and prosthesis revisions - Dr Alexander Hoffman- General discussion

High incidence of previously neglected meniscus lesions influencing knee biomechanics in association with ACL injuries - Virtual 19th ESSKA Congress
19/05/2021
Video from the Virtual 19th ESSKA Congress 11-15 May 2021 CHL / LIROMS / LIH Caroline MOUTON, Amanda MAGOSCH, Christian NÜHRENBÖRGER, Romain SEIL

High number of ACL injuries after the summer break in team ball sports - Virtual 19th ESSKA Congress
18/05/2021
Presentation at the Star paper session of the Virtual 19th ESSKA Congress. This presentation was selected amongst the 5 best abstracts from 2000 abstract submissions at the ESSKA Congress. CHL / LIROMS / LIH C.Mouton, A. Gokeler, A. Urhausen, C. Nührenbörger, R. Seil

Incidence and risk factors for residual high-grade pivot shift after ACL reconstruction with or without a lateral extra-articular tenodesis
11/05/2021
Link to the article Jacquet, C., Pioger, C., Seil, R., Khakha, R., Parratte, S., Steltzlen, C., Argenson, J.-N., Pujol, N., & Ollivier, M. (2021). Incidence and Risk Factors for Residual High-Grade Pivot Shift After ACL Reconstruction With or Without a Lateral Extra-articular Tenodesis. Orthopaedic Journal of Sports Medicine. https://doi.org/10.1177/23259671211003590 Background: Residual rotatory knee laxity at midterm follow-up after isolated anterior cruciate ligament reconstruction (ACLR) versus ACLR with lateral extra-articular tenodesis (LET) remains an issue. Purpose/Hypothesis: To evaluate the outcomes of ACLR with or without additional LET at a minimum 2-year follow-up in patients with preoperative high-grade pivot shift (PS). Our hypothesis was that the addition of LET would decrease the risk of secondary meniscal injury and the presence of residual high-grade PS at follow-up. Study Design: Cohort study; Level of evidence, 3. Methods: A retrospective analysis performed at 3 sports medicine centers identified 266 study patients; all had a high-grade PS (grade 2 or 3) preoperatively and underwent isolated ACLR with or without LET. Four different ACLR techniques were used: single-strand quadrupled semitendinosus (ST4) ACLR without LET (ST4 group; n = 55), ST4 with anatomic LET (ST4+LET group; n = 77), bone–patellar tendon and modified Lemaire LET (BTB+LET group; n = 43), and quadriceps tendon and modified Lemaire LET (QT+LET group; n = 91). At follow-up, we evaluated for the presence of high-grade (grade ≥2) PS. Preoperative meniscal tears and their treatment were recorded. Results: Overall, 185 (69.5%) patients had at least 1 meniscal tear at index surgery. The mean follow-up period was 44.3 months; 47 (17.7%) patients had a new meniscal tear and 64 (24%) patients had a high-grade PS at follow-up. Compared with meniscal repair, significant predictors for high-grade PS at follow-up were meniscectomy (odds ratio [OR] = 2.65 [95% CI, 1.19-5.63]; P = .02) and nonrepair of preoperative meniscal tear (OR = 3.26 [95% CI, 1.27-9.43]; P = .007). The appearance of a new symptomatic meniscal tear was the strongest significant predictor of high-grade PS at follow-up (OR = 4.31 [95% CI, 2.31-8.06]; P < .001). No significant correlation was observed between the addition of LET and the presence of high-grade PS at follow-up. Conclusion: In the current study, 1 in 4 patients with high-grade PS before ACLR with or without LET was at risk of residual rotatory knee laxity at mean 44-month follow-up, regardless of the technique used. Repairing a pre-existing meniscal lesion was more effective than performing LET to decrease the presence of a high-grade PS at follow-up.

The knee in elite sport
03/05/2021
Keynote lecture during the German Sports, Medicine and Health Summit 2021 about the knee in elite sport by Prof. Dr. Romain Seil.
The future of meniscus science: international expert consensus
28/04/2021
Link to article DePhillipo N.N., LaPrade R.F., Zaffagnini S., Mouton C., Seil R., Beaufils P. . The future of meniscus science: international expert consensus. J EXP ORTOP 8, 24 (2021). https://doi.org/10.1186/s40634-021-00345-y Purpose. The purpose of this study was to evaluate the main focus areas for research and development for furthering the state of meniscus science in 2021. Methods. An electronic survey including 10 questions was sent in a blind fashion to the faculty members of the 5th International Conference on Meniscus Science and Surgery. These faculty served as an expert consensus on the future of research and development areas of meniscus science. Survey responses were analyzed using descriptive statistics and ranking weighted averages were calculated to score survey questions. Results. Of the 82 faculty, 76 (93%) from 18 different countries completed the survey (84% male, 16% female). The highest ranked future research and development focus areas were meniscus repair, biologics, osteotomy procedures, addressing meniscus extrusion, and the development of new therapies for the prevention of posttraumatic osteoarthritis. Currently, the most ‘valuable’ type of biologic reported for meniscus treatment was platelet-rich plasma. The main reported global research limitation was a lack of long-term clinical outcomes data. The most promising emerging medical technologies for improving meniscus science were 3-D printing, personalized medicine, and artificial implants. Conclusions. This survey suggests that the future of meniscus science should be focused on meniscal preservation techniques through meniscus repair, addressing meniscal extrusion, and the use of orthobiologics. The lack of long-term clinical outcomes was the main reported research limitation globally for meniscus treatment. Future product development utilizing emerging medical technologies suggest the use of 3-D printing for meniscal transplants/scaffolds, personalized treatment, and bioengineering for artificial implants.

Paperjam article: 'Orthopaedic insoles: the last chance'
28/04/2021
Link to the article Title: LE BON GESTE: Semelles orthopédiques: le dernier recours By Prof Dr Jan Cabri in Paperjam on 8 April 2021 More and more runners are using orthopaedic insoles to correct their movement. But the debate about their effectiveness is still ongoing. For Professor Jan Cabri (Liroms), their effectiveness is often unproven.
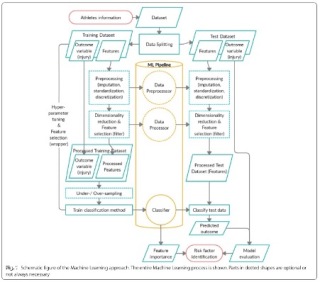
Machine learning methods in sport injury prediction and prevention: a systematic review
21/04/2021
Link to the article Van Eetvelde, H., Mendonça, L.D., Ley, C.,Seil R.and Tischer T. Machine learning methods in sport injury prediction and prevention: a systematic review. J EXP ORTOP 8, 27 (2021). https://doi.org/10.1186/s40634-021-00346-x Injuries are common in sports and can have significant physical, psychological and financial consequences. Machine learning (ML) methods could be used to improve injury prediction and allow proper approaches to injury prevention. The aim of our study was therefore to perform a systematic review of ML methods in sport injury prediction and prevention. Methods: A search of the PubMed database was performed on March 24th 2020. Eligible articles included original studies investigating the role of ML for sport injury prediction and prevention. Two independent reviewers screened articles, assessed eligibility, risk of bias and extracted data. Methodological quality and risk of bias were determined by the Newcastle–Ottawa Scale. Study quality was evaluated using the GRADE working group methodology. Results: Eleven out of 249 studies met inclusion/exclusion criteria. Different ML methods were used (tree-based ensemble methods (n = 9), Support Vector Machines (n = 4), Artificial Neural Networks (n = 2)). The classification methods were facilitated by preprocessing steps (n = 5) and optimized using over- and undersampling methods (n = 6), hyperparameter tuning (n = 4), feature selection (n = 3) and dimensionality reduction (n = 1). Injury predictive performance ranged from poor (Accuracy = 52%, AUC = 0.52) to strong (AUC = 0.87, f1-score = 85%). Conclusions: Current ML methods can be used to identify athletes at high injury risk and be helpful to detect the most important injury risk factors. Methodological quality of the analyses was sufficient in general, but could be further improved. More effort should be put in the interpretation of the ML models.

Paperjam article: 'And suddenly it's a cramp!'
29/03/2021
Link to the article Title: LE BON GESTE: Et soudain, c’est la crampe! By Prof Dr Jan Cabri in Paperjam on 14 January 2021 We may be well prepared, but a cramp can spoil a performance in competition. Can it be prevented and avoided?

Winner of the Best Original Article Award in the JISAKOS Best Article competition.
19/03/2021
Link to the award winning article Ardern CL, Ekås G, Grindem H, et al. 2018 International Olympic Committee consensus statement on prevention, diagnosis and management of paediatric anterior cruciate ligament (ACL) injuriesJournal of ISAKOS: Joint Disorders & Orthopaedic Sports Medicine 2018;3:66-82. Hearty congratulations to the authors for being honoured as the winner of the Best Original Article Award in the JISAKOS Best Article competition selected by the Journal of ISAKOS (JISAKOS) Editorial Board and the ISAKOS Board of Directors. The article was entitled '2018 International Olympic Committee Consensus Statement on Prevention, Diagnosis and Management of Paediatric Anterior Cruciate Ligament (ACL) Injuries'. The Best Article competition was conducted as part of the celebration of ISAKOS 25th Anniversary and the JISAKOS 5th Anniversary. The authors have been invited to join at the 13th Biennial Congress in Cape Town, South Africa where the article will be recognized during the session titled 'How to get Published in The Journal of ISAKOS: Editor's Tips for Maximizing Your Journal Submissions' on Monday, November 29, 2021 at 10:30-11:15 am. Authors who attend the session also will receive a certificate of recognition as well as a cash award from the Journal of ISAKOS.
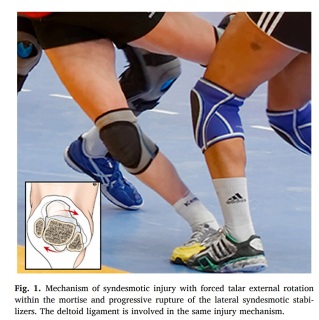
Diagnosing instability of ligamentous syndesmotic injuries: A biomechanical perspective. Review published in Clinical Biomechanics
18/03/2021
Link to the article Spennacchio P., Seil R., Gathen M., Cucchi D. Diagnosing instability of ligamentous syndesmotic injuries: A biomechanical perspective, Clinical Biomechanics, Volume 84, 2021, 105312, ISSN 0268-0033, https://doi.org/10.1016/j.clinbiomech.2021.105312. Highlights Different experimental setups available to investigate syndesmotic stability.. Ex vivo models: significant kinematic role of anterior inferior tibiofibular ligament.. Isolated anterior inferior tibiofibular ligament lesion can cause dynamic instability.. Suspected syndesmotic instability: 2nd level diagnostics, minimize risk for sequelae.. Computed tomography can improve the diagnosis of syndesmotic instability.. Abstract Background: High ankle sprains are insidious injuries associated with a long recovery period, functional impairment and long-term sequelae if mistreated. This systematic review investigates the biomechanical knowledge on the kinematic consequences of sequential syndesmotic ligamentous injuries, aiming to furnish an updated and objective contribution for the critical appraisal and further elaboration of current diagnostic algorithms for high ankle sprains. Methods: A systematic review was performed to identify human biomechanical studies evaluating the stabilizing role of the syndesmotic ligaments. Special attention was paid to identify the smallest lesion within the progressive simulated injuries able to provoke statistically significant changes of the syndesmotic kinematic on the specimen, the mechanical solicitation that provoked it, and the measurement methodology. Findings: Fourteen studies were included. In eight articles already an isolated injury to the anterior inferior tibiofibular ligament provoked significant changes of the syndesmotic kinematic, which was always depicted under an external rotation torque. In three articles an isolated deltoid ligament injury provoked significant changes of the syndesmotic kinematic. Four articles described a direct measure of the bony movements, whereas seven collected data through conventional radiography or CT-scan imaging and three via a 3D motion analysis tracking system. Interpretation: An isolated lesion of the anterior inferior tibiofibular ligament can provoke significant kinematic modifications in ex vivo syndesmotic models and may be responsible of subtle patterns of dynamic instability, regardless of further syndesmotic ligamentous injuries. The data observed support efforts to define reliable CT imaging parameters to improve non-invasive diagnostic of subtle forms of syndesmotic instability.
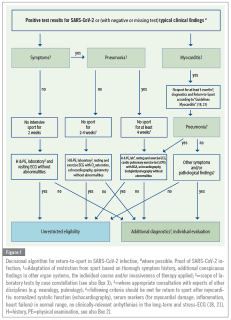
Video recording of the lecture: 'Return to sport after Covid 19' by Prof Urhausen
05/03/2021
The conference/webinar on 'The Management of Post Covid 19 Patients' was held on Wednesday, March 3, 2021, online and in person. It was organized by the CHL in collaboration with the Society of Medical Sciences of the Grand Duchy of Luxembourg. Prof Dr Axel Urhausen was invited to present his lecture on 'Return to sport after Covid 19' . The overall programme can be assessed at https://www.chl.lu/fr/actualites/videos-conference-prise-en-charge-des-patients-post-covid-19 The video recording of the conference can be assessed at https://vimeo.com/showcase/8211358/video/519810335
Ramp lesions are six times more likely to be observed in the presence of a posterior medial tibial bone bruise in ACL‑injured patients: Publication in KSSTA
04/03/2021
Link to the publication Beel W, Mouton C, Tradati D, Nührenbörger C, Seil R. Ramp lesions are six times more likely to be observed in the presence of a posterior medial tibial bone bruise in ACL-injured patients. Knee Surg Sports Traumatol Arthrosc. 2021 Mar 4. doi: 10.1007/s00167-021-06520-z. Epub ahead of print. PMID: 33661324. Abstract Purpose: The aim of this study was to determine whether posterior tibial slope (PTS), meniscal slope (MS), and bone bruise pattern (BBP), as observed on magnetic resonance imaging (MRI), differed between patients with or without medial meniscus ramp lesions at the time of anterior cruciate ligament reconstruction (ACLR). The hypothesis was that patients with a ramp lesion had a higher PTS and MS, with a different BBP than patients without a ramp lesion. Methods: Fifty-six patients undergoing ACLR were selected from an in-house registry and separated into 2 groups: (1) the RAMP group included patients with a primary ACLR and a medial meniscus ramp lesion diagnosed intraoperatively; (2) the CONTROL group included patients with a primary ACLR without ramp lesion after arthroscopic exploration of the posteromedial knee area. The two groups were matched for age, sex and type of concomitant meniscal lesions. The medial/lateral-PTS/MS and BBP were subjected to blinded evaluation on the preoperative MRI of the reconstructed knee. Results: Twenty eight patients (21 males; 7 females) were included in each group. No significant difference could be observed between groups in terms of demographical characteristics, PTS, and MS. A posteromedial tibial plateau (PMTP) bone bruise was more often observed in the RAMP group (n = 23/28) compared to the CONTROL group (n = 12/28) (p < 0.01). The RAMP group was 6.1 (95%CI [1.8; 20.8]) times more likely to present a PMTP bone bruise. The likelihood of having a bone bruise in both the medial and lateral compartments was 4.5 (95%CI [1.2; 16.5]) times higher in the RAMP group. However, a BBP only involving the lateral tibiofemoral compartment was more likely to be observed in the CONTROL group (n = 10/28) compared to the RAMP group (n = 3/28, p < 0.05 - odds ratio 4.6 (95%CI [1.1; 19.2]). Conclusion: Ramp lesions were 6.1 and 4.5 times more likely to be observed in the presence of a posteromedial tibia plateau bone bruise or a combined bone bruise respectively in both the medial and lateral tibiofemoral compartment in patients undergoing ACLR. The tibial and meniscal slopes did not differ between patients with or without ramp lesions undergoing ACLR. Level of evidence: Level III. Keywords: ACL reconstruction; Bone bruise; Meniscal slope; Posterior tibial slope; Ramp lesion.
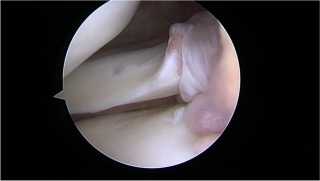
The aspiration test: an arthroscopic sign of lateral meniscus posterior horn instability. Publication in JEO
02/03/2021
Link to the publication Jacquet, C., Magosch, A., Mouton, C. et al. The aspiration test: an arthroscopic sign of lateral meniscus posterior horn instability. J EXP ORTOP 8, 17 (2021). https://doi.org/10.1186/s40634-021-00327-0 The suspensory mechanism of the posterior part of the lateral meniscus is an anatomically complex structure which allows its mobility, essential to the kinematics of the knee. Damage to this structure (either through knee trauma or congenital abnormalities) can result in an instability of the lateral meniscus that may lead to lateral knee pain, locking sensations or lack of rotational control of the knee. Currently, there are no reliable clinical or imaging tests to identify this pathology and the diagnosis of lateral meniscus instability is often delayed or missed The authors of this study propose a novel method for a quick and easy arthroscopic screening test (called the aspiration test) to help surgeons to identify this instability of the lateral meniscus The description of this test is important in order to improve its diagnosis and to allow for complete anatomical repair when indicated.
Best young researcher award at ReFORM- won by Amanda Magosch
28/02/2021
ReFORM Amanda Magosch from LIROMS won the award for the best young researcher in an online conference organized by ReFORM, the French consortium for sports health research recognized by the International Olympic Committee along with another researcher. This consortium includes the National Sports Institute of Montreal, the University of Liège, the University of Geneva, INSEP in Paris and us. The centres had selected their 11 best researchers, for the occasion. The title of Amanda's presentation was: "On the road to knee rotary instability". Her work involved a clinical examination called "pivot shift" that we routinely perform under general anesthesia before any surgery for the anterior cruciate ligament of the knee. In more than 300 patients, she was able to identify 3 variables associated with the degree of rotary instability, namely age at the time of injury, accident-surgery interval and extent of associated meniscal lesions. This is the first time these associations have been described in the literature. They are important to refine our understanding of the extent of lesions and the therapeutic approach in these patients and to improve their long-term prognosis, including physical activity and the development of osteoarthritis of the knee. The results are currently being published. The fact that Ms. Magosch was awarded this award is a testament not only to the importance of the results to the international scientific community, but also to an excellent talent in a young medical student and the right entourage by our various clinical and scientific teams. We wish her the very best in her endeavours.

ReFORM PhD days scientific contribution
26/02/2021
Two of our PhD-students were invited to represent LIROMS at the first "Young Researcher Day“ organized by ReFORM. Anouk Urhausen described her ongoing project on the 10-year follow-up of the Delaware-Oslo ACL Cohort Study. Amanda Magosch presented the results of a study on factors associated with the Pivot Shift signs, a clinical test for rotational instability in the ACL-insufficient knee Joint. The findings that age at injury, time from injury to surgery and amount of meniscus damage were are associated with rotational laxity are new, especially with respect to the meniscus damage. In the end, Amanda was awarded for the best presentation along with one other presenter.

Video recording of the webinar: Biomechanical analysis of running performance
03/02/2021
On 20 January 2021, a sports medical webinar on "Biomechanical assessment of running performance" by P. Gette, R. Krecké, and Prof J. Cabri, PhD (LIROMS/CHL/LIH, Luxembourg) was held virtually over Zoom attended by 100 participants. A video recording of the talk is now available.

Influence of physical activity and sports training on obesity: Review/ Special Issue in Sports Orthopaedics and Traumatology
01/02/2021
Link to the article Summary For years, the prevalence of overweight and obesity has been increasing worldwide. Due to a variety of associated comorbidities, this represents a central challenge for the health care systems. The majority of the daily energy consumption of humans can be influenced by physical training. Endurance and strength training is recommended for weight reduction. This is one of the main focus of integrative treatment programs, along with the modification of nutrition and behavior. In an adipogenic environment, however, it is very difficult for most overweight and obese people to lose weight. Exercise, even without weight normalization, can help prevent overweight-associated diseases and thus reduce mortality. Physical activity, as a cost-effective intervention, has such a positive effect on health as hardly any other measure. For this reason, therapeutic efforts in overweight and obesity should not be aimed exclusively at weight reduction, but also and especially at increasing cardiorespiratory fitness. Keywords Fitness, Overweight, Obesity, SportsTraining, Cardiorespiratory fitness Thomas Thünenkötter, Axel Urhausen (2021) Einfluss von körperlicher Aktivität und sportlichem Training auf Übergewicht, Sports Orthopaedics and Traumatology, 2021, ISSN 0949-328X, https://doi.org/10.1016/j.orthtr.2020.11.009.

ESSKA Newsletter Dec 2020
15/12/2020
Read the latest news from ESSKA in the December issue of their quarterly newsletter. View it in a user-friendly online version as well as the traditional PDF version which can be downloaded to read offline. In this issue, there are a number of interesting articles, including: 3. ESSKA President Jacques Menetrey’s Editorial: News from the Society4. 19th ESSKA Congress GOES VIRTUAL - 11-15 May 202110. Tips and Tricks for Young Reviewers14. Pillar of ESSKA: Romain Seil18. ESSKA Sections looking forward to 202127. ESSKA Speciality Days - 3-4 September 2021 in Warsaw, Poland35. ESSKA Webinars scheduled for 2021-202248. 2020 update of Medial meniscus ramp lesions; difficult to diagnose but vital to repair50. 3D Navigation Model for Diagnosis and Treatment of the Elbow Bony Impingement ...and much more!

Exclusive Interview of LIROMS President Prof Dr Romain Seil: "Pillars of ESSKA"
15/12/2020
ESSKA likes to honour individuals who they consider to be the "pillars" of the society. In the December 2020 quarterly online newsletter of ESSKA, an exclusive interview of LIROMS President, Prof Dr Romain Seil has been presented. Interviewed by Jaun Carlos Monllau. Read the interview here to catch a glimpse of Prof Seil's inspring career as well as his personal journey along the way!

2020 update of Medial Meniscus ramp lessions: published in ESSKA Newsletter
15/12/2020
In the December 2020 ESSKA Newsletter, an article co-authored by LIROMS President Prof Dr Romain Seil has been published. Titled as "2020 update of Medial Meniscus ramp lessions, difficult to diagnose but vital to repair". Link to the article here.

Updates on PAMI: published in ESSKA newsletter Dec 2020
15/12/2020
Latest news from Pediatric ACL Monitoring Inititiative (PAMI), co/authored by LIROMS President Prof Dr Romain Seil and LIROMS scientific collaborator Dr Caroline Mouton, published in ESSKA December 2020 newsletter. Link to the article here.
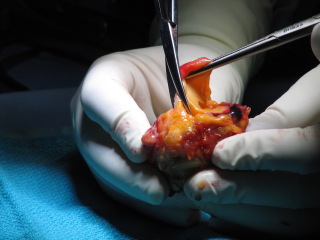
Surgical treatment of complex meniscus tear and disease: state of the art review
27/11/2020
Link to the publication Ozeki, N., Seil, R., Krych, A., & Koga, H. (2020, September 17). Surgical treatment of complex meniscus tear and disease: State of the art. Retrieved November 27, 2020, from https://jisakos.bmj.com/content/early/2020/09/17/jisakos-2019-000380 In collaboration with Tokyo Medical University, Japan, Mayo Clinic, USA and CHL, LIH and LIROMS, Luxembourg, a recent publication published in BMJ journals highlights the most modern and advanced techniques of meniscus preservation surgery (instead of resection). Dr Megha Agrawal was acknowldged in the manuscript for English editing.

Editorial in BJSM: The mission of ReFORM
26/11/2020
Link to the article Martens G, Edouard P, Tscholl P, et alDocument, create and translate knowledge: the mission of ReFORM, the Francophone IOC Research Centre for Prevention of Injury and Protection of Athlete HealthBritish Journal of Sports Medicine Published Online First: 12 November 2020. doi: 10.1136/bjsports-2020-103087 The International Olympic Committee (IOC) has supported athletes’ health protection by funding research centres dedicated to the prevention and treatment of sports-related injuries and illnesses. After establishing four centres in 2009, the IOC research centres network expanded to 9 institutions in 2014 and the 2019 round recognised 11 centres. In this editorial, the mission of ReFORM—an international French-speaking network of five institutions is discussed along with the focus areas, expertise and what makes ReFORM unique.

A warm-up before jogging: useful or not? Prof Dr Jan Cabri discusses
12/11/2020
https://paperjam.lu/article/echauffement-avant-jogging-uti
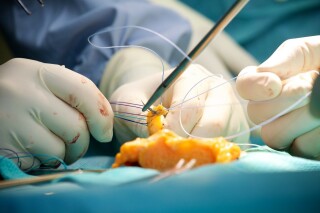
Publication: Medial meniscus ramp and lateral meniscus posterior root lesions are present in more than a third of primary and revision ACL reconstructions
09/11/2020
Link to the article This study identified concomitant meniscal lesions in two thirds of all ACL reconstructions. Fifty in ACL-injured knees and an improved understanding of ACL injury mechanisms. 50 percent of them involved the biomechanically relevant, but previously often undiagnosed lesions of the medial meniscus ramp or the lateral meniscus posterior root. These findings highlight the need for a thorough and systematic inspection of the menisci. Magosch, A., Mouton, C., Nührenbörger, C. et al. Medial meniscus ramp and lateral meniscus posterior root lesions are present in more than a third of primary and revision ACL reconstructions. Knee Surg Sports Traumatol Arthrosc (2020). https://doi.org/10.1007/s00167-020-06352-3

The Meniscus Congress postponed to January 12th-15th 2022
29/10/2020
Unfortunately, the pandemic forced us to revise our plans for THE MENISCUS congress which was scheduled from January 27th – 30th 2021 in Luxembourg..

KSSTA Editorial Published, ‘From Meniscal resection to meniscal repair: a journey of the last decade’
29/10/2020
Authors: Roland Becker, Sebastian Kopf, Romain Seil, Michael T. Hirschmann, Philippe Beaufils, Jon Karlsson The last decade has shed some light on the darkness surrounding the treatment of meniscal injuries. A significant amount of work has been done in order to provide a more scientific approach to the treatment of the injured meniscus. Degenerative meniscal lesions and traumatic meniscal tears differ in terms of aetiology and pathology and require differentiated diagnostic algorithms and treatments. A new terminology has, therefore, been defined by the ESSKA meniscus concensus project. A traumatic meniscal tear is caused by an acute and sufficiently serious trauma to the knee. In contrast, a degenerative meniscal lesion occurs due to repetitive minor injuries and lacks a sufficiently serious single trauma. This editorial shows that the scope of the meniscus repair is greater than before and there is still a need for both more basic scince and clinical research in order to identify the best practice when treating different meniscal pathologies. Link: https://link.springer.com/article/10.1007/s00167-020-06316-7

Release of the book on ‘Primary prevention of sports injuries’ after the success of GOTS Expert meeting 2019 in Luxembourg
15/10/2020
In close collaboration with LIROMS, the German-speaking Orthopaedic and Traumatologic Society of Sports Medicine (GOTS) has continued the successful tradition of its expert meetings, which started in 2010.. At the 6th edition of GOTS expert meeting from 19-22 September 2019, in Canach (Luxembourg), organized under the direction of GOTS president Prof. Romain Seil, a group of 30 specialists from Austria, Belgium, Germany, Luxembourg, Norway, Switzerland, and The Netherlands, discussed the current status of primary prevention of sports injuries and illnesses. The majority of the experts were orthopaedic surgeons, but also sports scientists and physiotherapists, as well as German health insurance companies, were involved.

LIROMS recognized by the International Olympic Committee as one of the five partners of the French-speaking Sports Medicine Research
13/10/2020
We are proud to announce that LIROMS has been recognized by the International Olympic Committee as one of the five partners of the French-speaking Sports Medicine Research Network. ReFORM: Réseau Francophone Olympique de la Recherche de Médecine du sport (formerly known as FReNAHP2).

The 1st virtual Qualisys User Group Meeting took place on October 8th, 2020.
09/10/2020
Qualisys users across Central Europe gathered at the virtual “Hopin” venue to share their work and experience on the topic ”Using motion capture to benefit researchers, clinicians and coaches – today and in the future”. LIROMS representatives were amongst invited speakers for the session entitled “Functional Assessment”. Presentations covered the state of play in scientific and field-based motion capture approaches for athletes, coaches and medical teams working with them to assess athlete’s health and performance status. The panel discussion fostered in-deep conversations amongst peers, pinpointing current challenges and future opportunities of available and rising technologies. The LIROMS contribution was rewarded with positive echo and a burst of recurrent exchanges throughout the rest of the day in the event’s chat rooms. Honored by the invitation, the LIROMS team thanks the event organizers and attendees for this outstanding session. Link: https://www.qualisys.com/events/qualisys-virtual-user-group-meeting-dach/

The first annual workshop for the Pediatric Anterior Cruciate Ligament Initiative (PAMI), 2nd Oct 2020, organized by ESSKA.
03/10/2020
The aim of the workshop was to gather PAMI partners as well as interested institutions to discuss the organisational aspects and the future perspectives of the initiative. The PAMI aims to collect and analyse data from orthopaedic surgeons who are treating children and adolescents with anterior cruciate ligament (ACL) injury using an international data collection system. Through this initiative, the goal is to improve diagnosis, treatment options, surgical techniques and rehabilitation of pediatric ACL injuries. Presented during the ESSKA conference in Glasgow in May 2018, the ESSKA leadership has placed PAMI under the lead of its Basic Science Committee chaired by Caroline Mouton since May 2020. Currently, 6 partner institutions from Austria, Italy, Luxembourg, Netherlands Norway, and Spain are actively enrolling patients. Since the first inclusion in October 2018, 68 children have been recruited with a continuous increase of inclusion within the last months. The first data shows that the chronological age at injury for this population was in average 12 years of age (from 6 to 17 years of age). Most injuries occurred while playing football (38%). At the time of the analysis, 69% were indicated for surgery. While several developments were made in the last months to enhance data quality and user’s experience with the PAMI web portal, the preliminary analyses allowed the PAMI steering committee to highlight some technical issues in data consistency, accuracy and completeness. These issues will be specifically targeted within the next months to consolidate the database and provides efficient guidelines to PAMI partners. In 2021, the PAMI managers will also start to provide yearly feedbacks to partner institutions on their data in order to ensure the quality of data and to officially publish the first results of the PAMI. Next years will be critical for the PAMI. A request to extend the ethical approval of the project as well as financial supports is foreseen, which also gives the opportunity to evaluate and strengthen the current initiative. During the workshop, inclusion/exclusion criteria were discussed again as well as the possibility to extend the content of data gathered within the project. Please be aware that we are still looking for interested partner institutions to join us. If you are an orthopaedic surgeon or a medical doctor treating children and adolescents with ACL injury and are interesting in the PAMI, please contact us at pami@esska.org. We will keep you aware of our next workshop and symposium that we hope to be able to organise during the next ESSKA congress in Milano. Detailed information on how to become a PAMI partner is available online on the ESSKA platform; https://www.esska.org/general/custom.asp?page=PAMI Thanks to the following partners: Smith and Nephew, International Olympic Committee, Luxemburgish Olympic committee, Luxembourg Institute of Health

A Comparison of the Energetic Cost of Running in Marathon Racing Shoes
Wouter Hoogkamer, Shalaya Kipp, Jesse H. Frank, Emily M. Farina, Geng Luo & Rodger Kram Link to the article Abstract. Background. Reducing the energetic cost of running seems the most feasible path to a sub-2-hour marathon. Footwear mass, cushioning, and bending stiffness each affect the energetic cost of running. Recently, prototype running shoes were developed that combine a new highly compliant and resilient midsole material with a stiff embedded plate. Objective. The aim of this study was to determine if, and to what extent, these newly developed running shoes reduce the energetic cost of running compared with established marathon racing shoes. Methods. 18 high-caliber athletes ran six 5-min trials (three shoes × two replicates) in prototype shoes (NP), and two established marathon shoes (NS and AB) during three separate sessions: 14, 16, and 18 km/h. We measured submaximal oxygen uptake and carbon dioxide production during minutes 3–5 and averaged energetic cost (W/kg) for the two trials in each shoe model. Results. Compared with the established racing shoes, the new shoes reduced the energetic cost of running in all 18 subjects tested. Averaged across all three velocities, the energetic cost for running in the NP shoes (16.45 ± 0.89 W/kg; mean ± SD) was 4.16 and 4.01% lower than in the NS and AB shoes, when shoe mass was matched (17.16 ± 0.92 and 17.14 ± 0.97 W/kg, respectively, both p < 0.001). The observed percent changes were independent of running velocity (14–18 km/h). Conclusion. The prototype shoes lowered the energetic cost of running by 4% on average. We predict that with these shoes, top athletes could run substantially faster and achieve the first sub-2-hour marathon.
